Background: Adolescent and young adult (AYA) survivors—particularly those from historically underserved groups—may encounter different challenges than other cancer survivors.
Objectives: To assess needs of female AYA breast cancer (BC) survivors who may be from racial/ethnic minority groups, and/or have low income, live outside urban settings, and/or have metastatic cancer, as well as the perspectives of those who provide services to them.
Methods: Focus groups were held with 33 survivors who had received services from a community center for BC survivors. Ten professionals (primarily oncology nurse navigators) who provide services to AYAs in different healthcare systems were recruited for key informant interviews. Themes were identified from audio recordings and interview/focus group notes.
Results: Although AYAs face many of the same challenges as other cancer survivors, some concerns, such as childcare and infertility, are especially salient for them. Black women may encounter “race-based nonchalance,” and many women do not receive needed referrals. Financial toxicity is particularly problematic because many AYAs are in the early years of employment. Both patients and providers express a need for greater care coordination and better communication among healthcare team members and between patients and service providers.
Conclusions: An underlying theme was the need to educate providers to think beyond medical diagnosis and treatment and communicate information about long-term symptom management, signs of recurrence or metastasis, and complementary therapies—particularly mental health services. This communication must take into account social determinants of health, such as race/ethnicity and health literacy. The results underscore the key role navigators can play in providing support or facilitating referrals tailored to individual AYA needs. Findings also highlight the importance of continued advocacy and public education to raise awareness that insurance does not eliminate the financial burdens that AYA cancer survivors may face.
Although less common than in older adults in the United States, adolescents and young adults (AYAs) aged 15 to 39 years can have breast cancer (BC).1 It is the most commonly diagnosed cancer among female AYAs aged 30 to 39 years, with an estimated 11,100 females expected to be diagnosed in 2020.1 While AYAs tend to be diagnosed at earlier stages for most cancers compared with older adults, female AYAs are more likely to experience a delay in diagnosis of BC.1 This may be due to various factors, including annual mammography screening beginning after age 40 years and limited healthcare access.2 In female AYAs, delays in BC diagnoses often contribute to more advanced tumors and a need for more aggressive treatment, which lead to various unmet needs in their lives.3
Female AYAs are at a different developmental phase than older females, thus BC treatments and their effects likely impact them in a different way. AYAs have critical developmental milestones, including completing education, becoming financially independent, securing employment, having romantic relationships, having children and parenting, establishing autonomy, and developing personal identity.4
Despite increasing awareness of AYAs with cancer, few studies consider underserved groups, such as racial/ethnic minorities and low-income individuals. The BC incidence in black and Hispanic female AYAs is higher than in white female AYAs1; mortality rates in black females with cancer in their 30s are nearly double compared with those of white females.5 Black AYAs are also less likely to be enrolled in clinical trials.6 AYAs with cancer experience more severe financial toxicity than the general population because of limited financial assets and inadequate insurance coverage.7-9 Surveillance is important, but low-income AYA survivors may have barriers that make monitoring their cancer or complying with preventive measures difficult.10 Although racial/ethnic disparities in financial hardship are well documented in older adult cancer research,11,12 studies evaluating the needs of racial/ethnic minority and/or low-income AYA survivors are limited.
Therefore, the focus of this needs assessment was to assess the needs of female AYA BC survivors who may be most likely to experience health disparities: those from racial/ethnic minorities, and/or have low income, live outside urban areas, and/or those with metastatic BC (mBC). This information can guide providers in developing age-appropriate supports/resources, particularly for those from historically underserved groups.
Methods
The Breast Cancer Resource Center of Texas (BCRC) is a community-based nonprofit community organization providing individualized support from the moment of diagnosis, through treatment and into survivorship. The staff includes certified patient navigators who are BC survivors. They strive to empower those touched by BC to become active and knowledgeable participants in their healthcare.
BCRC received a grant from the CDC to develop an integrated response to optimize care for AYA survivors. As part of the needs assessment process, the BCRC contracted with The University of Texas at Austin School of Nursing to conduct focus groups with female AYAs and key informant interviews with healthcare professionals. The BCRC staff and the needs assessment team jointly developed a semistructured interview and a focus group guide that addressed information resources, gaps in services, desired supports/services, barriers to care, and provider interactions. Specific questions are shown in Table 1. The University of Texas at Austin Institutional Review Board (IRB) deemed the research exempt from IRB oversight because it did not meet the criteria for human subjects research. To meet BCRC’s desire for timely information about local AYA needs to guide program development, data were collected quickly, resulting in a small sample size.
Focus Group Procedures
The research team leader, an experienced focus group facilitator, has conducted numerous research and evaluation projects in cancer prevention and survivorship. She teamed with the BCRC grant specialist, a public health professional experienced in program planning and evaluation who does not provide direct client services, to conduct the focus groups.
Participant Recruitment
The BCRC staff utilized their online data base to generate a report of their clients who had been diagnosed at age 45 years or younger. The staff then invited clients to specific groups based on their demographic characteristics. Clients who identified as being of Hispanic descent were invited to the Hispanic focus group. Clients with black or African American listed as their race were invited to the African American focus group. Clients with a metastatic diagnosis were invited to the metastatic focus group. Clients without insurance or those who only had access to government-funded health insurance during the time of their diagnosis and/or treatment were invited to the underinsured/uninsured focus group. Finally, clients living in a zip code located at least 30 minutes from their medical home and/or oncology care team were invited to the “rural” focus group.
Once clients were invited to their respective groups, the grant specialist coordinated the logistics of when each focus group would be conducted. Although the 5 focus groups were originally intended to address low-income, rural, and ethnic/racial status and metastatic disease separately, the group composition often included women whose life experience touched on multiple underserved contexts (eg, women could be both a member of a minority group and a low-income group). All women in the metastatic focus group had metastatic cancer.
The focus groups were conducted and recorded on Zoom. To address member checking, the focus group moderator summarized major highlights she had heard toward the end of each group and invited participants to clarify or expand on them. After each group, the assistant moderator (the grant specialist) and the moderator debriefed about major themes they heard in the groups. The assistant moderator shared her notes with the moderator, who used both sets of notes and audio recordings to identify key themes and specific examples to illustrate those themes. The guidance of Kidd and Parshall13 informed the analysis of the focus group data. The questions in the focus guide served as initial coding categories, but the analysis was expanded to include other topics raised by AYAs in the focus groups.
Key Informant Interview Procedures
BCRC staff invited professionals in the community who had worked with BCRC, treated BCRC clients, and/or referred their patients to BCRC services to participate in key informant interviews. Once they had agreed, the grant specialist introduced interested professionals to the interviewer, who then coordinated when each interview would be conducted. Ten professionals from organizations/clinics in the Central Texas area were interviewed by a School of Nursing researcher. They included 7 nurse navigators, 1 physical therapist, 1 social worker, and 1 genetic counselor (all hereafter referred to as “professionals”).
The research team leader trained the interviewer, who is a pediatric nurse and a PhD nursing student, in the interview protocol. The interviews were conducted via telephone and audio recorded. The interviewer subsequently coded the interviews based on her notes and the recordings. The interview questions served to structure the initial coding, although the codes were expanded to include other topics, such as health literacy, addressed by the key informants. The analytic structure proposed by Miles and Huberman14 was used to organize the coding into a cross-case display. To increase trustworthiness of the analysis, the interviewer discussed her codes with the needs assessment team leader, who also listened to a subset of the taped interviews to check the interview credibility and initial coding. The needs assessment team leader summarized the findings from these codes, which the interviewer then reviewed.
Results
Focus Group Findings
Sample Description
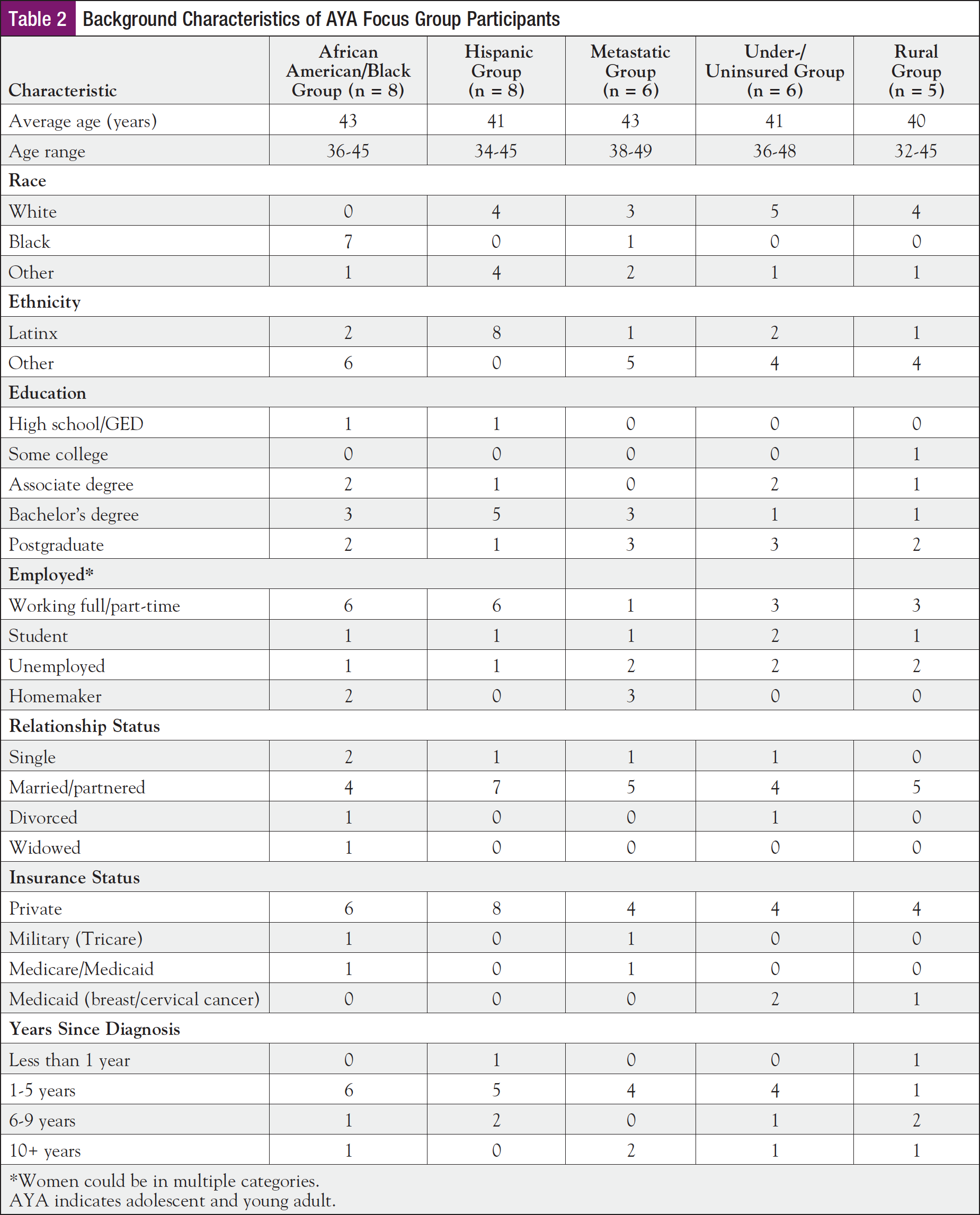
Thirty-three participants were recruited. Ninety-four percent had at least some college, 58% were employed, 75% were married, and 79% had private insurance. Twenty-four percent were black; 42% were Hispanic (see Table 2 for breakdown by focus group).
The average age of 41 years was consistent with the target age range identified in the program’s grant, which was under age 45; 61% were diagnosed with cancer 1 to 5 years previously.
Helpful Services and Resources
Women most frequently discussed complementary treatments, particularly mental health services, financial assistance (including copays), and support groups/navigation services as helpful supports/resources. Support groups and navigation services were discussed as good places to ask questions or clear up miscommunications because it is sometimes difficult to reach providers by phone. One woman described navigators as “people who go above and beyond.” Another stated: “Just have to have enough courage to ask the questions.”
Some women mentioned online information, although many stressed the need to find trusted online sources. A few women avoided seeking out certain information until they needed it, while others were hypervigilant about locating whatever they could find. Several participants looked to their oncology providers for information and described them as helpful when they could take the time and “break everything down for me” or respond to e-mailed questions. Some women found the sheer volume of information, particularly when initially diagnosed, to be overwhelming. By contrast, one found the large binder of information useful and termed it her “cancer bible.”
Needed Supports and Services
Several BC survivors requested more comprehensive and coordinated services, particularly after active treatment. Some women felt supports “taper off” or “fade away” over time. One stated this is the time when the posttraumatic stress disorder sets in, so access to mental health services to process those emotions is particularly important. When she told her nurse and oncologist about her anxiety and depression, she was referred for mental health services financed by a local nonprofit. Women wished that they could be told about that service sooner. An underlying theme was that the survivor has to be proactive to identify information/resources.
Some women mentioned that their partners needed support. Help communicating with children about their parent’s cancer, and even age-appropriate training for children on how to help care for their mothers, such as emergency training, were discussed. One woman pointed out this would be particularly important for single mothers.
Barriers to Accessing Resources
Even when programs are available, focusing energy on seeking them out and applying for them are difficult. Women have such limited time and “bandwidth” to go for treatment, work, and take care of children. Some women (particularly in outlying areas) were aware of services that could be useful, but the drive creates problems, especially when dependent on family members for transportation.
When asked if race/ethnicity, LGBTQ status, insurance status, or other issues created barriers to services, some women expressed that black women could experience treatment delays, or receive different treatments compared with white women. One woman stated that “As black women, we constantly have to dig for information because doctors don’t seem to want to provide the whole picture to us.” Another woman described it as “race-based nonchalance” and stated that twice a black nurse stepped in to stop it.
Financial Concerns
Financial issues were discussed repeatedly. For some women, insurance did not cover needed services, particularly mental health services. Even for those insured, copays, deductibles, and other “hidden costs” created problems and were confusing. And taking time off from work can strain finances, and changing jobs can change insurance status. In particular, women with mBC experience financial burdens for many years.
Help navigating insurance coverage was requested in every group. One woman pointed out that patients don’t learn costs until they are scheduled for the service, and that makes financial planning difficult. Help may be available, but the application process can be daunting, especially when coping with treatment effects. Available financial support may not cover all extra expenses or be available to those women in the AYA age-group. One stated, “It’s almost like you have to be…completely out of money to get some assistance.”
Communication and Relationship with Providers
When asked what information they wished providers had communicated to them, some women wanted more information about long-term treatment effects. One stated: “Doctor tends to just worry about like the cancer and making sure that’s under control and less about the side effects caused by like the chemotherapy and stuff.” The importance of listening to patients was also discussed.
One recommendation was better connections between community navigators and the patients’ healthcare team. Having someone checking in periodically to see how survivors were doing was also suggested. These contacts provide an opportunity to ask questions or clear up miscommunications, because it is sometimes difficult to reach providers by phone. Participants expressed that patients do not always know they have a choice about treatment. One stated: “I’m grateful that I was able to push back. I wished that other women knew you don’t have to do what…is asked of them.”
The need to inform patients about signs and symptoms of recurrence and mBC was discussed. Patients may need to hear the information multiple times, because they may not be able to process it immediately. As one stated: “So confusing and so terrifying.”
Women in the mBC group wished providers had explained about palliative care earlier, including end-of-life planning. They also wanted information about mBC earlier, particularly symptoms indicating mBC versus recurrence, so they could make “good decisions.” One stated: “If you’re running a short distance, you train totally different than for a marathon. It doesn’t feel like there’s a lot of information on how to pace yourself for the marathon.”
Concerns Specific to AYA Survivors
Although many of the issues discussed impact older as well as younger BC survivors, some issues emerged as particularly concerning for AYAs. Support group meetings during work hours were difficult to attend. A few women discussed delays in getting diagnostic tests, such as mammograms, because of their age. Intimacy issues can also be a concern. Two women discussed childcare needs during medical appointments or complementary treatment services to address mental health, for example.
Many women, particularly in the Hispanic focus group, indicated providers had not discussed fertility preservation or future pregnancy with them. One stated: “My very first oncologist. I told him, I have a concern about premature menopause because I would like to have kids. And he said, do you want to have kids or do you want to live.” Cost can also be a barrier to fertility preservation. Another woman discussed having inadequate time to get information and process it so she could make good decisions about fertility preservation before beginning treatment.
Findings from Key Informant Interviews
The professionals interviewed, who work in different settings, perceived available resources and barriers to accessing them differently. Some see survivors at diagnosis; others interact with them later. Comments illustrating some key themes appear in Table 3.
Perceptions of Existing Services
Professionals described fragmented care. When care is not well coordinated, some necessary services are not made available to patients in a timely manner. If specialized services are not available “in-house” (eg, physical therapy, fertility treatments, genetic testing, complementary therapies), then referrals must be made. One professional expressed that not everyone who is referred makes an appointment. Four professionals stated that it can be difficult for patients to get fertility treatment before they begin their cancer treatments.
Professionals stressed that survivors have different needs, and professionals must take time to build relationships with survivors that will help them determine these needs. For example, those with children at home have childcare needs, while other survivors may need complementary care.
One overarching theme was to determine the best timing for providing resources/information so as not to overwhelm survivors with too much information, especially early in the diagnosis and treatment process. Yet, providers pointed out patients need to be referred earlier for some services.
Eight professionals discussed health literacy, and they considered different issues in this area. Some saw language as the issue. One professional expressed that details about diagnosis can get lost in translation for Spanish-speaking women. Another professional mentioned that patients may appear to agree with what they are told without really understanding it. Others discussed limited understanding of the diagnosis or one’s body, or fear about the diagnosis that might create barriers to accessing services. Concerns arose among professionals that the reading level of written information (particularly genetic testing) may be too advanced. Providers do not always recognize terms that may be unfamiliar to patients, so navigators may take responsibility for explaining terms to patients.
Some professionals pointed out that thinking more holistically about the patients’ needs is a new way of thinking for providers, who are traditionally focused on medical diagnosis and treatment. One stated that as more services and supports become available, providers need to know about them.
Barriers to Services
When asked about barriers that keep patients from accessing available resources, all professionals recognized that insurance coverage deficiencies along with out-of-pocket expenses limit survivors’ access to some resources. Providers might not mention certain services, such as genetic testing or fertility preservation, because they think the patients may not be able to afford them.
A few professionals mentioned immigration status and geographic residence. Even if women can use a service, wait times, transportation, or time to get to the service can create barriers. One professional stated that Latina women tend not to ask questions about what the doctor tells them, and she speculated it could be due in part to feeling embarrassed about not understanding what they are told. On the positive side, one interviewee stated: “Part of the beauty of being in rural, small communities is people pull together because they know you.”
Two professionals expressed concern that black women may experience delays in care because they may not have had access to preventive services. Sometimes that is because of financial constraints, but one respondent suggested that for some women distrust of the healthcare system may cause delays in seeking care.
Concerns Specific to AYA Survivors
Professionals identified childcare as a key concern for AYAs. Without adequate childcare, they may not be able to utilize needed services. Low-income survivors in particular may be working in inflexible settings that do not accommodate their needs. Female AYAs were described as trying to juggle many roles in the context of their cancer.
Support for children is very important to help children understand their mother’s cancer, but this support may not always be available, particularly in rural areas. A somewhat related concern is deciding who should take care of their children if the mothers die.
Body image changes, femininity, sexuality, and premature menopause were mentioned as especially key for AYAs. As one professional stated, AYAs have a lot of life ahead of them, so noncancer treatment issues are particularly important. Only 4 professionals discussed fertility preservation, and they discussed it in the context of lack of availability/referral or cost.
Meeting Survivors’ Needs
Professionals stressed the importance of a more coordinated, holistic system when a patient is diagnosed, because dealing with things preventively can be much more effective.
Immediately available mental health service was also discussed in this regard. One professional emphasized the importance of open and expedient communication that empowers women to make decisions that are in their best interest.
Improvements to the healthcare financing system were also discussed. For instance, an insurance expert was mentioned as a potentially helpful resource. Certain treatments, such as breast reconstruction, aren’t really options for women who can’t afford copays, even if they have insurance. As one professional stated: “We should do better for unfunded, working poor people who don’t qualify for assistance.”
Professionals try their best to fill in the gaps that the often disjointed and financially challenging system does not deliver. For example, one navigator has reached out to day care centers to solicit scholarships for women who need childcare assistance. As another professional stated: “Our basic goal and mission is to get them to treatment somehow.”
Discussion
While previous studies have identified AYAs’ needs, the present study addressed the needs of historically underserved AYA populations. Moreover, 2 information sources were combined: focus groups with AYA BC survivors and key informant interviews with those who provide care to them. Although many of the concerns raised by these participants are not new, this study’s findings underscore that these concerns have yet to be adequately resolved, even as attention to AYA cancer survivors has increased.
Issues discussed by AYA survivors in these groups reflect previously reported literature.15 The survivors and the professionals both recognize that even when resources are available, many barriers to accessing them exist. Financial constraints repeatedly emerged as an issue. Participants recognized the many demands on women in this age-group that increase support needs. Professionals and survivors both stressed the necessity for integrated seamless services, tailored to individuals’ needs, particularly needs arising from this specific developmental stage of life. Additional research is needed to explore how to most effectively provide such integrated services within the constraints of the healthcare system.
Survivors and professionals expressed differing perspectives on the issue of race-related barriers to accessing care. Some professionals suggested distrust of the healthcare system or lack of understanding about cancer and related treatments may impede care for women of color. Black women suggested their providers may have offered them different treatment options compared with their white peers. One woman used the term “race-based nonchalance” to describe differences in treatment experience. Her comment that a black nurse stepped in to help points to the importance of a diverse professional workforce. Taken together, these comments echo the increasing recognition of disparities in access to care and health outcomes for racial and ethnic minorities. Continued research is needed to understand the unique survivorship concerns among minority patients, as well as the deleterious effects of systemic racism on healthcare outcomes for BC survivors.
Both groups discussed the importance of good communication and relationship building between patients and providers. Survivors expressed the need for physicians to give useful, clearly communicated information. The professionals were concerned about not overwhelming women with too much information, particularly early on, and survivors agreed. Their comments point to the importance of matching the timing of information to the BC survivor’s needs and preferences for amount and information modality.
Personal connections are so important; from providers taking time to talk with and listen to survivors to navigators who can “fill in the gaps” and brainstorm how to break down or overcome barriers. The professionals pointed to health literacy issues they believe can hinder understanding, which makes this personal communication especially important. In addition, connections with other AYA survivors who understand what young women with BC are experiencing are valuable for many BC survivors.
Navigators and other members of the healthcare team (eg, nurses) are particularly positioned to take time to explain treatment variations linked to differences in diagnoses, but also steps women can take if they have concerns about their treatment. The information and communication gaps identified both by BC survivors and professionals highlight the key role that navigators and others, such as survivorship nurses, can play in providing and interpreting information along with supporting and empowering survivors to maximize their well-being. Culturally sensitive navigation services are particularly important for AYA survivors from historically underserved groups because of the many challenges they face when diagnosed at this point in their lives.
When first diagnosed with breast cancer, women must make consequential decisions usually in a short time period. Research has identified that stress negatively impacts cognitive functioning, including information processing and decision-making, and this has implications for the life changes (eg, fertility preservation) many women are facing when under significant stress at the time of diagnosis. We are asking women to make life-changing decisions when they may be least able to process the information they need to make informed choices. All who provide care and support to newly diagnosed AYA BC patients must understand how to support people to make important decisions under difficult circumstances.16
An underlying theme was the need for providers to think beyond medical diagnosis and treatment and communicate information about symptom management, signs of recurrence or metastasis, fertility preservation, and complementary therapies. Future research should address best practices for teaching providers how to guide BC patients through the decision-making process, assess for distress, and promptly refer their patients for psychosocial intervention for managing stress and related symptoms.
Limitations
This study had limitations. Data were collected from those who had received services from or worked with BCRC in the past. Their perspectives may not reflect the experience of those without a connection to services such as those provided by BCRC (eg, patient navigation), or those whose contact may not have been as positive as these participants described. The focus group moderator and assistant moderator are both non-Hispanic white women, and the racial/ethnic difference between them and many focus group participants may have limited some of the issues that were raised in these groups. Although the assistant moderator was a grants specialist who does not provide navigation services, her connection to BCRC may have affected women’s comments. Focus group participants were highly educated, and most had private insurance, so they may not be reflecting concerns of women who lack these resources. Although many attempts were made to include women living in rural areas, no one in the focus groups lived farther than 30 miles away from a major metropolitan area.
The number of participants in focus groups and particularly in the key informant interviews was small, did not include younger AYAs, and did not include oncologists (despite repeated attempts to encourage their participation). Future needs assessment studies should include more diverse groups of participants and key informant interviewees who represent a wider range of professional roles.
Conclusion
This study points to the key role both patient and nurse navigators can play in providing sustained support that is tailored to AYA survivors. Although addressing the financial tsunami created by a cancer diagnosis is difficult, these findings highlight the importance of continued advocacy and public education to raise awareness that having a basic level of insurance does not eliminate financial burdens for survivors. Navigators and other providers are encouraged to collaborate with partners in their communities to decrease burdens on AYA survivors, particularly women with mBC who face long-term expenses. Evidence-based strategies to improve access to culturally sensitive care and enhance patient/provider communication must also be implemented.
Acknowledgments
The Breast Cancer Resource Center is supported by the Grant or Cooperative Agreement Number NU58DP006675-01-00, funded by the Centers for Disease Control and Prevention. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the Centers for Disease Control and Prevention or the Department of Health and Human Services. The authors wish to thank the project’s Advisory Council for their help.
Emily Croce is supported by the National Institute of Nursing Research of the National Institutes of Health (T32NR019035). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
References
- Miller KD, Fidler-Benaoudia M, Keegan TH, et al. Cancer statistics for adolescents and young adults, 2020. CA Cancer J Clin. 2020;70:443-459.
- Martin S, Ulrich C, Munsell M, et al. Delays in cancer diagnosis in underinsured young adults and older adolescents. Oncologist. 2007;12:816-824.
- Nolan VG, Krull KR, Gurney JG, et al. Predictors of future health-related quality of life in survivors of adolescent cancer. Pediatr Blood Cancer. 2014;61:1891-1894.
- D’Agostino NM, Penney A, Zebrack B. Providing developmentally appropriate psychosocial care to adolescent and young adult cancer survivors. Cancer. 2011;117(10 suppl):2329-2334.
- Arora RS, Alston RD, Eden TOB, et al. Comparative incidence patterns and trends of gonadal and extragonadal germ cell tumors in England, 1979 to 2003. Cancer. 2012;118:4290-4297.
- Siembida E, Loomans-Kropp HA, Trivedi N, et al. Racial disparities in adolescent and young adult cancer clinical trial enrollment. J Clin Oncol. 2020;38(suppl). Abstract 91.
- Guy GP Jr, Yabroff KR, Ekwueme DU, et al. Estimating the health and economic burden of cancer among those diagnosed as adolescents and young adults. Health Aff (Millwood). 2014;33:1024-1031.
- Kale HP, Carroll NV. Self-reported financial burden of cancer care and its effect on physical and mental health-related quality of life among US cancer survivors. Cancer. 2016;122:283-289.
- Smith AW, Parsons HM, Kent EE, et al. Unmet support service needs and health-related quality of life among adolescents and young adults with cancer: the AYA HOPE study. Front Oncol. 2013;3:75.
- Kirchhoff AC, Lyles CR, Fluchel M, et al. Limitations in health care access and utilization among long-term survivors of adolescent and young adult cancer. Cancer. 2012;118:5964-5972.
- Jagsi R, Pottow JAE, Griffith KA, et al. Long-term financial burden of breast cancer: experiences of a diverse cohort of survivors identified through population-based registries. J Clin Oncol. 2014;32:1269-1276.
- Pisu M, Kenzik KM, Oster RA, et al. Economic hardship of minority and non-minority cancer survivors 1 year after diagnosis: another long-term effect of cancer? Cancer. 2015;121:1257-1264.
- Kidd PS, Parshall MB. Getting the focus and the group: enhancing analytical rigor in focus group research. Qual Health Res. 2000;10:293-308.
- Miles MB, Huberman AM. Qualitative Data Analaysis. 2nd ed. Thousand Oaks, CA: Sage Publications; 1994.
- Gould J, Grassau P, Manthorne J, et al. ‘Nothing fit me’: nationwide consultations with young women with breast cancer. Health Expect. 2006;9:158-173.
- Sun CSJ. Shared decision-making about breast reconstruction: a decision analysis approach. Dissertation. The University of Texas at Austin; 2013. https://repositories.lib.utexas.edu/handle/2152/22976.