Melissa Mazor, PhD, RN1; Daniel David, PhD, RN2; Dolores Moorehead, MS, APCC3; John D. Merriman, PhD, RN2; Jenny J. Lin, MD, MPH1
1Department of Medicine, Icahn School of Medicine at Mount Sinai, New York, NY;
2Rory Meyers College of Nursing, New York University, New York, NY;
3Women’s Cancer Resource Center, Berkeley, CA
Background: Little is known about the role of community-based navigation in supportive care delivery for historically marginalized cancer survivors. The purposes of this study were to evaluate supportive care experiences of low-income Black and Latina cancer survivors and examine the care role of their community navigator.
Methods: Semistructured interviews with Black and Latina cancer survivors (n = 10) and navigators (n = 4) from a community-based organization for low-income women were conducted and qualitatively evaluated using content analysis.
Results: Content analysis yielded 6 themes that described the supportive care experience over time and before and after navigator support. When navigating supportive care alone, the themes were: (1) internal and external influencers, (2) alone and just surviving, and (3) feeling overwhelmed and distressed. When community navigator delivered supportive care, the themes were: (1) establishing trust and safety, (2) accepting multidimensional navigator-assisted supportive care management, and (3) distress alleviation.
Conclusions: Low-income Black and Latina women with cancer reported internal strength yet endured cancer care alone leading to a feeling of distress. Subsequently, community navigators provided patient-centric, supportive care and alleviated physical and emotional distress. These findings highlight the importance of increasing awareness of and linkage to community navigators, who may be able to meet the supportive care needs of diverse patient populations.
Black and Latina women with cancer experience disparities in supportive care delivery and outcomes,1,2 an understudied area of health equity. Given improvement in targeted therapies, cancer patients have increased survival3 but contend with challenging and often unaddressed supportive care needs, including pain and psychosocial distress.1,4 For low-income women of color, consequences of structural racism and social determinants of health may impede awareness of and access to supportive care.5,6 For example, poverty and isolation may diminish social networks that would normally support access to emotional and financial care.7 Hence, physical, psychological, socioemotional, and practical supportive care needs are often inadequately addressed and managed among Black and Latina cancer survivors.8
Cancer patient navigation was developed to address barriers related to social determinations of health and improve cancer care access and outcomes for low-income, racial, and ethnic minority patients.9 A navigator is a patient advocate who provides support to patients and assists them in overcoming barriers throughout their cancer trajectory.10 The role of a navigator can be filled by a nurse, social worker, health educator, or lay person and varies widely across settings and educational background of the navigators.11 In the context of this paper and in line with the foundation of navigation for structurally and historically marginalized paitients,9 a navigator is defined as a nonclinical employee of a community-based system who provides individual support to underserved patients with cancer and their families (ie, henceforth termed “community navigator”). Despite promising findings, the majority of navigation studies focus on screening and/or diagnostic resolution,12 and little is known regarding the role of community navigators in optimizing supportive care access and delivery for structurally marginalized cancer survivors across the cancer continuum.10,11,13
Given the persistent disparities in supportive care outcomes for Black and Latina women with cancer and the paucity of data examining the mechanisms by which navigators may mitigate these disparities, a further investigation into these experiences and processes is needed. The purpose of this study is to qualitatively evaluate how low-income Black and Latina women self-managed supportive care and investigate the subsequent role their community navigators played in their supportive care management. These findings will provide insight into the mechanisms by which navigators help underserved women with cancer manage their supportive care needs and may help identify target process measures and outcomes for future community-based navigational trials.
Methods
Design
Semistructured qualitative interviews were conducted with patients and community navigators as guided by descriptive qualitative design.14 The interviews were designed so that participants could answer open-ended questions and allow for opportunities to dive deeper and share experiences14 of supportive care before and after working with a community navigator (ie, trained and professionally employed lay navigator working at a community organization). Consolidated criteria for reporting qualitative research were applied to improve transparency and credibility of this study.15
Participants and Setting
Purposive sampling was used to recruit patients and navigators at a nonprofit community-based organization that provides free educational and exercise workshops, resources, and navigation for low-income women with cancer in the San Francisco Bay Area. The patients were eligible to participate if they: (1) had a history of cancer, (2) were >21 years of age, (3) were able to communicate in English, and (4) self-identified as Black and/or Latina. Navigators were eligible if they: (1) were >21 years of age, (2) were able to communicate in English, (3) self-identified as Black and/or Latina, and (4) worked as a community navigator for at least 1 year. Information about the study was posted through flyers, organizational newsletters, and staff dissemination of study information during community workshops. Individuals interested in the study notified a staff member at the community-based organization and provided their information to be contacted by the principal investigator (PI).
Data Collection
Individual 1-time semistructured interviews were conducted by a single interviewer with 10 years of clinical oncology nursing and qualitative research experience (MM) either in person in a private room at a community-based organization or over Zoom. The interviewer did not know the participants prior to participation in the research study. The interview protocol was reviewed with the community collaborators and co-authors and revised based on their feedback before starting the first qualitative interview. Interviews began with informed consent, followed by a short clinical and demographic survey. The interview questions were designed to elicit an in-depth description of the participants’ supportive care experiences from diagnosis to posttreatment survivorship, with an emphasis on before and after they connected with a community navigator. Community navigator interviews were designed to elicit their perspective of the supportive care needs and their ability to provide supportive care management within this population. Field notes were taken to supplement the transcripts and emphasize key common experiences. Interviews ranged from 60 to 75 minutes and were audiotaped, transcribed verbatim, and checked for accuracy.
The patient interview guide was divided among 3 domains: (1) getting to know you: culture, traditions, daily life, and activities; (2) supportive care experiences from diagnosis to survivorship; and (3) role of the navigator: in-depth description of supportive care delivery. The navigator interviews were designed to elicit feedback on patient supportive care needs and experiences and increase the credibility, validity, and trustworthiness of the findings. Data were collected until data saturation was reached (ie, no new themes or categories emerged from interviews)16 and sufficient depth of understanding of supportive care experiences before and after the navigator was reached.
Data Analysis
Data were analyzed using inductive content analysis.17,18 Audio recordings were transcribed verbatim by an institutional review board–approved independent transcription company. The PI checked the transcripts for accuracy and anonymity and uploaded them onto Dedoose. A 3-person coding team consisted of the PI, coinvestigator, and expert community provider. Text of each interview was read by all members of the coding team to gain an overall perspective of the participant’s experience. Initial codes were generated using the process of individual open coding. The team then convened to review their individual coding and reach agreement. Data analysis began during the first interview and was an iterative process; interpretations of data from previous interviews guided the subsequent interviews. Codes were collated into broader descriptive and interpretive themes.12 Themes and subthemes were reviewed by all authors to ensure consistency of interpretation and rigor of analysis.
Quality of the Data
Study and data quality and trustworthiness were enriched through investigator triangulation, member checking, audit trail, and debriefing with community peers.16 In addition, the PI met with an expert qualitative researcher (JJL) to review all findings, analysis, processes, and data interpretation. The varying perspectives of the 4 members (oncology nurse and researcher, palliative care nurse and researcher, physician with expertise in cancer survivorship, community-based client support clinician) enriched the analysis.
Ethics
This study was approved by the institutional review board (IRB-FY2020-3721). Written and verbal informed consent were obtained prior to participation.
Results
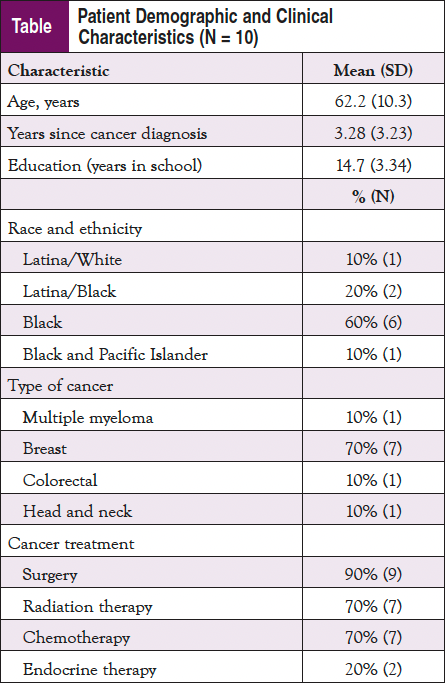
A total of 14 interviews were conducted with 10 patients and 4 community navigators between December 2019 and December 2020. Patients reported a mean (SD) age of 62.2 (10.3) years and were 3.28 (3.23) years from their cancer diagnosis. The majority had breast cancer (n = 7) and had completed their primary, active cancer treatment and were in posttreatment survivorship (n = 8). Regarding race/ethnicity, participants self-identified as Black (n = 6), Black and Pacific Islander (n = 1), Latina/White (n = 1), and Latina/Black (n = 2) (Table). Community navigators reported a mean (SD) age of 41.3 (10.8) years, had worked as a navigator for 12.3 (10.9) years, and self-identified as Black/African American (n = 2) and White/Latina (n = 2).
Four interviews were conducted at the community-based organization, and 10 interviews were conducted virtually over Zoom due to COVID precautions. Content analysis yielded 6 themes embedded within 2 categories that are described below in detail. The Figure shows the relationship between themes over time along with exemplary quotes.
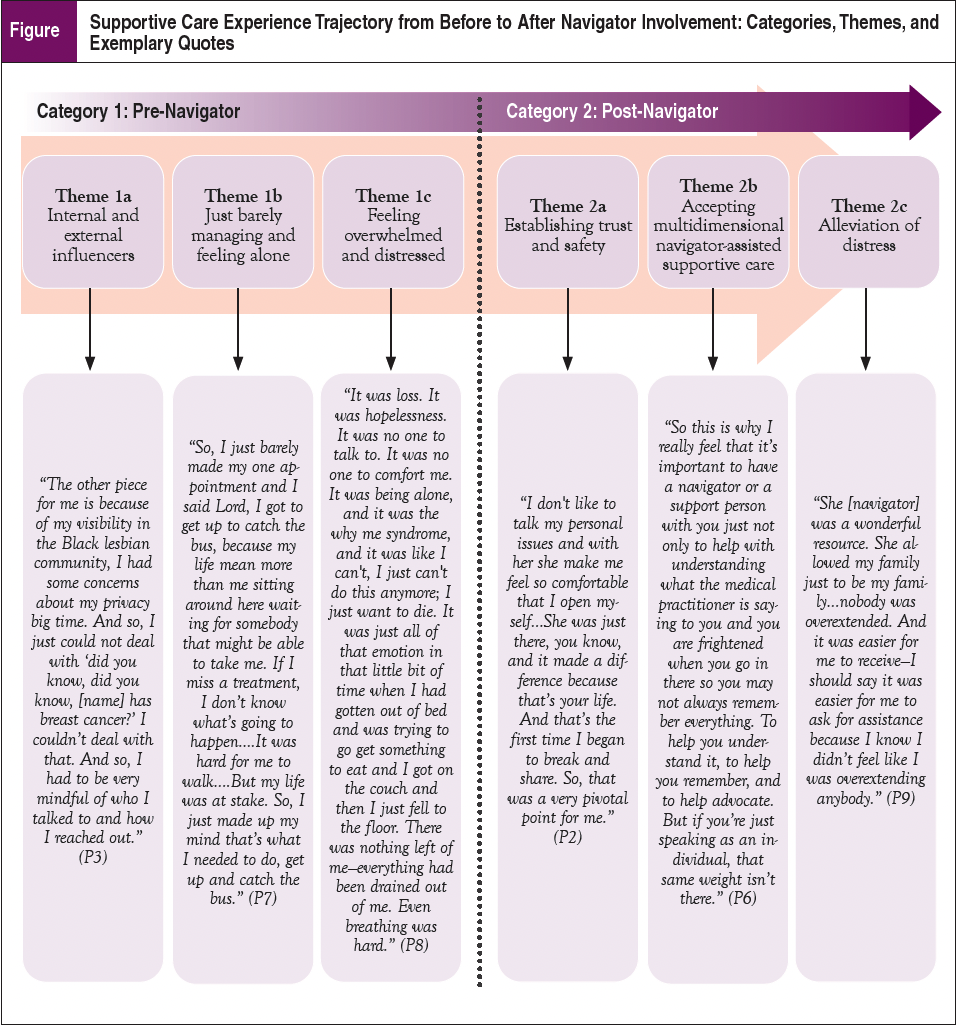
Category 1: Navigating Supportive Care “Alone”
This category embodies 3 themes describing factors related to survivors feeling alone while trying to take care of their supportive care needs. As described below in greater detail, the first theme describes antecedents to feeling alone; the second theme describes specific experiences and examples of navigating supportive care alone; and the third theme describes how survivors felt overextended, overwhelmed, and distressed after navigating their care alone.
Theme 1a: Internal and External Influencers of Navigating Supportive Care Alone
Most of the patients discussed how internal influencers such as past life circumstances and personal beliefs contributed to self-reliance, or a feeling that they could only count on themselves to address their supportive care needs. They described how they did not feel comfortable reaching out for help because they had repeatedly been let down or disappointed by others. For example, one participant discussed how she could not trust that others would be there for her, which led to her feeling she must be independent in her care.
“It’s just a disappointment of people letting me down basically my whole life. I just didn’t have maybe the courage or something, because like I said, I moved to this state by myself. I’ve been taking of care myself ever since I got here, so you kind of get in that mode.” (P5)
In addition to self-reliance, privacy was an important internal factor that made it challenging to reach out for support. More specifically, they found it challenging to both receive and/or accept supportive care by their clinical care team because of the importance of being private in their life. For one participant, she commented how her need for privacy was so powerful that she did not tell anyone about her diagnosis or treatment, which led to negative consequences in both her family and work life.
“After I got diagnosed, after 9 months nothing happened because I was in denial. I didn’t talk about it. I didn’t tell anybody. Only the doctor knew and that is it. I didn’t tell my husband….I’m very private in my life, and I used to go in my lunch time to get my chemo and I would get in trouble for coming 10 minutes late.” (P10)
Of note, this participant described how she was later fired from her position after being late returning to work over several days due to time conflicts with her infusion appointments.
External influencers also impacted how participants felt alone in navigating supportive care. In this context, participants described how both system- and provider-level interactions were delivered in a manner that felt discordant to their individual comfort levels. For example, communication around supportive care was often presented in a culturally insensitive manner.
“She [the oncologist] says, I’m sorry, I know you’re angry. I said I’m not angry. I’m scared. You know, and it’s that thing. Black women’s emotions, we’re mean or we’re angry, and I had to check her on that. I said I’m not angry.” (P3)
Of note, the navigators were aware of how these factors, such as implicit bias, contributed to a tendency of patients not wanting to follow up with their care. This point is succinctly described by one of the navigators.
“When racial discrimination is encountered by our patients, negative responses occur. Women lose faith in their care, become disillusioned, and avoid appropriate follow-up.” (N2)
Participants also discussed how external factors such as discordant hospital-based supportive services were oppositional to their individual and cultural preferences and thereby did not provide sufficient support for their supportive care needs. One participant explained how the care that was offered was personally offensive and made her feel disconnected from her care.
“In the hospital setting, and I don’t believe it’s just because it’s the hospital, it’s because her [the social worker] sense of checklist, it felt invasive. Surgeries never felt invasive, but that relationship felt more invasive than a true, genuine interest in me.” (P6)
Theme 1b: Alone and Just Surviving
As a result of these internal and external factors, patients felt they needed to self-manage all their supportive care needs. In most circumstances they were able to address these needs using their own internal strength, yet they expressed feeling alone throughout the process. For example, one participant discussed how it was upsetting to self-manage even the most basic postoperative supportive care needs such as getting a drink of water or food in her own home.
“So, I went through the surgery alone. Nobody was with me. I was in the hospital 5 days….I had 4 drain tubes, so she had to drain with the long needle, and I got poked all the time. I’m a pretty tough girl. But, when you come home, there’s nobody to hand you a glass of water or prepare you food. I lay there, and I said, ‘Gee, it pays not to be sick.’” (P8)
Participants also described how it was challenging to figure out the basics of finances and transportation that were essential to obtaining appropriate cancer care. One participant discussed how it took every ounce of energy and willpower to find transportation to her chemotherapy infusion appointment (see Figure for exemplary quote). In addition to self-managing transportation, patients described their struggles trying to manage financial needs, including paying for rent and food. One participant described how she coped with concurrently dealing with both cancer and financial needs.
“I shut down. I slept a lot. I had no idea what was going on or how severe it was... I started smoking pot. And I do smoke cigarettes. It was just—I don’t know. I was definitely f - - - this and f - - - that. I rented out a room in my apartment, so I would have some income coming in, but then also there would be somebody there in case anything should happen.” (P5)
Theme 1c: Overwhelmed and Distressed
Most patients described being so exhausted after having to self-manage their supportive care that they reached an emotional and physical nadir. For example, one participant described how she simply broke down after extensive multidimensional supportive care self-management.
"It was loss. It was hopelessness. It was no one to talk to. It was no one to comfort me. It was being alone, and it was the why me syndrome, and it was like I can’t, I just can’t do this anymore; I just want to die. It was just all of that emotion in that little bit of time when I had gotten out of bed and was trying to go get something to eat and I got on the couch and then I just fell to the floor. There was nothing left of me—everything had been drained out of me. Even breathing was hard.” (P8)
Many of the participants discussed how they would continue to move forward 1 step at a time but were completely physically and emotionally exhausted along the way.
Category 2: Community Navigator–Led Supportive Care
After being introduced to a community navigator, the participants’ supportive care experiences improved. Of note, all participants described how they met their navigator by chance rather than a systematic process of referral to navigation services. Examples of how they heard about the navigator included word-of-mouth and “walking by” in the neighborhood. The 3 themes in this category explain the process by which the navigator helped them better address their supportive care needs. The 3 themes include: (1) establishing trust and safety, (2) accepting multidimensional navigator-assisted supportive care management, and (3) distress alleviation.
Theme 2a: Establishing Trust and Safety
All participants discussed how trust and safety were foundational to being able to “accept” the navigator’s support. Trust and safety were established through feeling like the navigator cared about them as a person beyond just their cancer diagnosis. One participant discussed how her navigator not only looked like her but also treated her like a whole person.
“And so, one of the differences is looking like me. The other difference is communication style. Truly being interested in me rather than a checklist. I felt I have someone to lean on and take care of me and was really interested in my well-being, it wasn’t just her job. I really felt that from her.” (P3)
The navigators routinely reflect this essential aspect of establishing trust through empathy and holistic care.
Upon feeling safe, the participants were able to express their supportive care needs to the navigator, who subsequently could assist them through co-managing their care. This shift in acceptance of support is particularly poignant given that many of these participants previously discussed the importance of autonomy and privacy.
“I don’t like to talk about my personal issues, and with her she make me feel so comfortable that I open myself….She was just there, you know, and it made a difference because that’s your life. And that’s the first time I began to break and share. So, that was a very pivotal point for me.” (P2)
Theme 2b: Accepting Multidimensional Navigator-Assisted Supportive Care Management
After feeling safe, the participants discussed how they accepted and valued their navigator’s multidimensional care, including practical, physical, social, and emotional supportive care. Importantly, participants discussed how practical support, such as financial and food insecurity, needed to be addressed prior to initiating cancer treatment–related and/or other dimensions of supportive care. One participant mentioned how her navigator not only provided these types of practical resources but also accompanied her to social service appointments.
“Then it was very nice that she went with me to short disability office, permanent disability office, food stamp office, and when she saw that I was breaking out she will step in and help me and ask the good questions.” (P1)
Other common types of support included overcoming information and technology literacy challenges. For example, one participant discussed how her navigator helped her figure out how to look up trusted resources online.
“She know how to really look on the website and a specific question that I ask she will find it. I would get lost. If I put in the wrong question, they give me the wrong answer, but she [navigator] knows exactly what to ask and she finds things like this.” (P4)
All the participants discussed how much they valued their navigator’s social, emotional, and informational support through accompanying them to their oncology outpatient appointments. This aspect stood out as essential to maximize education and empowerment.
“So this is why I really feel that it’s important to have a navigator or a support person with you just not only to help with understanding what the medical practitioner is saying to you and you are frightened when you go in there so you may not always remember everything. To help you understand it, to help you remember, and to help advocate. But if you’re just speaking as an individual, that same weight isn’t there.” (P6)
Theme 2c: Distress Alleviation
Participants discussed how distress related to physical and psychological symptoms improved through work with the navigator. The navigators managed distress through teaching patients self-management techniques and recommending discussions with appropriate providers as needed. For example, one participant discussed how the symptom self-management techniques she learned from her navigator allowed her to be feel emotionally empowered.
“She would tell me to get a journal, write down what your symptoms are and then we’ll go over them. And then, from then on, I could just figure out what was going on.” (P2)
Participants also described how psychosocial distress improved through just knowing the navigator was there to help them.
“I see her, and I feel peace….All that stuff is super important because I'm very private. I feel whole, more relaxed and then I don’t have to burden my kids with my emotions. My kids are, they can listen to me but they’re young. They should not hear my crap, the stress when they have their own stress. It really helped me because every time I’m here with [navigator] I got very happy home.” (P7)
Importantly, these elements of navigational support not only alleviated personal but also family distress.
“She [navigator] was a wonderful resource. She allowed my family just to be my family…nobody was overextended. And it was easier for me to receive—I should say it was easier for me to ask for assistance because I know I didn’t feel like I was overextending anybody.” (P9)
Discussion
Main Findings
These findings provide often unheard descriptions of supportive care experiences of low-income Black and Latina cancer survivors. Their stories highlight how past life experiences, race, and discordant care contributed to navigating their cancer-supportive care journey alone. Prior to meeting the navigator, they were able to push through with internal strength, yet they experienced significant distress along the way. Community navigators were able to overcome these barriers, address multiple dimensions of unmet supportive care needs, and alleviate patient and family distress. As previously noted, establishment of trust in navigation is essential to acceptance of care and can arise through cultural sensitivity, patient-centricity, and holistic care.19 In fact, recent findings from the Patient Navigation Research Program support that navigation efforts should focus primarily on targeting vulnerable populations, often best served by navigators who are familiar with patients’ community and culture.6
All participants in this study discussed being self-reliant to overcome their experiences of being alone. Previous findings have shown that Black and Latina women rely on altruism, selflessness, and positive thinking to cope with their cancer treatment.20 There may be a double-edged sword to being a strong, independent woman of color: these women are resilient and value health privacy, yet they often suffer quietly and alone. Active inquiry into these values of selflessness and privacy are important so that providers, including navigators, can harness patients’ strength and provide appropriate support.21
Given that communication and cultural barriers contributed to the loneliness of these patients, cancer care delivery should be individualized and responsive to patients’ background and culture. Many women in this study described that support was nominally offered, but not in a patient-centric way. Despite being alone with unmet supportive care wishes, the mismatch between what was offered and what was needed proved so distressful that patients described it as more invasive than surgery. Similar to previous findings,22,23 when care is responsive to patients’ identities, values, and experiences,22 patients report feeling safe and supported, thereby enhancing access to health information23 and promoting equitable care delivery.
It is well known that provision of instrumental support including transportation and financial assistance is an essential component of navigational care.9 These instrumental matters need to be addressed prior to being able to focus on cancer treatment.6 Although less commonly discussed in the literature, our findings suggest that the presence of navigators during clinic visits was also a core element of instrumental support and enhanced feelings of support, empowerment, and respect. One qualitative evaluation examining the impact of Avon Foundation Patient Navigation found that the availability of navigators to attend appointments was noted as a primary strength of their program.24 Attendance at clinic visits on cancer care is important as it has implications on the design of future navigation programs and roles expected for the navigator.
Participants emphasized how multiple dimensions of navigational support enabled them to overcome practical and personal barriers to cancer care, provided stress relief, and mitigated feelings of aloneness. Akin to our findings, previous qualitative studies describe the value of providing social, emotional, and informational support within navigational care.25-27 For example, a recent review of 3 qualitative studies evaluating the impact of patient navigation for patients with cancer found that knowledge empowerment and mitigation of emotional isolation promoted continuity and quality of cancer care.25 Together these findings suggest navigators are essential, primary points of contact for the patient and family. Importantly, through supporting financial, emotional, social, and coordination of care support along the cancer continuum, they overcome internal and external barriers and optimize supportive care experiences for historically underserved patients with cancer.
Implications for Future Research and Practice
Community navigators may be an important component of cancer care models to address the unique supportive care needs of minoritized patients with cancer, yet this component is not commonly evaluated in navigational research.12 Future research should focus on the role of both community- and hospital-based navigation to address the supportive care needs of low-income Black and Latina women. As noted in this study, the community navigators had flexibility of time and space to straddle medical and social needs, which carries both benefits and challenges. Specifically, this connection may be beneficial to patient outcomes, yet it may lead to issues with clarifying boundaries and burnout.26 Future studies should consider how to best integrate community navigators into the multidisciplinary care team to provide support and facilitate maintenance of these personal/professional boundaries.
Limitations
This study carries several limitations. First, the findings are limited by the small sample of women from a single, urban, community-based organization. Although the participants were low-income and of diverse racial and ethnic backgrounds, the majority had a college education, which may provide advantages regarding health literacy and care. This small number and single site may threaten saturation and limits generalizability to women from other geographic areas and/or cultural and educational backgrounds. Future studies should include participants from more diverse cultural, sociodemographic, and educational backgrounds. However, the purpose of this study was to provide a foundation for the development of a community-engaged intervention development that will overcome some of these limitations and provide a wider perspective.
Conclusions
Low-income Black and Latina women with cancer carried internal strength, yet they endured the cancer care process alone, which in turn impacted their cancer care needs and led to significant distress. Black and Latina cancer survivors indicated that upon establishing trust and safety, community navigators addressed their unmet social, emotional, informational, and instrumental needs. In turn, patients felt supported, empowered, and less distressed. Future studies should evaluate the impact of community-based navigation on long-term outcomes across the cancer continuum and investigate how to implement and sustain navigational programs for at-risk patients across medical institutions.
Acknowledgments and Disclosures
Acknowledgment: The authors remain grateful for the generosity of time and experiences shared by all participants.
Conflicts of Interest: The authors have no conflicts of interest to disclose.
Funding: This work was supported by the National Institutes of Health [NCI T32CA225617-03]. Dr Mazor is currently funded by the National Institutes of Health [NCI 1K08CA267309-01].
References
- John DA, Kawachi I, Lathan CS, Ayanian JZ. Disparities in perceived unmet need for supportive services among patients with lung cancer in the Cancer Care Outcomes Research and Surveillance Consortium. Cancer. 2014;120:3178-3191.
- Mazor MB, Li L, Morillo J, et al. Disparities in supportive care needs over time between racial and ethnic minority and non-minority patients with advanced lung cancer. J Pain Symptom Manage. 2022;63:563-571.
- Mariotto AB, Etzioni R, Hurlbert M, et al. Estimation of the number of women living with metastatic breast cancer in the United States. Cancer Epidemiol Biomarkers Prev. 2017;26:809-815.
- Ferrell BR, Temel JS, Temin S, et al. Integration of palliative care into standard oncology care: American Society of Clinical Oncology Clinical Practice Guideline update. J Clin Oncol. 2017;35:96-112.
- Patel MI, Lopez AM, Blackstock W, et al. Cancer disparities and health equity: a policy statement from the American Society of Clinical Oncology. J Clin Oncol. 2020;38:3439-3448.
- Alcaraz KI, Wiedt TL, Daniels EC, et al. Understanding and addressing social determinants to advance cancer health equity in the United States: a blueprint for practice, research, and policy. CA Cancer J Clin. 2020;70:31-46.
- Guan A, Lichtensztajn D, Oh D, et al. Breast cancer in San Francisco: disentangling disparities at the neighborhood level. Cancer Epidemiol Biomarkers Prev. 2019;28:1968-1976.
- Ganz PA, Stanton AL. Living with metastatic breast cancer. Adv Exp Med Biol. 2015;862:243-254.
- Freeman HP, Rodriguez RL. History and principles of patient navigation. Cancer. 2011;117(suppl 15):3539-3542.
- Fischer SM, Kline DM, Min SJ, et al. Effect of Apoyo con Cariño (Support With Caring) trial of a patient navigator intervention to improve palliative care outcomes for Latino adults with advanced cancer: a randomized clinical trial. JAMA Oncol. 2018;4:1736-1741.
- Fink RM, Kline DM, Siler S, Fischer SM. Apoyo con Cariño: a qualitative analysis of a palliative care-focused lay patient navigation intervention for Hispanics with advanced cancer. J Hosp Palliat Nurs. 2020;22:335-346.
- Bernardo BM, Zhang X, Beverly Hery CM, et al. The efficacy and cost-effectiveness of patient navigation programs across the cancer continuum: a systematic review. Cancer. 2019;125:2747-2761.
- Freund KM, Battaglia TA, Calhoun E, et al. Impact of patient navigation on timely cancer care: the Patient Navigation Research Program. J Natl Cancer Inst. 2014;106:dju115.
- Kim H, Sefcik JS, Bradway C. Characteristics of qualitative descriptive studies: a systematic review. Res Nurs Health. 2017;40:23-42.
- Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19:349-357.
- Whittemore R, Chase SK, Mandle CL. Validity in qualitative research. Qual Health Res. 2001;11:522-537.
- Bengtsson M. How to plan and perform a qualitative study using content analysis. NursingPlus Open. 2016;2:8-14.
- Holloway I, Wheeler S. Qualitative Research in Nursing and Healthcare. 3rd ed. Wiley-Blackwell; 2010.
- Gotlib Conn L, Hammond Mobilio M, Rotstein OD, Blacker S. Cancer patient experience with navigation service in an urban hospital setting: a qualitative study. Eur J Cancer Care (Engl). 2016;25:132-140.
- Glaser J, Coulter YZ, Thompson-Lastad A, et al. Experiences of advanced breast cancer among Latina immigrants: a qualitative pilot study. J Immigr Minor Health. 2020;22:1287-1294.
- Gazaway S, Stewart M, Schumacher A. Integrating palliative care into the chronic illness continuum: a conceptual model for minority populations. J Racial Ethn Health Disparities. 2019;6:1078-1086.
- Kamen CS, Alpert A, Margolies L, et al. “Treat us with dignity”: a qualitative study of the experiences and recommendations of lesbian, gay, bisexual, transgender, and queer (LGBTQ) patients with cancer. Support Care Cancer. 2019;27:2525-2532.
- Rust C, Davis C. Health literacy and medication adherence in underserved African-American breast cancer survivors: a qualitative study. Soc Work Health Care. 2011;50:739-761.
- Schlueter DF, Thompson WW, Mason TA, et al. A qualitative evaluation of the Avon Foundation Community Education and Outreach Initiative Patient Navigation Program. J Cancer Educ. 2010;25:571-576.
- Tan CHH, Wilson S, McConigley R. Experiences of cancer patients in a patient navigation program: a qualitative systematic review. JBI Database System Rev Implement Rep. 2015;13:136-168.
- Ferrante JM, Wu J, Dicicco-Bloom B. Strategies used and challenges faced by a breast cancer patient navigator in an urban underserved community. J Natl Med Assoc. 2011;103:729-734.
- Phillips S, Nonzee N, Tom L, et al. Patient navigators’ reflections on the navigator-patient relationship. J Cancer Educ. 2014;29:337-344.



