Background: Breast cancer is the leading cause of cancer death among women worldwide. Fortunately, frequent mammogram screening among 50- to 69-year-old women decreases breast cancer mortality between 20% and 35%; however, comorbidities, existing in the presence of a breast cancer diagnosis, significantly lower rates of survival. No study to date has analyzed whether certain comorbidities and the biases associated with these diagnoses impact breast cancer screening usage.
Objectives: To determine if screening rates differed among individuals with and without diagnoses of any of the following: diabetes, hypertension, cardiovascular disease (CVD), skin cancer, chronic obstructive pulmonary disease (COPD), arthritis, kidney disease, or depression compared with healthy patients. Secondarily, we assessed whether multiple comorbidities have an increasing effect on breast cancer screening rates.
Methods: Using the 2018 and 2019 Behavioral Risk Factor Surveillance System (BRFSS) data sets, we constructed multivariate logistic regression models to determine the adjusted risk ratios (ARRs) of women receiving breast cancer screening with and without comorbidities. To assess our secondary objective, we constructed a regression model to determine the likelihood of individuals with multiple comorbidities (1, 2-4, 5+) having a breast cancer screening. Regression models were adjusted for race, age, healthcare coverage, and education level. A post hoc regression model was conducted to assess the impact of health insurance on breast cancer screening, accounting for all co-occurring diagnoses and sociodemographic variables.
Results: Our models showed statistically significant associations among mammogram screening and chronic conditions except for diabetes, CVD, and kidney disease. The models showed that individuals who were obese (ARR, 1.02; 95% CI, 1.01-1.04), had hypertension (ARR, 1.09; 95% CI, 1.01-1.18), a skin cancer diagnosis (ARR, 1.05; 95% CI, 1.03-1.07), or arthritis (ARR, 1.02; 95% CI, 1.01-1.04) were more likely to have completed mammogram screening, whereas individuals with COPD (ARR, 0.93; 95% CI, 0.90-0.95) or depression (ARR, 0.96; 95% CI, 0.94-0.98) were less likely to be screened when controlling for age, race, healthcare insurance, and education. The post hoc analysis showed that the odds of women without healthcare insurance were much less likely (odds ratio [OR], 0.32; 95% CI, 0.28-0.37) to have a breast cancer screening than women with healthcare insurance, and it also indicated that the odds of having a screening increased with higher education.
Conclusion: We found that people with co-occurring diagnoses including obesity, diabetes, hypertension, skin cancer, and arthritis completed breast cancer screening more often than those with no comorbidities. Conversely, individuals living with CVD, COPD, and depression were less likely to receive potentially lifesaving breast cancer screening, suggesting biases may be present in women with these diagnoses. Our findings are supported by previous studies showing that breast cancer screening rates are inversely proportional to healthcare insurance and educational attainment. The critical nature of breast cancer screening effectiveness in reducing mortality through early detection highlights the need for greater multidisciplinary care integration to increase preventive health measures in the primary care setting where most chronic conditions are managed, including CVD and depression.
Breast cancer is the leading cause of cancer death among women worldwide,1 and multiple risk factors for breast cancer development exist, including genetics,1 race, and age.2 Fortunately, a meta-analysis by Fiorica in 2016 showed a significantly reduced breast cancer mortality in women who received mammogram screenings.3 Currently, the United States Preventive Services Task Force (USPSTF) suggests women start receiving mammogram screenings for breast cancer at age 50 years, which is 15 years later than the recommended screening age for other comorbidities, such as diabetes.4 The USPSTF recommends biennial mammogram screenings for women 50 to 74 years old who are at average risk of developing breast cancer. If a woman contains risk factors for breast cancer, such as a family history of breast cancer, it is recommended to start screening at age 40 years or earlier, as well as more frequently than biennial, depending on the patient’s preference.5
Previous studies have shown that comorbidities, existing in the presence of a breast cancer diagnosis, significantly lower rates of survival.6,7 The presence of comorbidities may reduce a person’s chances of being screened for cancer as they require attention and resources that may delay further preventive screenings.8 For example, previous research showed that obese individuals were significantly less likely to be screened for colorectal cancer and cervical cancer than non-obese patients, suggesting biases may be present in patients with comorbidities.9 Alternatively, chronic disease diagnoses may lead to increased patient–provider visits and thus more opportunities for breast cancer screening.10 However, there is still likely a delay in screening and follow-up.11
Although current evidence suggested that having comorbidities increases patient–provider visits, no study had analyzed the impact that individual diagnoses have on breast cancer screening and whether biases existed in certain women with these diagnoses. Thus, our primary objective was to determine if screening rates differed among individuals with and without comorbid diagnoses using data extracted from the BRFSS. Other disease conditions available for study within BRFSS included diabetes mellitus, hypertension, CVD, skin cancer, COPD, arthritis, chronic kidney disease, or depression compared with healthy patients. Secondarily, we assessed whether multiple comorbidities had an increasing effect on breast cancer screening rates.
Methods
We combined the 2018 and 2019 BRFSS data sets12 and performed a cross-sectional analysis to examine breast cancer screening prevalence among women with and without comorbid conditions. The BRFSS is a CDC-sponsored annual survey conducted via landline and cell phone interviews. The response rates for the 2018 and 2019 BRFSS were approximately 50%12 and were weighted to be nationally representative.
Respondents were classified as having a breast cancer screening through the following question: “Have you ever had a mammogram screening?” Those who answered yes and affirmed that it was conducted within the past 2 years were coded as having been screened. Those who responded no to having a mammogram screening, or reported that their mammogram screening occurred outside of the 2-year window, were coded as not having a current screening.
Respondents were included if they met screening recommendations based on current USPSTF guidelines. Specifically, they had to be women aged 50 to 74 years. Respondents were excluded if they were male, younger than 50 years, or older than 74 years. Those with a history of breast cancer were included in the analysis, as the screening recommendations continue to be at intervals of 2 years or less in this population, which suggests that they should be included in the analysis. We extracted sociodemographic data, including education level, race/ethnicity, healthcare coverage, age (in 5-year increments), and gender, as well as the aforementioned comorbidities.
Using the combined data sets, we calculated the weighted prevalence of breast cancer screening among individuals with and without comorbidities. We then constructed multivariable logistic regression models to determine the ARR13 of women with and without comorbidities receiving breast cancer screening. To assess our secondary objective, we constructed a regression model to determine the likelihood of individuals with multiple comorbidities (1, 2-4, 5+) having a breast cancer screening. Regression models were adjusted for race, age, healthcare coverage, and education level. A post hoc regression model was conducted to assess the impact of health insurance on breast cancer screening via ORs, accounting for all co-occurring diagnoses and sociodemographic variables. Sampling weights, provided by BRFSS, were adjusted to account for the combined data sets for population-level estimates. Statistical analyses were performed using Stata 16.1 in December 2020.
Results
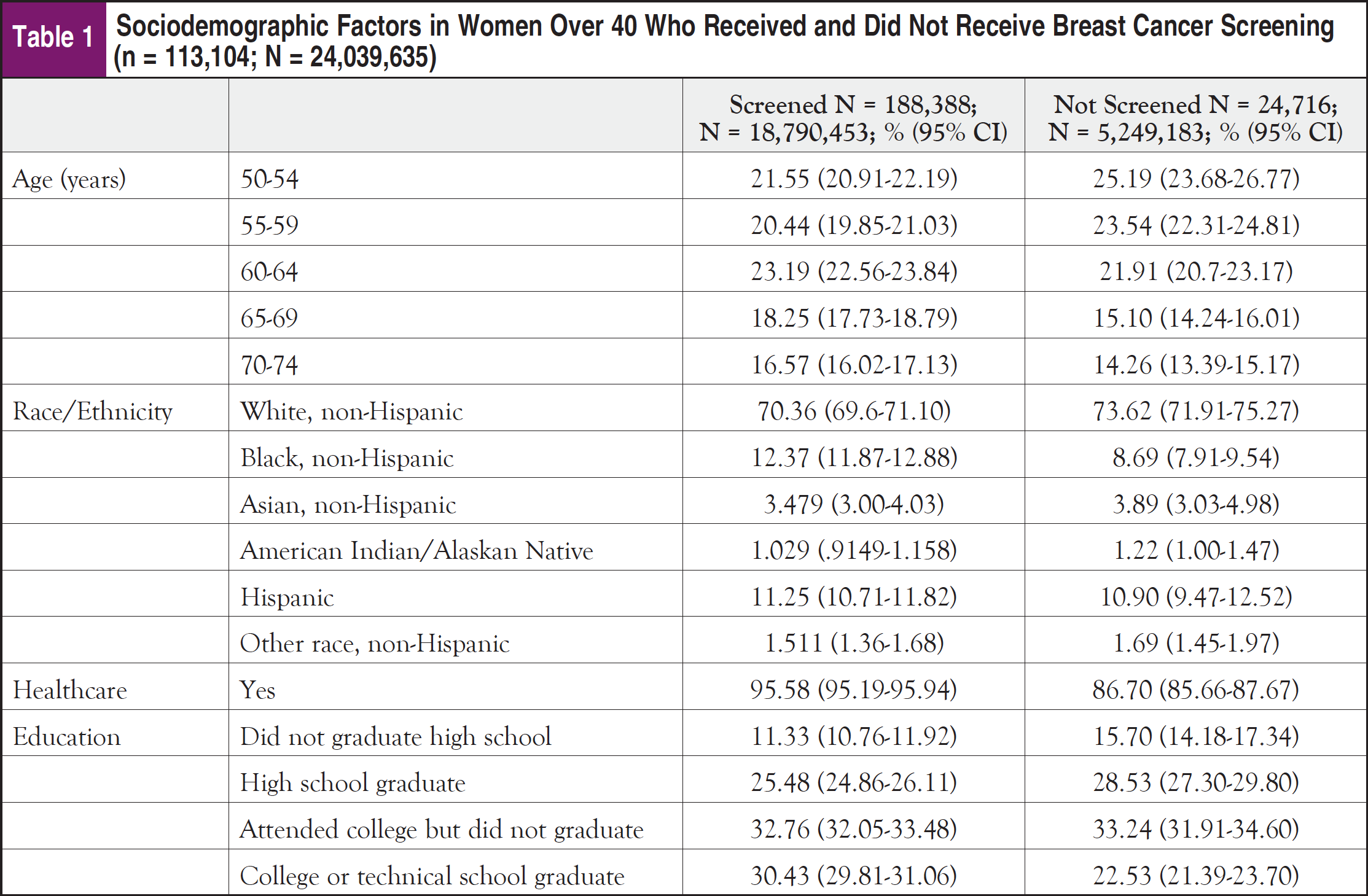
There were 855,704 respondents who completed the survey for combined years. After excluding men and women outside of the 50- to 74-year age range, our sample (n) consisted of 113,104 women, which after sampling weights were applied, provided a population (N) estimate of 24,039,635. Of the 113,104 women, 188,388 (N = 18,790,453) reported having had a breast cancer screening, while 24,716 (N = 5,249,183) had not (Table 1). Breast cancer screening guidelines were most often met among women aged 60 to 64 years (23.19%; 95% CI, 22.56-23.84) followed by women aged 50 to 54 years (21.55%; 95% CI, 20.91-22.19). Women between the ages of 50 and 54 years represented the largest group who did not meet the USPSTF criteria (25.19%; 95% CI, 23.68-26.77), closely followed by those aged between 55 and 59 years (23.54%; 95% CI, 22.31-24.81). Both groups were composed mostly of white women, while black, non-Hispanic women showed the greatest difference between groups—with nearly 3.7% more being in the screened group. Of individuals lacking screening, 13.30% reported having no healthcare insurance, compared with 4.42% having completed a screening while lacking health insurance. Rates of screening were similar among those who graduated high school and partook in some college; however, there was a 7.90% difference among screening rates of those with a college degree—30.43% of the screened population completed college compared with 22.53% in the unscreened. Conversely, a higher percentage (15.70%) of unscreened individuals lacked a high school diploma compared with those who were screened (11.33%; Table 1).
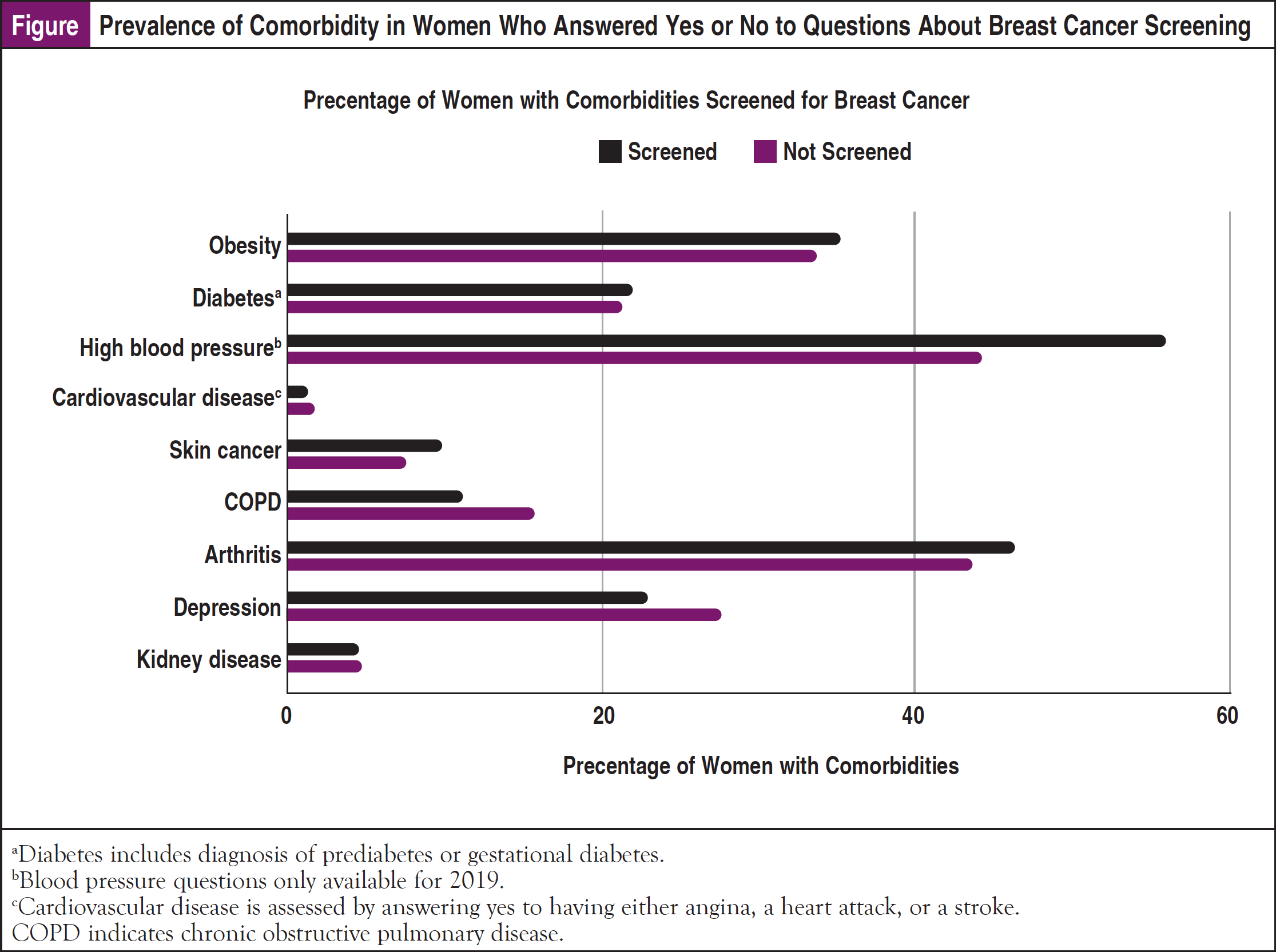
Obesity (body mass index >30) was present in 35.13% (95% CI, 34.40-35.86) of women who completed a mammogram screening, compared with 33.60% (95% CI, 32.22-35.00) of the nonscreened group (Figure). Further, hypertension occurred in 55.96% (95% CI, 51.57-60.26) of screened women compared with 44.23% (95% CI, 36.81-51.92) among the unscreened. Arthritis was also more prevalent among the screened group. Conversely, the prevalence of COPD and depression were higher among the nonscreened group.
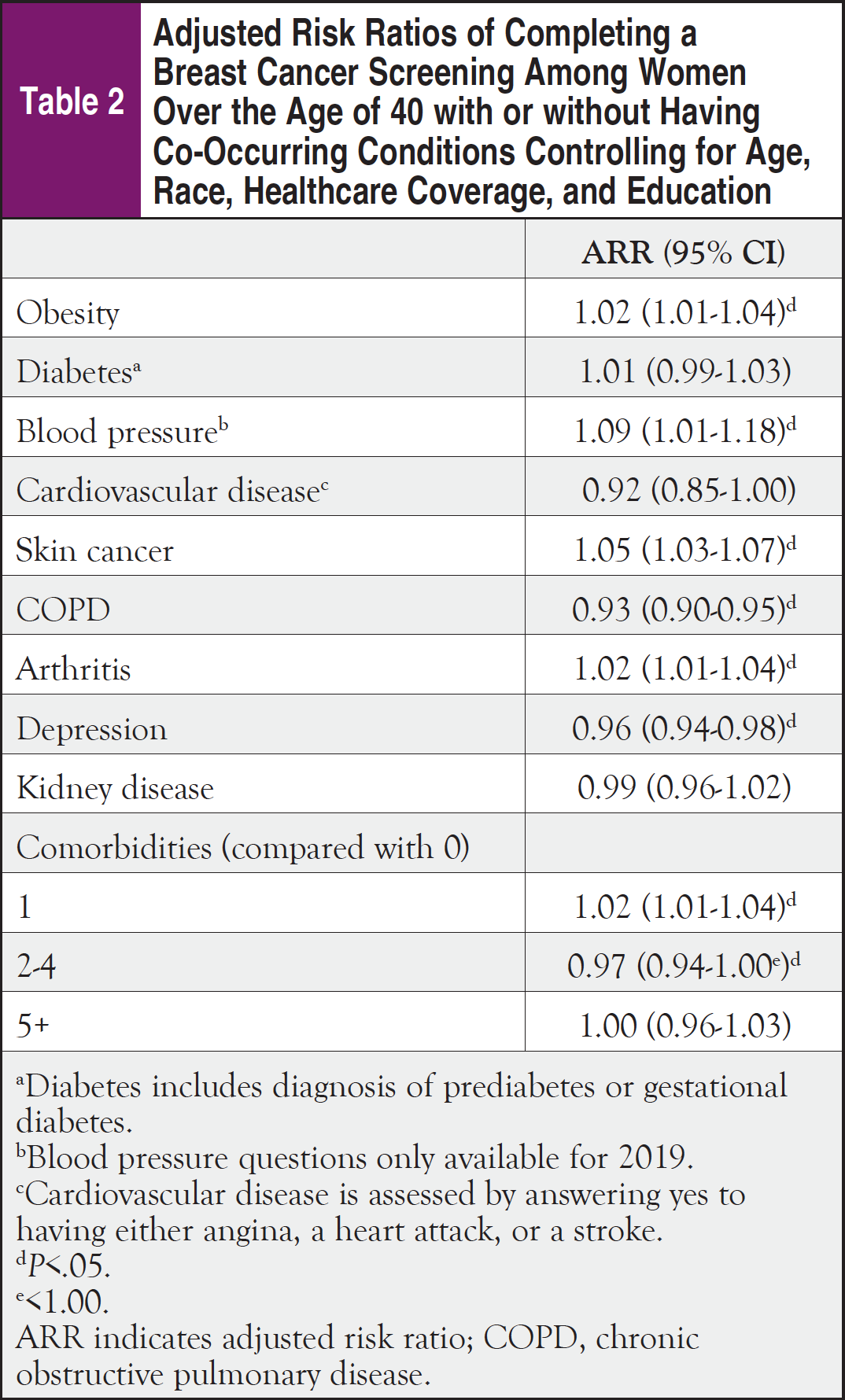
The multivariable logistic regression models found statistically significant associations between mammogram screening and chronic conditions except for diabetes, CVD, and kidney disease. The models showed that individuals who were obese (ARR, 1.02; 95% CI, 1.01-1.04), hypertensive (ARR, 1.09; 95% CI, 1.01-1.18), diagnosed with skin cancer (ARR, 1.05; 95% CI, 1.03-1.07), or arthritis (ARR, 1.02; 95% CI, 1.01-1.04) were more likely to have completed mammogram screening, while individuals with COPD (ARR, 0.93; 95% CI, 0.90-0.95) or depression (ARR, 0.96; 95% CI, 0.94-0.98) were less likely to have been screened when controlling for age, race, healthcare insurance, and education (Table 2).
Compared with women without any comorbidities, women with 1 of the investigated diagnoses were more likely to have completed a mammogram screening (ARR, 1.02; 95% CI, 1.01-1.04), while women with 2 to 4 comorbidities were less likely to have reported being screened (ARR, 0.97; 95% CI, 0.94-0.998; Table 2). Compared with women without any diagnosis, women with 5 or more diagnoses were similarly likely to have completed mammogram screening.
The post hoc analysis showed that the odds of women without healthcare insurance were much less likely (OR, 0.32; 95% CI, 0.28-0.37) to have a breast cancer screening than women with healthcare insurance. This model also indicated that the odds of having a screening increased with increasing education—women with a high school diploma, some college, and those completing college were more likely to have a mammogram screening compared with women who did not complete high school, with ORs of 1.23 (95% CI, 1.06-1.43), 1.33 (95% CI, 1.14-1.54), and 1.82 (95% CI, 1.54-2.14), respectively.
Discussion
Our results showed that women between 50 and 74 years of age diagnosed with hypertension, skin cancer, arthritis, or obesity were more likely to have completed mammogram screening, contrasted with women with CVD, COPD, and depression, who were less likely to have reported being screened. These results suggest that biases may exist in screening women with these diagnoses and may influence physician or patient perspectives. Additionally, women with 2 to 4 comorbidities had the lowest likelihood of completing a mammogram screening compared with those without a co-occurring diagnosis. The increased work hours, administrative burden, and complexity of care for managing multiple comorbidities can lead to physician fatigue and a complex hierarchy of care prioritization that may negatively impact screening implementation.14,15 However, women with 5 or more comorbidities were no more likely to be screened than those without a diagnosis.
Previous studies evaluated associations between chronic conditions and risk for breast cancer and the severity of the breast cancer disease at diagnosis.16,17 However, this was one of the first studies, to our knowledge, to examine the relationship between accumulating chronic conditions and breast cancer screening. Existing evidence evaluating the impact of a co-occurring obesity diagnosis on breast cancer diagnosis, severity, and complications showed that women diagnosed with obesity had increased rates of breast cancer diagnosis, complications in treatment, and worse overall survival.16,17 Similarly, women diagnosed with diabetes had an increased mortality rate once co-diagnosed with breast cancer.18 Increased risk of complications and severity of diagnosis may correlate with women diagnosed with obesity having a higher likelihood to receive a breast cancer screening. Breast cancer treatment may also increase the risk of developing other chronic conditions, such as CVD, although hypertension and depression have been found to have no significant association with breast cancer diagnosis.19,20 Individuals diagnosed with depression are less likely to leave their homes or seek medical attention compared with nondepressed people.21 This may be a fundamental cause for low rates of breast cancer screening in women diagnosed with depression.
Current guidelines for breast cancer screening vary based on the recommending organization. The CDC promotes breast cancer screening guidelines from the USPSTF,22 American Cancer Society,23 American College of Obstetrics and Gynecologists,24 International Agency for Research on Cancer,25 American College of Physicians,26 and the American College of Radiology.27 Most organizations advise women that initiating mammogram screening for breast cancer before age 50 should be a decision made between the patient and physician based on risk versus benefit and personal health factors, citing limited supportive evidence for benefit that would outweigh the risks.22-25 General consensus outlines that women aged 50 to 74 years should receive mammogram screening for breast cancer either annually or biennially. Variation also exists on when to cease breast cancer screening—some organizations cite insufficient evidence for late-age screening,22,25,26 others suggest continued screening as long as overall health is good and life expectancy is 10 years or greater,23 and others advise that ceasing breast cancer mammogram screenings should be based on health status and not age at all.24,27 Notwithstanding the source, recommendations for breast cancer screening modalities—MRI, ultrasound, and clinical breast exams—vary based on individual health risk factors, such as family and personal history, breast tissue density, and lifestyle, along with cost of service, availability of resources, time burden, and health literacy.28
Despite overall progress being made in the United States with decreasing trends for both breast cancer incidence and mortality, there are still disparities between patient populations.29,30 Our post hoc analysis found relationships similar to previous studies when comparing healthcare insurance and breast cancer screening, demonstrating that when healthcare insurance is lacking, so are preventive health assessments.31-33 Additionally, other studies also matched our results for education level and participation in breast cancer screening—higher education being a key predictor for most positive health outcomes.34,35
Based on data analysis from this and previous studies, multidisciplinary care coordination would likely increase access to breast cancer mammogram screening. Multidisciplinary care coordination ranges from integrating screening templates into intake forms or electronic health record documentation, increasing availability of patient and provider education materials, implementing protocols for care coordination between clinic offices or facilities, and providing incentives for facilities with higher-risk patient groups to collaborate with breast cancer screening programs.36 Additionally, a recent systematic review found overwhelming evidence that provider recommendation significantly aids adherence to preventive screening in most cancers.37 This was consistently validated across a variety of populations, including urban, rural, geographic regions, and various ethnicities. Therefore, communication campaigns should involve providers and be targeted to populations with risk factors for screening noncompliance, such as lack of higher education and healthcare insurance.
Integrating patient navigation—“a community-based service delivery intervention designed to promote access to timely diagnosis and treatment of cancer and other chronic diseases by eliminating barriers to care”—into multidisciplinary care models is an effective and scalable model to address multifaceted challenges in the healthcare system, such as those surrounding cancer screening and management.38 Many patients encounter complex barriers to accessing cancer preventive care, including financial burden, lack of transportation, and health literacy limitations. Applying risk stratification based on health status in addition to age-based guidelines for the practical implementation of breast cancer screening recommendations could result in a more individualized approach and therefore greater patient adherence.39,40 Patient navigators (PNs), whether identified as nurses, medical assistants, social workers, or community health workers, are uniquely positioned to partner with physicians and patients to enact these measures, with data showing improved efficacy with utilization for cancer screening, diagnostic resolution, treatment, and clinical trial enrollment along with increased patient satisfaction with cancer care.38
Our recommendations encompass further research into the guidelines for breast cancer screening, especially focusing on benefit–risk analysis for increased or decreased screening, along with expanding the age range to reflect current trends in health outcomes. Additionally, we suggest increased utilization of PNs to overcome the complex barriers to accessing cancer screening and management. Engaging PNs in multidisciplinary teams improves physician and patient care coordination while tailoring individualized healthcare services delivery to specific subgroups of patients according to other existing health and personal risk factors, such as comorbidities. Further, to increase access to breast cancer screening, increasing women’s health screenings using mobile care clinics or telehealth may improve screening rates and earlier detection of breast cancer.41 Overall, increased efforts are warranted to decrease the disparity in women receiving breast cancer screening who have been diagnosed with CVD, COPD, and depression.
Strengths and Limitations
The BRFSS data utilized for this study consisted of a large sampling size and thus provides a sufficient statistical strength for data analysis. A limitation in using BRFSS data was the method of data collection via self-reporting survey; response bias could negatively impact results. In addition, because this study was a cross-sectional analysis, it cannot be used to determine causation but rather correlation for influences on breast cancer screening.
Conclusions
Results from our study showed that people with co-occurring diagnoses, such as hypertension, skin cancer, arthritis, or obesity, were significantly more likely to have completed breast cancer screening compared with those with no comorbidities. Conversely, individuals with CVD, COPD, and depression were less likely to receive potentially lifesaving breast cancer screening through mammogram screening, a previously unstudied area in breast cancer research. Our findings are supported by previous studies showing that breast cancer screening rates are inversely proportional to healthcare insurance and educational attainment levels. The critical nature of implementing breast cancer screening through mammogram screening is due to the evidence that mortality can be reduced through early detection and prevention measures. Resulting recommendations from this study highlight the need for greater multidisciplinary care integration to increase preventive health measures, such as breast cancer screening, in primary care settings where most chronic conditions are managed, including CVD and depression.
Role of Funding Source
This study was not funded.
Conflict of Interest
We declare no conflicts of interest.
References
- Sung H, Ferlay J, Siegel RL, et al. Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71:209-249.
- Stapleton SM, Oseni TO, Bababekov YJ, et al. Race/ethnicity and age distribution of breast cancer diagnosis in the United States. JAMA Surg. 2018;153:594-595.
- Fiorica JV. Breast cancer screening, mammography, and other modalities. Clin Obstet Gynecol. 2016;59:688-709.
- Tracer H, Mohnot S. Screening for prediabetes and type 2 diabetes mellitus. Am Fam Physician. 2022;105:73-74.
- US Preventive Services Task Force. Breast Cancer: Screening. https://uspre ventiveservicestaskforce.org/uspstf/recommendation/breast-cancer-screening. Accessed April 4, 2022.
- Zhao XB, Ren GS. Diabetes mellitus and prognosis in women with breast cancer: a systematic review and meta-analysis. Medicine (Baltimore). 2016;95:e5602.
- Ewertz M, Land LH, Dalton SO, et al. Influence of specific comorbidities on survival after early-stage breast cancer. Acta Oncol. 2018;57:129-134.
- Cofie LE, Hirth JM, Berenson AB, Wong R. Chronic comorbidities and receipt of breast cancer screening in United States and foreign-born women: data from the National Health Interview Survey. J Womens Health (Larchmt). 2019;28:583-590.
- Seibert RG, Hanchate AD, Berz JP, Schroy PC 3rd. National disparities in colorectal cancer screening among obese adults. Am J Prev Med. 2017;53:e41-e49.
- Fleming ST, Pursley HG, Newman B, et al. Comorbidity as a predictor of stage of illness for patients with breast cancer. Med Care. 2005;43:132-140.
- Yasmeen S, Xing G, Morris C, et al. Comorbidities and mammography use interact to explain racial/ethnic disparities in breast cancer stage at diagnosis. Cancer. 2011;117:3252-3261.
- Centers for Disease Control and Prevention. 2019 BRFSS Survey Data and Documentation. www.cdc.gov/brfss/annual_data/annual_2019.html. Published August 31, 2020. Accessed April 21, 2021.
- Norton EC, Miller MM, Kleinman LC. Computing adjusted risk ratios and risk differences in Stata. The Stata Journal. 2013;13(3):492-509.
- Ahmad A. Managing physician fatigue. Gastrointest Endosc Clin N Am. 2021;31:641-653.
- Sverrisdóttir IS, Rögnvaldsson S, Thorsteinsdottir S, et al. Comorbidities in multiple myeloma and implications on survival: a population-based study. Eur J Haematol. 2021;106:774-782.
- Argolo DF, Hudis CA, Iyengar NM. The impact of obesity on breast cancer. Curr Oncol Rep. 2018;20:47.
- Lee K, Kruper L, Dieli-Conwright CM, Mortimer JE. The impact of obesity on breast cancer diagnosis and treatment. Curr Oncol Rep. 2019;21:41.
- Bernard L, Reix N, Benabu JC, et al. [Breast cancer and diabetes mellitus: complex interactions]. Gynecol Obstet Fertil. 2016;44:701-711.
- Yang Y, Lynch BM, Hodge AM, et al. Blood pressure and risk of breast cancer, overall and by subtypes: a prospective cohort study. J Hypertens. 2017;35:1371-1380.
- Sun HL, Dong XX, Cong YJ, et al. Depression and the risk of breast cancer: a meta-analysis of cohort studies. Asian Pac J Cancer Prev. 2015;16:3233-3239.
- Sheeran T, Rabinowitz T, Lotterman J, et al. Feasibility and impact of telemonitor-based depression care management for geriatric homecare patients. Telemed J E Health. 2011;17:620-626.
- Siu AL. Screening for Breast Cancer: U.S. Preventive Services Task Force Recommendation Statement. Ann Intern Med. 2016;164:279-296.
- Oeffinger KC, Fontham ETH, Etzioni R, et al. Breast cancer screening for women at average risk: 2015 guideline update from the American Cancer Society. JAMA. 2015;314:1599-1614.
- Committee on Practice Bulletins – Gynecology. Practice Bulletin Number 179: Breast Cancer Risk Assessment and Screening in Average-Risk Women. Obstet Gynecol. 2017;130:e1-e16.
- Fitzgerald SP. Breast-Cancer Screening – viewpoint of the IARC Working Group. N Engl J Med. 2015;373:1479.
- Qaseem A, Lin JS, Mustafa RA, et al. Screening for breast cancer in average-risk women: a guidance statement from the American College of Physicians. Ann Intern Med. 2019;170:547-560.
- Monticciolo DL, Newell MS, Hendrick RE, et al. Breast cancer screening for average-risk women: recommendations from the ACR Commission on Breast Imaging. J Am Coll Radiol. 2017;14:1137-1143.
- Chetlen A, Mack J, Chan T. Breast cancer screening controversies: who, when, why, and how? Clin Imaging. 2016;40:279-282.
- Toriola AT, Colditz GA. Trends in breast cancer incidence and mortality in the United States: implications for prevention. Breast Cancer Res Treat. 2013;138:665-673.
- Seely JM, Alhassan T. Screening for breast cancer in 2018 – what should we be doing today? Curr Oncol. 2018;25(suppl 1):S115-S124.
- Wyatt TE, Pernenkil V, Akinyemiju TF. Trends in breast and colorectal cancer screening among U.S. adults by race, healthcare coverage, and SES before, during, and after the great recession. Prev Med Rep. 2017;7:239-245.
- Cooper GS, Kou TD, Dor A, et al. Cancer preventive services, socioeconomic status, and the Affordable Care Act. Cancer. 2017;123:1585-1589.
- Berland LL, Monticciolo DL, Flores EJ, et al. Relationships between health care disparities and coverage policies for breast, colon, and lung cancer screening. J Am Coll Radiol. 2019;16(4 Pt B):580-585.
- Karadag Arli S, Bakan AB, Aslan G. Distribution of cervical and breast cancer risk factors in women and their screening behaviours. Eur J Cancer Care (Engl). 2019;28:e12960.
- Damiani G, Basso D, Acampora A, et al. The impact of level of education on adherence to breast and cervical cancer screening: evidence from a systematic review and meta-analysis. Prev Med. 2015;81:281-289.
- Selby K, Bartlett-Esquilant G, Cornuz J. Personalized cancer screening: helping primary care rise to the challenge. Public Health Rev. 2018;39:4.
- Peterson EB, Ostroff JS, DuHamel KN, et al. Impact of provider-patient communication on cancer screening adherence: a systematic review. Prev Med. 2016;93:96-105.
- Nirmal AA, Rodríguez-Colón SM, Costalas S, Lengerich EJ. Patient navigation and cancer-related care: policy solutions to improve access to Pennsylvania’s complex system of care. Journal of Cancer Policy. 2020;25:100231.
- Gagnon J, Lévesque E, Clinical Advisory Committee on Breast Cancer Screening and Prevention, et al. Recommendations on breast cancer screening and prevention in the context of implementing risk stratification: impending changes to current policies. Curr Oncol. 2016;23:e615-e625.
- Harkness EF, Astley SM, Evans DG. Risk-based breast cancer screening strategies in women. Best Pract Res Clin Obstet Gynaecol. 2020;65:3-17.
- Salmani H, Ahmadi M, Shahrokhi N. The impact of mobile health on cancer screening: a systematic review. Cancer Inform. 2020;19:1176935120954191.