Background: With increasing numbers of cancer survivors in the United States, cancer survivorship is of significant concern for nursing practice.
Objectives: The purpose of this project was to understand the unmet needs of cancer survivors as well as the role of cancer survivorship programs.
Methods: The cancer survivorship program consisted of 4 weekly complementary therapy sessions open to cancer survivors and their caregiver(s) in a rural county in New York. Participants completed questionnaires regarding unmet needs, attitudes, beliefs, and utilization of cancer survivorship care and complementary therapies. Participants completed postsurveys following attendance. Funding for this program was made possible by the Richard C. and Mary Anne Palermo Family Fund.
Results: Eleven participants attended 1 or all sessions. Unmet needs in cancer survivorship included concerns related to stress, lack of availability of complementary therapies, side effects of treatment, and quality-of-life concerns. The program results yielded participant desire for a sustained oncology program with a focus on interactions with other survivors.
Discussion: Unmet needs in cancer survivorship continue to be a challenge in the field of oncology. Cancer survivorship programs focusing on various therapies, including complementary modalities, are useful for addressing these unmet needs.
Conclusion: More research is needed on the role of cancer survivorship programs. This pilot program demonstrated that cancer survivorship programs are valuable and helpful for cancer survivors.
Cancer survivorship is a growing concern for healthcare providers in the United States. In 2006, the Institute of Medicine (IOM) recommended all cancer survivors receive an individualized survivorship care plan (SCP), including documented guidelines for health maintenance and monitoring.1
Survivorship care planning was an initiative introduced by the IOM to mitigate the growing needs of the increasing numbers of cancer survivors living in the United States. The American Cancer Society reported there were 15.5 million cancer survivors in 2016, and the number is projected to increase to 20.3 million by 2040, indicating this is going to be a concern for the healthcare system.1 The American Society of Clinical Oncology recommends cancer survivorship care programs as an intervention to meet the needs of cancer survivors through appropriate monitoring, follow-up care, needs assessments, and identification of risks and barriers.2 Rural locations are at risk for poorer healthcare outcomes associated with cancer survivorship and are of interest due to concerns related to access, socioeconomic status, and behavioral patterns.3
The transition from oncology to primary care is a challenge for cancer survivors. Survivors question whether they are considered to be in active treatment or survivorship. Also, there is a lack of personalization, and unmet needs remain.4,5 Patients expressed that ways of mitigating these unmet needs include support groups, having someone to call during times of need, and having family members involved in cancer survivorship.5 The use of designated staff in cancer survivorship care planning visits was a method of providing survivorship care discussed in the literature.5 Other cancer survivors felt the role of the nurse was essential, and they requested nursing participation in the process and felt oncology nurses with experience were most appropriate to provide cancer survivorship care.6 Cancer survivorship programs are a method of meeting some of these transitions and unmet needs successfully.
A successful cancer survivorship program should incorporate integrative therapies to meet the various and individualized needs of cancer survivors.7 Complementary therapies have been utilized in cancer survivorship with notable success in enhancing patient care experiences.8 Rural counties lack access to many of the integrative therapies that are being offered to their urban counterparts.
Cancer survivorship is a life-altering, dynamic, ongoing, individual experience beginning with a diagnosis of malignancy and containing a duality of positive and negative aspects with universal elements (universality). A theoretical underpinning of a program for cancer survivors requires an understanding of the ambiguity and uncertainty that occurs in cancer survivorship. Mishel’s Theory of Uncertainty in Illness provides a conceptual model to understand cancer survivorship and was used to provide a framework for this pilot project.9 According to Mishel, uncertainty is the inability to assign a specific value to events or accurately predict outcomes, making meanings of illness indeterminate.9 There are 3 parts to this theory, including the antecedents that occur prior to the diagnosis or illness experience, the appraisal that occurs while placing value on the uncertain situation, and coping with the uncertain situation, which is used to deal with uncertain events in the future.9 This theory explains the uncertainty that comes with cancer survivorship, and the fear of recurrence and secondary cancers cancer survivors face.
Objectives
The purpose of this project was to evaluate unmet needs of cancer survivors living in rural areas and their caregiver(s) as well as to measure attitudes, beliefs, awareness, and intent of use following the implementation of a cancer survivorship program. One goal of this pilot project was the successful implementation of a pilot cancer survivorship program focused on complementary therapies as a modality for alleviating unmet needs in cancer survivorship for both cancer survivors and their caregiver(s). This project obtained baseline data of the unmet needs of the cancer survivors and their caregiver(s). A second goal was to increase the awareness of participants of the cancer survivorship plan of care. A secondary component was to provide all primary care providers throughout the county with information about The George Washington University website that hosts free online e-Learning. A letter requesting provider support to encourage cancer survivors in their practices to attend the program was sent to their offices.10
Sample and Setting
Any cancer survivors and their caregiver(s) in the county were invited to attend the program through the marketing for this program. No cancer types were excluded, and anyone at any stage of survivorship was encouraged to attend 1 or all sessions. Each week included the presentation of a different complementary therapy. Topics included music therapy presented by a licensed music therapist, oncology massage (OM) by a licensed massage therapist with OM training, chair yoga taught by a licensed yoga instructor who routinely teaches yoga to cancer survivors, and mindfulness-based stress reduction (MBSR) taught by a registered nurse trained in instructing MBSR to clinicians. Institutional Review Board approval was granted by the writer’s college for this project. A total of 11 participants attended at least 1 of the 4 sessions, which took place in a public library in a rural county in New York State. Informed consent was obtained from all participants.
The CaSUN (Cancer Survivors’ Unmet Needs) measure is a validated psychometric tool created by Hodgkinson and colleagues and is used with permission.11 This tool measures unmet needs of cancer survivors. Preprogram surveys included demographic data and questions that elicited information regarding participant knowledge, attitudes, beliefs, and utilization of complementary therapies, cancer survivorship care, current utilization of complementary therapies, as well as information on SCPs and treatment summaries (TSs). Each 2-hour session began with 15 minutes reserved for filling out preprogram surveys and questions. The principal investigator spent 15 minutes discussing cancer survivorship care, including fear of recurrence, lifestyle behaviors, transitions in care, appropriate provider contacts, SCPs, TSs, and appropriate monitoring and surveillance. The complementary therapy expert spent 15 minutes discussing the use of the complementary therapy in cancer survivorship and then demonstrated the use of the therapy to participants. The rest of the session was reserved for postsurveys and questions.
Results
Results were obtained through preprogram and postprogram data. Demographic data were obtained in preprogram surveys. Participants ranged in age from 50 to 72 years, with only 1 participant identifying as male. No participants identified solely as caregiver, but 2 participants identified as both cancer survivor and caregiver. All participants identified as white; 5 had a high school diploma or GED, 3 had associate’s degrees, 2 had bachelor’s degrees, and 1 had a graduate degree. Five of the participants were employed at the time of the study, 4 were retired, and 2 were disabled. Two of the participants identified as single or never married, 1 identified as divorced, and 8 identified as married or in a domestic partnership. The participants were asked to rate their health at the beginning of the program. One participant rated their health as excellent, 6 rated their health as very good, 3 rated their health as good, and 1 rated their health as fair. Participants were asked about the current state of their cancer survivorship care. When asked how often they receive cancer survivorship care, 2 participants responded “every 12 months,” 6 responded “every 6 months,” 2 responded “every 3 months,” and 1 left this question unanswered. When asked about their satisfaction with care, 4 participants stated they were very satisfied with their care, 5 responded they were satisfied, and 2 responded neutral. Participants were given the definition of SCPs and TSs and asked if they had received them. Four participants responded yes, 5 responded no, and 2 responded unsure. The 4 who responded yes stated they received this information prior to ending cancer treatment. One stated they were very satisfied with the SCP/TS, and 3 stated they were satisfied with the SCP/TS. When asked if they took this information to all provider appointments, 1 responded “always,” 1 responded “sometimes,” 1 responded “never,” and 1 responded “this has not happened yet.” Participants were asked what complementary therapies they were currently utilizing, and what they would like in the future (Table 1).
Postprogram surveys were obtained at the end of every session with questions on participant satisfaction. Participants stated they were satisfied with the content, and the highest satisfaction scores were noted with the content in the MBSR and OM surveys. Participants found the content useful; the speakers helpful; enjoyed the time, date, and location; and were overall happy with the program. The survey also asked what topics the participants would like to see in the future. The responses included emotional support, dealing with the fear of cancer returning, nutrition, journaling, support groups, and alternative treatments at a reasonable price.
For purposes of this project, any CaSUN score over 5 was considered a higher need. The higher needs reflected in this survey included contact with other survivors, quality-of-life changes, coping with the impact of cancer on life, knowing providers communicate with each other, access to complementary therapies, and stress reduction. Participants also expressed positive changes, including contact with other cancer survivors.
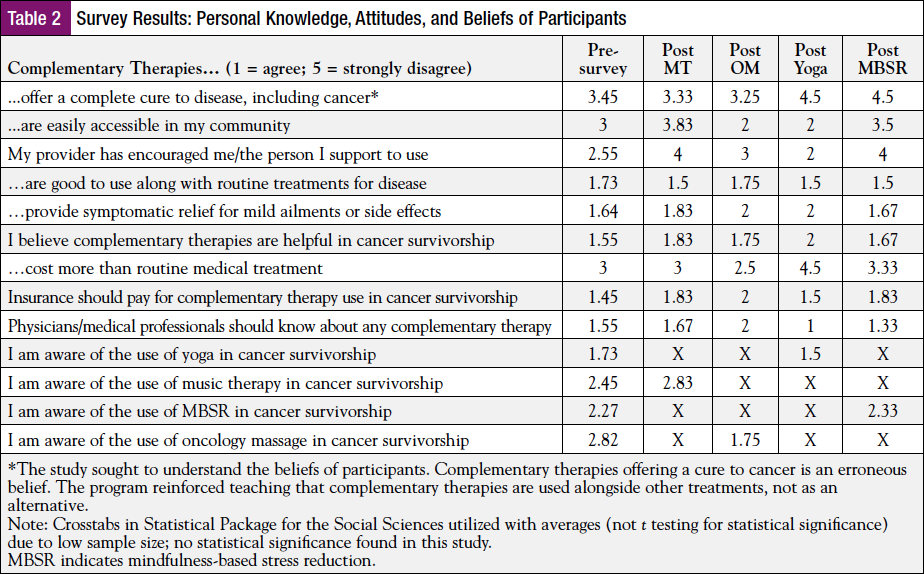
Knowledge, attitudes, and beliefs were scored using Crosstabs in Statistical Package for the Social Sciences (SPSS) software (Table 2). SPSS software is a software package utilized for cross tabulation of data that allows for better insight of data with limited sample sizes. Participants were asked about knowledge, attitudes, and beliefs about complementary therapies in the preprogram survey. These questions asked them to rank, on a scale of 1 to 5, whether they agreed (designated with 1) or disagreed (designated with 5) or were somewhere in between. They were asked the same question regarding the complementary therapy in the postprogram session to observe any differences following attendance in the program.
Participants were asked to score their intent to use the information, skills, treatment learned, and likelihood to encourage other cancer survivors to participate in the specific treatment. All of the complementary therapies had a very strong intent to utilize score with the exception of music therapy. This is likely because music therapy is not well understood, hard to obtain, and costly.
Reflective surveys were sent to participants 6 weeks following completion of the program. Five of the 9 participants who agreed to participate mailed back their reflective survey for inclusion in this project. Participants were asked about what complementary therapies they were using, barriers to use, and what they would like to see in the future. Participants stated they were using yoga techniques, MBSR exercises, and discussed their appreciation for recognizing what they have available to them. Some of the barriers to use of the therapies included fatigue and cost of complementary therapies. Participants felt that the music therapy and yoga sessions were less needed because many were already attending yoga classes through other cancer survivorship programs. For future presentations, participants stated they would like to see more information on cancer education, meditation, yoga, cancer-fighting ingredients in the kitchen, effects of chemotherapy on daily function, ways to handle memory loss, tai chi, exercises to help during and postcancer treatment, and acupuncture. Participants also expressed wanting to have more active participation, less sugary treats, and more publicity in the future for better attendance for a future program. One participant stated: “The program was very helpful and would be useful to someone with a new diagnosis. I had already found the resources to help with my recovery, but it was good to learn more.”
Postprogram phone calls were made 3 months following completion of the program. Participants were asked about their utilization of the complementary therapies, barriers to use, and what they would like to see in the future. Some of the therapies still being utilized included OM, chair yoga, meditation, yoga, tai chi, and essential oils. Participants stated they had encountered few barriers to utilization of complementary therapies except cost, but expressed that in their experience these therapies were worth the cost. They also stated other barriers included accessing or finding the time, having the energy to engage in these activities, and memory loss from chemotherapy-induced memory loss, or chemo brain. For future sustainability, participants stated they would like to see more chair yoga, more outdoor activities, engagement with other survivors in the community in coffee clubs or other social groups, cancer information groups, and more availability of services in the rural county. One participant stated: “I really enjoyed the program; it is so helpful. It is a way of knowing you’re not just a number. It has been 6 years for me, but it is still a huge part of my life. The longer it goes, the more important it is to me. You are just getting through and surviving the first couple of years after treatment—just getting through it you can’t focus on anything else.”
Other survivors spoke about wanting to be a part of the project in the future. One participant stated: “I would love to continue being a part of this project. I don’t know if I got more out of the experience as a patient or a presenter. Being a cancer survivor really gives you a unique perspective.”
Discussion
Complementary therapies have gained a great deal of interest in cancer survivorship for various reasons, including symptom control and overall feelings of well-being.12 This study sought to determine the unmet needs of cancer survivors; understand knowledge, attitudes, and beliefs of cancer survivors related to cancer survivorship; and determine intent to use complementary therapies following participation in a cancer survivorship pilot program. Many of the participants in this study admitted to having several unmet needs, as indicated by the results. Participants were very satisfied with the content of each of the programs and were utilizing several of the complementary therapies presented. Participants also expressed their desire for continuation of a cancer survivorship program in this rural location.
Studies have demonstrated there are unmet needs in cancer survivorship that complementary therapies can assist in meeting.13 Other studies on the use of complementary therapies in survivorship have been consistent with barriers related to chemo brain, fatigue, and lack of time for use of complementary therapies.14 Programs have also demonstrated participant satisfaction with the use of complementary therapies in cancer survivorship for various reasons, including symptom control.14 This pilot study demonstrated that there are not only unmet needs in cancer survivorship, but that complementary therapies are a method of meeting some of those needs. This study also demonstrated intent to use and actual utilization of the complementary therapies presented in the program.
Strengths and Limitations
A key limitation of this project was the number of participants, the limited age range of participants, and attendance of only 1 male. Many of the women who attended came from a specific group of women who met through a support group. Participants have suggested they felt more marketing should be done to assist in making this more successful for future sessions.
Another limitation was the lack of caregiver attendance. Caregivers were invited because survivors have stated the desire to have family be a part of the survivorship experience.4,5,15 A possible reason that no caregivers attended may be because they have their own support group, and because they need their own separate time to express their own unmet needs away from the person they are supporting.
One final limitation was the limited buy-in from providers. No primary care providers in the county reached out or responded to the mailers. This was likely due to the fact that with full patient schedules and current provider shortages, primary care providers have limited capacity to take on additional commitments.
There were several strengths to this study, including the number of attendees compared with other programs in the area. Other programs in the area have 3 to 5 participants per program with attrition throughout the program. This program had higher attendance at the final session. Another strength was the number of interested participants who want to be a part of making this successful in the future.
Buy-in from the community, including grant funding, was a strength. No marketing was paid for, food and beverages were donated by a local chain restaurant, and the local library donated the use of its conference room.
Implications for Nursing Practice
This project clearly indicated there is a role for nursing in meeting the unmet needs of the cancer survivorship population. Nurses and other patient navigators are involved throughout the many transitions cancer survivors experience from diagnosis through survivorship. They play a vital role in assisting cancer survivors in navigating through these transitions effectively.
Another implication of this study is the need for improved education in cancer survivorship. There is no standardized educational component for education for cancer survivors in medical schools, advanced practice nursing education, physician assistant education, or nursing schools. The George Washington Institute offers free online learning, but this is a limited time grant offering.10 More research in survivorship needs to be done, but more education needs to take place between oncology and primary care providers to ensure the transition between the two is more seamless for cancer survivors. Initiatives increasing the number of nurse practitioners providing survivorship care and improving the nurse practitioner curriculum of survivorship care will achieve cost-effectiveness of cancer survivorship care.16 Advanced practice nurses must educate themselves to understand the unmet needs of cancer survivors and encourage cancer survivors to continue appropriate cancer care and follow-up. The utilization of patient navigators along with additional transition tools to improve the cancer survivorship experience are other venues that warrant further exploration.
Conclusions
This pilot project demonstrated there are cancer survivors living with many unmet needs and that there is more work to be done to determine whether formal cancer survivorship programs fulfill those needs. This program displayed participant intent to use and actual use of complementary therapies offered in the sessions. Participants have requested a role in sustaining this program in the future.
There is much more to learn about the unmet needs of cancer survivors and the role of nurse and patient navigators in cancer survivorship. A sustained cancer survivorship program would be helpful in determining the effectiveness of such a program. Collection of data related to adherence to cancer survivorship plans of care, secondary and recurrent cancer rates, and participant fear of recurrence would be helpful in determining the effectiveness of these programs long-term.
References
- American Cancer Society. Cancer Facts and Statistics. www.cancer.org/research/cancer-facts-statistics.html. Accessed March 1, 2019.
- American Society of Clinical Oncology. Building a Survivorship Care Program. www.asco.org/practice-policy/cancer-care-initiatives/prevention-survivorship/survivorship/survivorship-0. Accessed March 1, 2019.
- Weaver KE, Geiger AM, Lu L, Case LD. Rural-urban disparities in health status among US cancer survivors. Cancer. 2013;119:1050-1057.
- Burke NJ, Napoles TM, Banks PJ, et al. Survivorship care plan information needs: perspectives of safety-net breast cancer patients. PloS One. 2016;11:e0168383.
- DeGuzman P, Colliton K, Nail CJ, Keim-Malpass J. Survivorship care plans: rural, low-income breast cancer survivor perspectives. Clin J Oncol Nurs. 2017;21:692-698.
- Smith S, Singh-Carlson S, Downie L, et al. Survivors of breast cancer: patient perspectives on survivorship care planning. J Cancer Surviv. 2011; 5:337-344.
- Viscuse P, Price K, Millstine D, et al. Integrative medicine in cancer survivors. Curr Opin Oncol. 2017;29:235-242.
- Browning KK, Kue J, Lyons F, Overcash J. Feasibility of mind-body movement programs for cancer survivors. Oncol Nurs Forum. 2017;44:446-456.
- Mishel MH. Uncertainty in illness. Image J Nurs Sch. 1988;20:225-232.
- GW School of Medicine & Health Sciences. Cancer Survivorship E-Learning Series for Primary Care Providers. https://smhs.gwu.edu/gwci/survivorship/ncsrc/elearning. Accessed March 1, 2019.
- Hodgkinson K, Butow P, Hunt GE, et al. The development and evaluation of a measure to assess cancer survivors’ unmet supportive care needs: the CaSUN (Cancer Survivors’ Unmet Needs) measure. Psychooncology. 2007;16:796-804.
- Qureshi M, Zelinski E, Carlson LE. Cancer and complementary therapies: current trends in survivors’ interest and use. Integr Cancer Ther. 2018;17:844-853.
- Cutshall SM, Cha SS, Ness SM, et al. Symptom burden and integrative medicine in cancer survivorship. Support Care Cancer. 2015;23:2989-2994.
- Stoutenberg M, Sogor A, Arheart K, et al. A wellness program for cancer survivors and caregivers: developing an integrative pilot program with exercise, nutrition, and complementary medicine. J Cancer Educ. 2016;31:47-54.
- Wieldraaijer T, Duineveld LAM, Donkervoort SC, et al. Colorectal cancer patients’ preferences for type of caregiver during survivorship care. Scand J Prim Health Care. 2018;36:14-19.
- Pandey P, Van Nguyen MS. Achieving the triple aim through doctor of nursing practice–directed breast cancer survivorship care. The Journal for Nurse Practitioners. 2017;13(4):277-283.