Background: Since 2015, the Academy of Oncology Nurse & Patient Navigators (AONN+) has encouraged local navigator network (LNN) formation in communities. A network is a group of navigators composed of anyone working in or supportive of the navigation role who chooses to meet in their local region to share strategies, experiences, and resources to increase empowerment and a sense of community. The LNN leader is required to be a member of AONN+ and hold 4 meetings throughout the year. In 2019, the American Cancer Society (ACS) received a Merck Foundation grant to develop a paper outlining effective strategies for the development, implementation, and sustainability of LNNs. The navigation leaders from ACS reached out to AONN+ leadership to collaborate on the development of the paper.
Purpose: To understand the experiences of existing AONN+ LNNs, including their beginnings, challenges, and contributing factors to their success to assist ACS with their grant deliverable and support the growth and development of AONN+ LNNs.
Methods: A 45-item multiple-choice and open-ended survey was developed by the national AONN+ LNN liaisons and ACS leaders to capture LNN composition and meeting structure, as well as successes and best practices in implementing, developing, and sustaining networking. In 2019, a 20-minute blinded survey was e-mailed to the leaders of LNN networks that had been operational for at least 1 year, and each leader was given the opportunity to respond separately over a 2-week period. Eleven LNNs have coleaders, therefore, 34 surveys were e-mailed to LNN leaders representing 23 LNNs.
Results: Twenty-three surveys were completed representing 17 LNNs for a 68% leader response rate. Leaders in the surveys noted that AONN+ mentorship, program champions such as directors or navigators, as well as organized leadership skills were critical to successful implementation. For sustainability, membership “buy-in, pharmaceutical meeting support, and media communication were vital.”
Discussion: In addition to these key factors, leaders supported the development of a toolkit to supplement the current AONN+ LNN online resources to improve mentoring, network leader training, and networking opportunities among leaders to help facilitate mentoring, and sharing of best practices and lessons learned.
Conclusion: AONN+ LNN leader survey responses provided a rich understanding of network implementation and sustainability lessons learned that can be shared with other leaders to facilitate success in local settings.
The Academy of Oncology Nurse & Patient Navigators (AONN+) is the largest national specialty organization dedicated to improving patient care and quality of life by defining, enhancing, and promoting the role of oncology nurse and patient navigators. The organization was founded in May 2009 to provide a network for all professionals involved or interested in patient navigation and survivorship care services to better manage the complexities of the cancer care treatment continuum for their patients. In 2013, AONN+ added the “+” to its name to clarify that the organization is supportive to all those who are involved in patient navigation and survivorship, including nurses, social workers, nonclinical navigators, case managers, administrators, physicians, researchers, and others. The mission of AONN+ is to advance the role of patient navigation in cancer care across the care continuum by providing a network for collaboration, leadership, and development of best practices for the improvement of patient access to care, evidence-based cancer treatment, and quality of life. The vision of AONN+ is to achieve, through effective navigation, patient-centered superior quality cancer care coordination from prediagnosis through survivorship/end of life.
Since 2015, to support the mission of collaboration, AONN+ has encouraged local navigator network (LNN) formation in communities at the local, regional, or state level to facilitate communication and education among peers and improve patient outcomes and survivorship. By the summer of 2019, 23 LNNs had been in existence for at least 1 year, and 4 more were getting established.
Since 2017, the American Cancer Society (ACS) has participated in the AONN+ National Alliance Program to bring together 2 organizations that are strongly aligned in their missions and values to help elevate oncology navigation and improve the care of patients. The agreement is structured to provide interactive opportunities to experience knowledge sharing, increase innovation, and enhance collaborative engagement to pursue superior quality cancer care.
This collaboration allowed AONN+ to assist ACS in a Merck grant proposal deliverable to develop a paper outlining effective strategies for the development, implementation, and sustainability of LNNs. AONN+ had well-established LNNs (ie, had been operational for longer than 1 year and conducted at least 4 meetings every year), which could be leveraged to help ACS with their deliverable and in the process support the growth and sustainability of AONN+ LNNs. As part of the AONN+ and ACS national alliance partnership to advance the field and profession of patient navigation, representatives from both organizations created a project team to collaborate on a survey to collect lessons learned from existing AONN+ LNNs on their development, implementation, and sustainability with the goal to share the findings, enrich established LNNs, and give guidance to future networks as they originate on the local level.
The purpose of this paper is to understand the experiences of existing AONN+ LNNs, including their beginnings, challenges, and contributing factors to their success to assist ACS with their grant deliverable and support the growth and development of AONN+ LNNs. Quantitative findings identify lessons that may be of assistance to other communities interested in creating, maintaining, and evaluating their own LNN, and qualitative results give further insight on the successes, challenges, and best practices with local navigator networking.
Methods
As the ACS and AONN+ team created the tool to describe and explore LNNs, a mixed method survey developed by gathering quantitative items on LNN geographic level, membership composition and meeting characteristics while using a qualitative strategy with open-ended questions, was chosen to capture challenges, successes, ideas, and best practices on LNN implementation, development, and sustainability.1,2 To focus the survey, it was developed with a specific approach to broadly describe the LNN landscape with quantitative questions and then narrow the focus to frame the development of LNNs.2 Also, a “please describe” option was used for clarification of the qualitative selections to provide a more detailed insight into LNN practices. A review of the literature through PubMed on any articles that addressed community professional local network development, implementation, and/or sustainability was performed. However, there was a dearth of articles, and most were limited to community and government structure.
The project team elected to include all established LNNs within the survey population. AONN+ recognizes 27 LNNs; however, 4 LNNs had not been in operation or established for a full year and were not eligible to take part. This decision reduced the coverage and sampling errors that are common with surveys when only a part of the intended population is invited to participate.1,3 An electronic format via e-mail was used because each LNN leader in previous correspondence demonstrated access to a computer. Prior to release to the participants, the survey was loaded into SurveyMonkey, and the development team previewed for content coverage. After edits, a 20-minute survey comprised of 45 short items was disseminated to each LNN leader with a letter describing the contents of the survey questionnaire, time length, and how the summarized recommendations will be published. No incentive was provided to leaders for participation. The survey return was set for 2 weeks, and to decrease the nonresponse error, a reminder to complete the survey was sent out 1 week prior to the deadline to all participants. Because 11 LNNs have coleaders, 34 surveys were e-mailed to LNN leaders, which represented 23 LNNs. By having coleaders respond independently of each other, it allowed a wider leader perspective. Frequency data were generated for each item.
Findings/Results
Twenty-three surveys were completed representing 17 LNNs for a 68% LNN leader response rate. At the time of the query, there were 26 established LNNs in the United States and 1 international group. Two were inactive since they had not responded to queries with any meeting reports within a year, and 1 was reorganizing after being inactive. These 4 LNN leaders (2 leaders in 1 LNN) were asked to participate but did not respond. There was a 74% (17 of 23) response rate from the LLNs that had been meeting consistently over the past year.
The professional roles of the responding leaders were nurse/clinical navigator (72%), patient navigator (20%), program administrator (4%), and public health professional (4%). Most of the leadership structure (78%) is composed of a leader or coleaders (61%), with 48% having a scribe or secretary, 26% having a membership chair, and 13% having a program chair.
Composition
The composition of the LNNs replying to the survey reflected 14 states spanning the United States and 1 international group, with the demographics reflecting urban, suburban, and rural areas. The majority were on a regional level (43%), followed by a state venue such as the entire state or upper/lower/southern/northern area (35%), health system (13%), and 1 LNN was a health system organization. Two of the groups are connected to their respective state cancer plan or organizations. Overall, 95% of the LNNs reflect their state name.
Membership base queries showed that 70% of LNNs had more than 20 individual members, 26% with 10 to 20, and only 1 LNN had fewer than 10 participants. The LNN leaders are encouraged to reach out and include other navigator organizations or community agencies outside of their healthcare system, and the survey responses revealed that 13 LNNs had under 10 represented, 8 had between 10 and 20, and only 2 had more than 20. Eighty-six percent of the groups never experience challenges in sharing ideas or resources among competing health systems. The member roles were diverse, with the majority being clinical or patient navigators. The Figure shows the composition of varied participants in LNNs. Fifty-five percent of the LNNs do membership outreach or marketing to invite other relevant professionals to their meetings. The leaders estimated that 37% of their membership were AONN+ members. Ninety percent of the LNNs did not participate in the AONN+ 2019 membership challenge campaign to increase national membership.
All LNNs reported meeting the minimum of 4 times a year. Four of the LNNs went beyond that expectation, with 3 meetings monthly, and the others meeting 9 times a year. All the networks meet in person, with 30% adding audio technology and only 10% using video/webinars media (prior to Coronavirus disease 2019). The local groups have a variety of meeting formats throughout the year, with networking activities (78%) being the most common meeting format, followed by data presentations by a pharma-sponsored speaker/dinner (70%), continuing education sessions (65%), case studies (57%), and patient education seminars (22%).
Program Development
Sixty percent of the networks do not survey their membership to identify best practices or gaps in care to plan programs, but 83% host invited speakers to help members increase their knowledge in these areas. Most LNNs do not promote cancer awareness months (74%) or invite patients to participate in educational activities (70%). Fifty-five percent have received funding from product companies, industry, or pharmaceutical companies to support program activities.
In response to networking of membership, 83% of the LNNs encourage communication and interaction of members outside of the regular meetings, and 87% feel that the needs of the membership are being met by LNN activities of connecting with other navigators, sharing experiences, and promoting best practices. No members participate in more than 1 LNN.
On questions around LNN membership attending AONN+ conferences, 70% attend, and 85% would be interested in LNN activities at midyear or annual national meetings.
Implementation
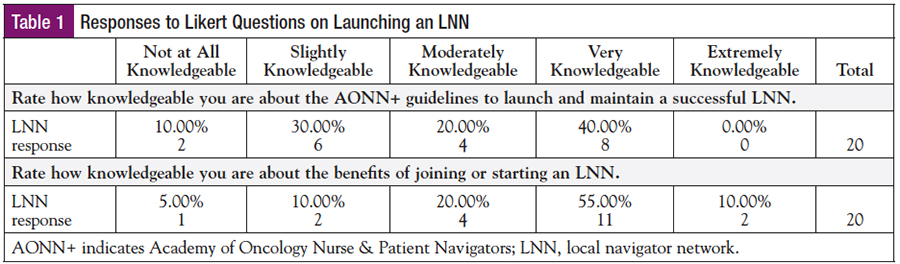
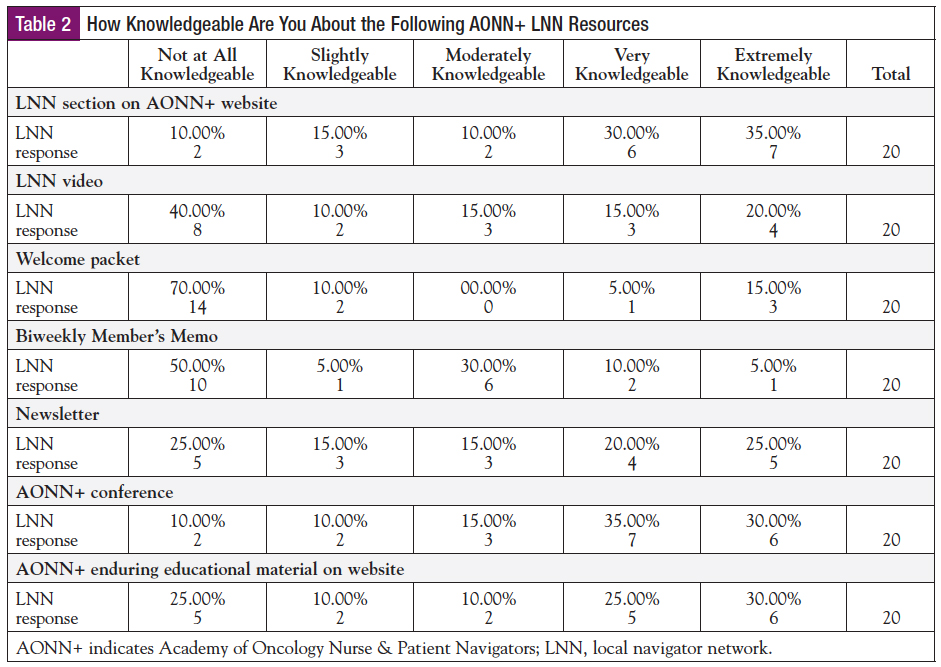
Using a 100-point Likert scale from not at all (0) to extremely knowledgeable (100), the leaders ranked aspects of starting an LNN. When the leaders were asked about the AONN+ guidelines to launch and maintain a successful LNN, 40% were very knowledgeable, 40% had limited knowledge, and 20% fell in the midrange. On the same scale, 65% were well versed in the benefits of joining or starting an LNN, 15% were not informed, and 20% fell in the midrange (Table 1). When asked about the AONN+ LNN resources, the conference networking events (80%), the LNN website (75%), educational videos (65%), and the quarterly newsletter (60%) were the resources they were knowledgeable about. Most leaders were not aware of the welcome packet (79%) and Member’s Memo (55%) (Table 2). When asked about use of the AONN+ LNN resources, again the conference networking events, newsletter, and LNN website were recognized as reflective of knowledge about resources; the welcome packet and Member’s Memo were rarely tapped.
Findings—Open-Ended Questions
The survey asked open-ended questions on LNN implementation, sustainability, and ideas to support networking and growth. Eighty-seven percent of the respondents qualitatively described successes, challenges, and resources they found helpful, as well as support they would have liked for implementation, sustainability, and development of an LNN.
The first question on implementation asked leaders to describe their biggest successes or practices in implementation. The number 1 answer was networking among peers in the same institution as well as those outside their practice, and being able to share resources and discovering new ones in the area. “We all wear similar ‘hats’ but found out quickly how much our roles varied from practice to practice working in a community setting.” The additional bonus of collaboration was better care coordination among service lines and cancer centers. The networking included peer-to-peer advice and sharing of best practices. The second key to successful implementation was having multidisciplinary and coworker members attend. To promote attendance, the meetings were held at different locales to accommodate those in other areas of the region, e-mail or Facebook announcements were posted, and technology meeting formats such as Zoom were used for face-to-face or phone connections. Another strategy was proactively planning education via dinner meetings or summits with experts in different fields. Some LNNs used a continuous action item around training and certification or resource sharing at each gathering to encourage interest in professional growth, and others were able to provide continuing education units for obtaining certification or renewal.
The biggest challenges identified in implementing an LNN were around membership and programs. The main membership concerns were actual attendance at networking events, with distance as a barrier, and secondly, getting people to commit to assist in planning meetings. Distance was mentioned by several leaders, and even getting people to attend by technology encountered resistance. Sadly, lack of health system support was mentioned. “Navigators are largely unsupported by their parent organization so that you have to expect very low attendance in relation to the numbers ‘on paper’ in the e-mail invite.” A few mentioned the challenge to get others to join who do not have “navigator” in their title. A different view on the “navigator” title came from a group that had to be firm about who could attend—“not for people looking for a night out/dinner to socialize.” AONN+ was recognized as a resource to help walk the leader through the network start-up, and comments reflected the support for the initial LNN meeting invite, starting a membership roster, and the website.
No-shows were also experienced despite the positive return of people committed to attend. One LNN is exploring the idea of charging a small fee to attend meetings because “some folks would say they are coming and would not show up, so we would end up with more food than we needed.” Also, getting members to help with scheduling meetings, identifying discussion topics, finding sponsors, and lack of interest to serve on a position/board in the LNN were struggles for some groups in the implementation phase.
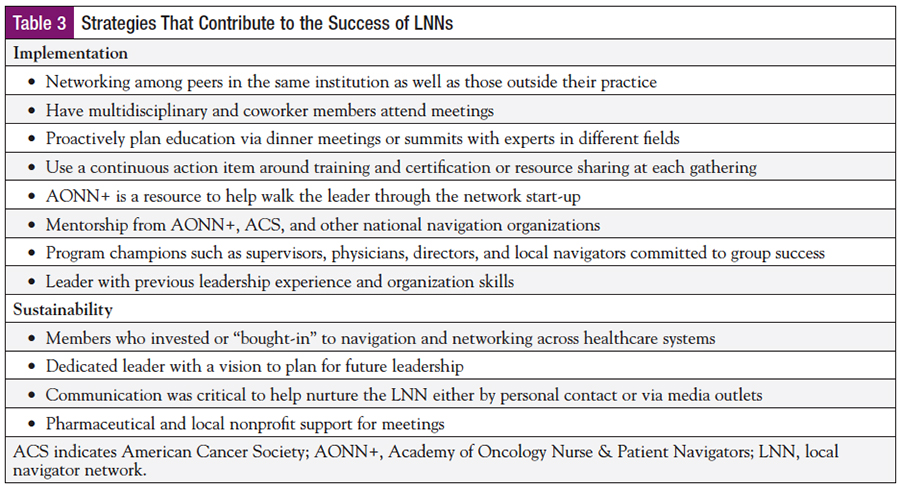
Leaders were asked to identify resources or support that upheld the implementation of the LNN. Three common themes were identified. First was mentorship from AONN+ with specific mention of leadership response and guidance, website resources, and other LNN leaders who were a positive influence when the new LNN organizer reached out to them for contact and feedback. The ACS was noted as an advocate for meeting resources as well as providing a location for gatherings. Other organizations were George Washington University and Harrold Freeman navigation programs, as well as local patient support agencies and pharmaceutical companies. Of note, pharmaceutical companies have commented to AONN+ leadership that LNNs were an attraction for them due to well-attended gatherings. Second were program champions such as supervisors, physicians, directors, and local navigators as they committed to the success of the group. Also, the past leadership gave guidance as they were included on communication and decision-making after they transitioned out of their role, and current leadership was proactive in guidance with regularly scheduled meetings to discuss how to best guide the LNN. The final theme was the leadership skill of the organizer. Previous leadership experience from other organizations or roles was noted to help take the LNN forward (Table 3).
This question was followed by asking them what support or resources in hindsight would have been helpful in implementing their group. The primary need was “more direction on how to lead this group.” The cited leadership needs revolved around the concepts of leadership skills, group dynamics such as a focused purpose, how to transition group knowledge to benefit navigators as well as patients, how to tap into other LNNs, accessing pharmaceutical industry or organizations for resources and ideas, and how to unify opposing members from different organizations. The other need was a “how to” or a basic toolkit on developing an LNN. They asked for this kit to include best practices and lessons learned from other LNNs, governance advice, and financial costs of meetings. One participant wanted “AONN+ resources which were shared in 2019…I plan to use them for talking points.”
Sustainability
LNN leaders were asked open-ended questions about sustainability and what has been most helpful to guide and keep the LNN functioning. The most frequent reply was the members who were invested or “bought-in” to navigation and networking across healthcare systems. “The navigators themselves getting to know each other and work together.” “Navigation as a team being supportive and attending meetings.” Dedicated leaders with support from champions such as physicians, managers, directors, and AONN+ guidance, as well as supportive navigator members, were recognized as a vital core group to support consistent meetings and current topic discussions, and the words “determination,” “doing the lion’s share of the work,” and “passion” were used to describe this effective group. One leader recognized planned transition among leadership in alternating years, so it was not a brand-new board every 2 years. Pharmaceutical and local nonprofits support were other common responses because they provided education, a nice relaxing atmosphere after work, and speakers on navigation-related topics. Also, communication was critical to help nurture the LNN either by word of mouth, per AONN+ website, leaders, or newsletters, annual meeting attendance, and Facebook. Five LNNs created a web page for their members after this option became available through AONN+ in 2018. “This encouraged the identification and connection of like-minded initiatives in providing guidance.”
In response to what would be helpful to support sustainability of the LNN, leaders desired specific training with needs for running a successful meeting (“how to get navigators to participate”), basic funding education that includes scholarship development to promote national meetings attendance, and how to get continuing education for members. Many want to network with other LNNs to learn from their challenges and successes:
- “Fund a training conference or a webinar to bring networks together”
- “Have a way to network to learn how others are working their LNN”
- “Guidance on getting navigators to participate”
- “Additional resources on how to run an LNN meeting, how to talk with sponsors, ways to have a successful LNN”
The leaders then described what was challenging to the sustainability. Common responses included:
- People issues were a challenge as members changed roles and dropped out of attending
- Struggled with work/life balance
- Did not attend after a positive RSVP
- Felt like the distance was a hardship with region versus a city meeting
- Lack of other leaders stepping up
- Lack of funding
One positive response to this difficulty was “growth over the last year due to a more engaged member chair.” Over half of the LNNs do get funding for program support or summits, and AONN+ does not have a financial relationship with LNNs.
Additional Suggestions of LNN Support
Ideas or suggestions to support the networking and initiatives of LNNs were collected from the leaders, and a common reply was to bring leaders or LNN representatives together on a regular basis, and proposed online avenues were a webinar, chatroom, Facebook page, or forum board. They would like this site to have the ability to ask questions, receive answers, and highlight LNNs. They asked for the LNN website and newsletter to continue because it is accessible to all LNNs no matter their geographic location, and for AONN+ to “continue education and support from their leadership.” Two leaders asked for AONN+ to contact “local media outlets where navigators meet to highlight our work and network initiatives since we do not have public relations support.” Then the question was phrased around the concept of supporting LNN growth, and the same ideas on leadership training, funding support, scholarships, and an avenue for leader networking were reiterated.
In the survey closing, the leaders were asked to share anything else about their LNNs. Two LNNs are 5 years young, and the leaders were “extremely proud” and “excited to provide a forum for navigators.” The determination to continue to grow membership, and appreciation for engaged attendees was voiced repeatedly. The vision for scholarship support to attend an AONN+ conference was noted, and until that goal is achieved, they would like to “schedule some form of webinar to have members Zoom into parts of the conference.”
Discussion
With a 74% response rate from LNNs that had been actively meeting for more than 1 year, and because the composition of LNN respondents was inclusive of multiple geographic areas across the United States, the information captured from this sample is reflective of the breadth and appropriately represents this population to draw conclusions on network implementation, development, and sustainability in the United States.4
The leadership structure varies per LNN, but the majority have a leader and coleader who facilitate the meetings and work on the action item tasks such as contacts, resources, etc. Half of the networks have a secretary or scribe, and this is invaluable since AONN+ asks for a meeting summary via standard form after each networking session and an annual report each year. Others that are more developed in structure with a larger membership base have a membership chair who can develop a member roster and help people join future meetings. A program, education, or social media chair is seen in larger membership networks. The leader and/or coleader information is displayed on the AONN+ website with contact information so AONN+ members in the area can reach out to the network, and it is optional to add other member positions. Five of the responding LNNs have supportive positions posted on their LNN website. A basic premise for implementation is a leader; the other supportive positions can be developed as the group expands membership.
Interestingly, one-fourth of the LNNs are led by navigators other than nurses, and this reflects the inclusiveness and mission of AONN+ to advance the role of all those involved in patient navigators across the care continuum by providing a network for collaboration, leadership, and development of best practices. Since AONN+ is the only professional organization to support all types of navigators, the leader can be a nurse navigator, patient (nonclinically licensed) navigator, or someone involved in supporting navigation (administrator).
Answers to the membership base queries on size and geography support the AONN+ position not to set a minimum number for membership in less populated areas. Creating a support network of other like-minded people in the rural or less populated settings can encourage sharing of common issues and strategies as well as promote empowerment to face challenges. AONN+ encourages the group to have their own local identity, and this was evident in the survey as networks with names such as Journey Across Maine, Fairfield County, Greater Kansas City, and North or South Florida responded. Two of the groups are connected to their respective state cancer plan, therefore they identify with the entire state.
LNN membership makeup shows diverse networks, with all having representation from different cancer centers or healthcare organizations and a variety of navigation types or supporting roles. The majority of LNNs never experience challenges with sharing ideas or resources among competing systems, and only 2 leaders commented on the rivalry between healthcare organizations and getting others to see “that we are not competitors but collaborators.” “We all agree that we only want the best outcomes for our patients.” “We connect directly with each other and meet at a neutral site to preclude any idea of one system being emphasized over another.” “The leadership team highlighted representatives from all systems equally. They openly discussed programs, challenges, and resources among competing systems to promote best practices and gaps in care.” “We share information related to both member and patient educational opportunities and/or resources with our members.” One participant described it as “members are aware of their organizational rules,” and this could reflect the unspoken rules that are behavioral constraints imposed in organizations or societies that are not voiced or written down. AONN+ encourages the leadership to reach out to navigators (patients, nurses, social workers, etc) outside their healthcare system and offer to assist with a list of members in the area as the LNN is being implemented. Since organizational networking is reflected positively in most leaders, this practice will continue to be encouraged at the initiation stage, with the expectation that each member will act according to any organizational constraints. The ripple effect of inviting will also remain to help drive membership. “We communicate with other program navigators via e-mail and by sharing informational flyers for upcoming meetings.”
Even though AONN+ asks the LNNs to strive for a membership roster of at least 50% current AONN+ members, this is not a focus of the LNNs, as shown in the survey results and lack of participation in the 2019 membership campaign. The primary emphasis on developing a local network of navigators is to facilitate communication and education among peers and to improve patient outcomes and survivorship. As local attendees are exposed to AONN+ through the networking and continued interest in meeting, the goal is that they will join on the national level at some future point.
Each LNN’s individuality is reflected in their varied meeting frequency and formats. By all responding that they were able to meet 4 times a year, AONN+ will continue to keep this minimum expectation and encourage additional programs if feasible for the group. All networks meet in person for that face-to-face networking, but for future implementation and development support, a review of meeting audio and video options would enrich other attendance avenues. The virtual media routes might increase attendance for those with distance concerns and home commitments and be critical during a national crisis like COVID-19. For financial feasibility, the international group uses WhatsApp to connect to their diverse navigators since this is a free app for phones or computers that allows one to send messages, pictures, videos, and even voice recordings over the Internet, rather than using a mobile network that charges a fee.
It was not surprising to see networking and data presentations with pharma dinner support as the most used formats since this is a time to facilitate communication among community members, promote education, and all networks meet apart from their work commitment. The welcome packet has the various formats (case studies, networking, education seminars, data presentations, continuing education [CE]) explained to stimulate meeting ideas. LNN leaders requested more information on obtaining CEs for their meetings. The popular route is through medical or pharmaceutical companies. Another avenue is to show an AONN+ CE webinar, after which each member can go on the website and complete the CE application. Non-AONN+ members do not have access to the CE credit. Since two-thirds of the LNNs offer CEs, and because this is a need for maintaining national certifications, additional information can be developed on how LNNs get CEs based on the current knowledge of the successful leaders in this area.
For program development, the majority of LNNs do not survey their membership for program ideas on best practices or gaps in care, but the minority that did shared navigator programs gleaned from their membership. Financial toxicity including insurance delays, role delineation, rural navigation, certification, training, metrics such as time to CT/PET scheduling, tumor board, transportation issues, multidisciplinary care, increasing demand for genetics, as well as national shortage of counselors and pathology concerns, are programs they have addressed or plan to share in future meetings. Financial toxicity was a best practice concern in 2018, when Virginia partnered with pharmacology and oncology financial assistance organizations and provided speakers focused on overcoming financial barriers as part of their quarterly meetings. Pharmacology financial patient advocates and nonprofit organizations provided booths with information and contact information for attendees.
Of the LNNs that do not survey their membership for program ideas on best practices or gaps in care, many host invited speakers or summits to address the knowledge and care gaps around the topics of patient advocacy, professionalism, research, integrative services, sexuality, genetics, survivorship, individual cancers, and financial navigation. Two groups held a summit and used vendor support to increase the knowledge of treatments patients may receive across the continuum. The other groups used local specialists, such as physicians or nurse educators, AONN+ Leadership Council members, patient advocacy foundations, unbranded pharma education with sponsored speakers, and local members. Discussions at meetings, especially around an educational topic, allow sharing about inequalities in treatment. The member survey is an initial suggestion from AONN+ to plan future meetings, but because there are overlaps in topics in either approach to programming, each of these methods can be addressed as options for LNNs to employ in program development.
Programming around cancer awareness months or the use of patients in educational events is not a common practice with LNNs. For the few groups that do promote cancer awareness months, the meeting has a specialist speak on the topic or highlight LNN members with that unique navigation talent in a way to increase disease knowledge and unique challenges that come with the disease. For example, gynecologic cancers featured in September has a program around challenges of screening, HPV vaccinations, genetic testing, lymphedema, and newer treatments such as PARP inhibitors or immunotherapy. For the few LNNs that use patient involvement in professional meetings, this must be done thoughtfully with guidance so the patient can contribute their personal experience with respect to dealing, working, and collaborating with professionals in the field as they express issues that matter to them. It can be a win-win situation with navigators gaining from the personal patient experience perspective, and patients can gain more knowledge on navigation that can increase navigation awareness and benefit the profession.
The leaders were asked if they had received funding to get started, or if they had obtained outside funding to support program activities. This funding came as money for a summit or a full-day meeting, and most did not receive direct funding per se but commented on medical companies or pharmaceutical support with dinners and educational speakers.
The primary purpose of LNNs to support the mission of collaboration is being met, as the leaders responded positively to the query about the needs of the membership being fulfilled by the connectivity with other navigators and sharing of experiences and best practices. Over three-quarters of the LNNs encourage networking outside of regular meetings, and this is promoted through e-mail, Facebook, contact lists of members, and sharing of business cards. The leaders described navigators meeting for “happy hour,” dinner at local restaurants, and “time out” among professionals. “Networking in our LNN has helped to facilitate introductions and new relationships between members from different organizations around the area.” This leads to improved patient outcomes as “we often help coordinate care for patients that may need to go to that area or hospital.” One leader summed it up as “our LNN is a forum for knowledge exchange as well as ongoing networking and support for members.” For 1 leader who did not see the networking advantage, they cited the coverage of an entire state as a disadvantage…“being spread so thin that travel after work is a challenge.” No LNN had members who participated in more than 1 LNN, and this is understandable with the distance between present LNNs.
On a national level for collaboration, more than two-thirds of the LNNs have members who attend the AONN+ annual or midyear conferences, and the majority were interested in an LNN activity at the AONN+ conferences. AONN+ will continue to request that 1 or 2 members attend the annual conference because this is an opportunity to network with other LNNs and come together to openly share triumphs and challenges. At the meetings, there have been LNN sessions on State of the Art of LNNs, meet and greet AONN+ leaders, and the option to have meeting space for their LNNs. Each year an LNN is selected as the Outstanding Local Navigator Network Award winner for exceptional work in the establishment of an open forum for professional development and networking that aligns with the AONN+’s national mission. The meeting and support for LNNs on the national level will continue.
Implementation of an LNN
The leader responses to being knowledgeable about LNN resources to launch and maintain were split between the extremes on the continuum, and a minority felt uninformed on benefits of joining or starting an LNN. The welcome packet to new LNN leaders was organized in 2018, so LNNs established prior to that time did not receive written instructions on website posting information, leader responsibilities, meeting ideas, and how to develop the LNN mission, vision, and goals, as well as when to complete meeting forms and annual report at the time of implementation. The information was shared with LNN leaders in 2018, but as leadership positions changed, it is possible the information was not passed on to the next leader. In the future, AONN+ can share this same package with all existing leaders as well as any future new leaders. The package does not include specifics on benefits to join or start an LNN, but this can be developed to enhance the welcome kit.
When the LNN resources were broken down by individual items, most leaders were aware of the conference networking events, the LNN website section, the LNN video, the webinars offering free CEs to participants, and the quarterly newsletter, but they were not as informed about the Member’s Memo in the Navigation & Survivorship News or the LNN welcome packet. The question was rephrased to ask about the use of AONN+ resources, and the responses reflected the same awareness. To promote awareness, as well as encourage use of available resources, AONN+ can send out the welcome packet to ALL current leaders. The Member’s Memo awareness and use was puzzling because it is referred to in each quarterly newsletter that leaders receive, and the newsletter had high recognition and application. The Member’s Memo can be highlighted and bolded in future newsletters to increase its visibility, and leaders can receive additional correspondence via e-mail. Since it is in a biweekly e-mail, leaders may not be accessing it due to their workload, the e-mail could be lost in cyberspace or spam, or because they receive frequent e-mails from the professional organization, they may delete it prior to reading. Since the e-mail is delivered every other Friday and is titled AONN+ Navigation & Survivorship, leaders can be informed to look for the correspondence.
The open-ended questions provided more detail on how to support implementation. To attract and implement LNNs in the more sparsely populated areas, such as Alaska or the southern and midwestern states, it would take a strong leader with organization skills and champions throughout the region. But the question remains how to connect navigators over large areas that do not have Internet access or even personal phones. Key central meeting points that are accessible to these navigators, such as ACS sites, Cancer Community Support Centers, or other sites with Internet connectivity, could be identified and would allow virtual networking. The leader and champions would have to proactively mail meeting announcements with plenty of advance notice for navigators in these areas to plan attendance. Key insights can always be derived from those desiring connectivity who reside in the low-density population areas.
The welcome packet can be enhanced with the requests for best practices, group dynamics such as a focused purpose, how to tap into other LNNs, and pharmaceutical/industry or organizations for resources and ideas on programs and costs of meetings. This project could be a network among some of the more successful LNNs as well as the ones facing challenges in implementation. The goal would be to share the expanded welcome packet with current leaders and any future new leaders.
Virtual meetings can address the costs of in-person meetings, although this is still an issue for rural frontier communities that lack hardware support such as phone, computers, or Internet access. The survey was issued prior to COVID-19, so any hesitancy using webinars for meetings and socials (cocktail hour) may have diminished, making them a viable solution for most members.
The open-ended discussion on sustainability revealed a need for governance advice, obtaining CE credits, and program funding. This request is different from the welcome kit that is shared with the LNN leaders at network inception. The leaders want hands-on management training and networking that can be completed in a webinar or a series of webinars to address each of these ideas in a group format. With the increased use of technology, this is a feasible request that can be presented live and then stored on the AONN+ LNN web page. In 2020, the AONN+ Leadership Council was exploring the concept of scholarship support for members to attend the national meetings, and this will be shared with LNNs once it is developed.
Limitations
Since only 1 respondent was international, the information cannot be generalized to this group. If the 3 inactive nonresponse LNNs had shared their comments, the information on sustainability would have been enhanced with information on challenges LNNs face over time.
Conclusion/Next Steps
The survey provided a rich insight into what is going well for LNNs as well as ideas for improvement (Table 4). Also, it will fill a gap in the existing literature about creating and maintaining an LNN and add to the evidence base of networking value. AONN+ will continue to enhance the welcome toolkit with suggestions from this survey and continue the current resources on the LNN website that leaders found helpful. AONN+ will move forward with the scholarship exploration to support attendance at national conferences. The quarterly newsletter will continue to highlight AONN+ overall activities with the expectation of LLN leaders sharing with their membership. The Member’s Memo will continue as a biweekly column dedicated to LNN activities. Reintroducing assets to current leadership and providing to future leaders will be an ongoing endeavor. In collaboration with the ACS national alliance partnership to advance the field and profession of patient navigation, a basic toolkit on developing an LNN is a vision to replace the welcome kit in the future. This kit will include best practices and lessons learned of other LNNs, governance advice, and financial aspects of meetings. An online LNN leader training will be a focus for AONN+ to develop, with the objectives of how to lead, leadership skills, group dynamics, as well as expectations of leadership to be highlighted. The sundry topics on membership nuances, successful structure to promote participation, funding, program development, CEs, and others raised in this query will be used for future leadership training. An avenue to bring leaders or representatives together on a regular basis or in a “leader only” forum will be explored. AONN+ will continue to be responsive to leadership queries and outreach as well as guide new LNNs as they develop nationally and internationally.
References
- Ponto J. Understanding and evaluating survey research. J Adv Pract Oncol. 2015;6:168-171.
- Agee J. Developing qualitative research questions: a reflective process. International Journal of Qualitative Studies in Education. 2009;22(4):431-447.
- Fincham JE. Response rates and responsiveness for surveys, standards, and the Journal. Am J Pharm Educ. 2008;72:43.
- Evans JR, Mathur A. The value of online surveys: a look back and a look ahead. Internet Research. 2018;28(4):854-887.
Acknowledgment
The author would like to acknowledge the contribution by Nicole L. Erb to this project while she was serving in the role of Director, Cancer Control Initiatives, for the American Cancer Society.