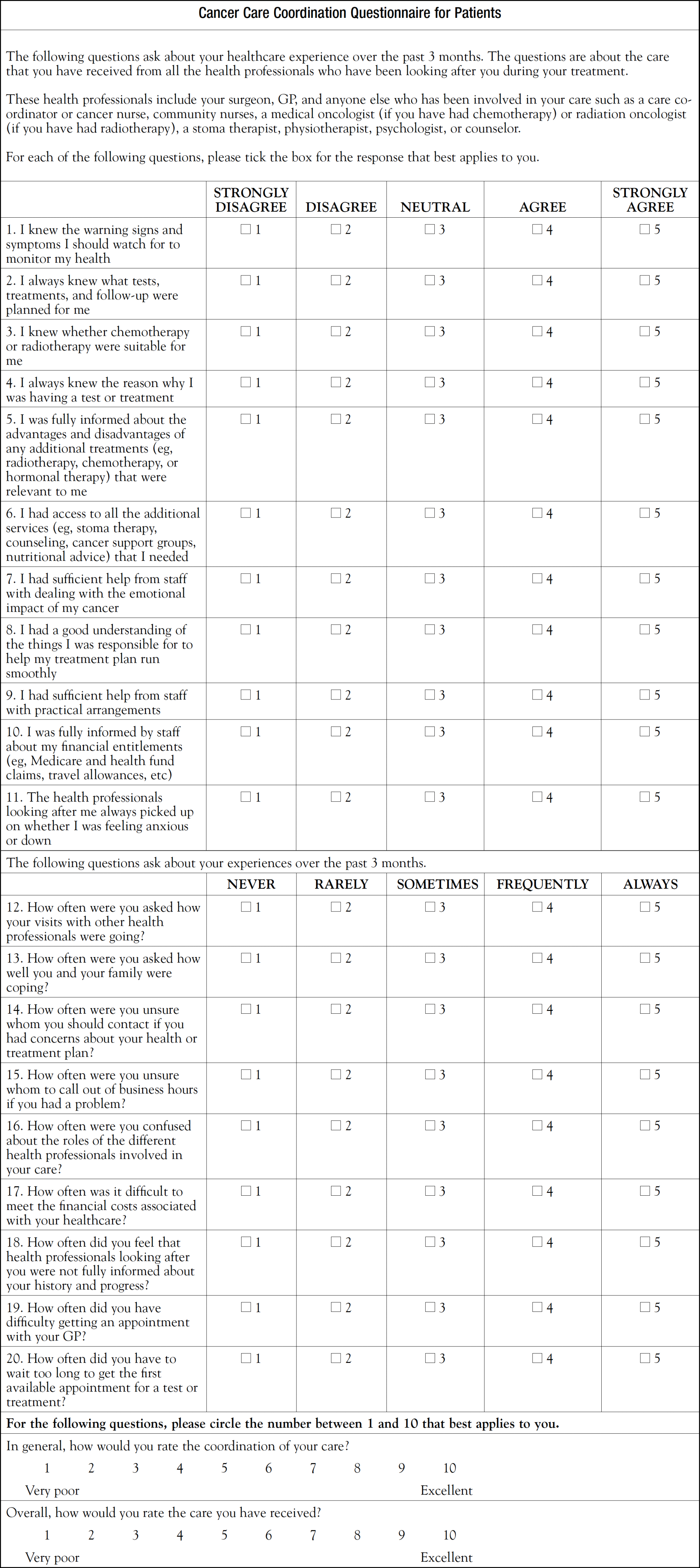
The leadership in oncology administration and the patient experience department at a community hospital identified coordination of care as an area for improvement for patients with brain cancer. The standard of care for these patients is concurrent radiation therapy and oral chemotherapy. The team members were effective at managing their own part of the care, but one dedicated team member was not ultimately responsible for coordinating care between the modality teams. The hospital’s patient navigator (lay, OPN-CG) was recruited to work with the neurology team to ensure coordination of care for this vulnerable population. The navigator interviewed individual staff members on the team to better understand existing patient flow and processes. With this view of the gaps in the processes, the patient navigator developed some tools to help educate patients and caregivers and to better guide the care team in managing patient flow. To evaluate the care coordination process, the patient navigator also identified a validated tool from the Sydney School of Public Health, Sydney Medical School, University of Sydney, NSW, Australia, to measure patient perception about care coordination (click here).1 This is now being administered midtreatment to address current patient issues. These data will also be used to design program improvements for future patients. The navigator and her supervisor will share the new best practices with other disease groups in the hospital for adaptation with their patient populations. The navigator will submit an abstract for a professional conference to demonstrate the role that a patient navigator can play in the operations of a clinic, care coordination, and patient satisfaction.
AZ is a 65-year-old male who was experiencing headaches, and ultimately a seizure, and went to the local emergency department. Brain imaging discovered a lesion suspicious of cancer. AZ underwent brain surgery, and the pathology resulted in a diagnosis of a World Health Organization grade 4 glioblastoma (GBM).
While recovering from the surgery, AZ scheduled an appointment with a medical oncologist who specializes in brain cancer. The patient navigator, who prepares a weekly report of new neurology patient consultation appointments from the electronic medical records system, saw that AZ was on the schedule. After reviewing his chart and having a discussion with the medical oncologist and the radiation oncologist, it was determined that a double consultation would help with the coordination of AZ’s likely care. The neurology clinic aims to start adjuvant therapy approximately 30 days from surgery.
Although there is a doubling time of 24 days for GBM, retrospective studies suggest that there is a clinical benefit associated with a short delay in the initiation of concurrent chemoradiation after surgery for GBM patients.2 The patient navigator plays an important role in ensuring timely provider consults and initiation of adjuvant therapy, as well as alleviating patient anxiety related to knowledge about next steps in his/her care plan.
The patient navigator attended the medical oncology consultation and provided the patient and his wife with a patient guide that she had compiled. This guide listed names and contact information for all members of the team, including medical oncology, radiation oncology, triage nurse, administrative schedulers, patient navigator, palliative care nurse practitioner, dietitian, social worker, rehabilitation/speech therapy, vision specialists, brain cancer and caregiver support groups, and brain cancer advocacy groups. Having staff names and contact information provide patients and their caregivers the ability to contact the appropriate person with questions or concerns or to schedule appointments with various departments. Patients and caregivers are also aware that the patient navigator is available to assist with scheduling or other coordination needed. In addition, the patient navigator refers all neurology patients to the social worker and to the palliative care nurse practitioner, who introduce themselves to the patient to offer their services.
During the initial appointment, the patient navigator learned that AZ and his wife had differences of opinion about employing a home health aide. The wife wanted to bring someone in so that she could get some time to go to the gym, while ensuring that AZ had someone available to help him if needed. AZ didn’t feel that this was necessary. The patient navigator referred the couple to the social worker for either individual counseling or family counseling to talk about how to acknowledge and satisfy both of their needs. At the consultation AZ was also referred to rehabilitation to manage some gait issues caused by the tumor and surgery, and the patient navigator facilitated scheduling rehabilitation appointments to coordinate with other planned visits to the hospital.
The patient navigator updated the team’s Excel spreadsheet (click here) with AZ’s information and distributed it to the rest of team for discussion at the weekly rounds. During these rounds, new, in-treatment, follow-up, and hospice patients were discussed. Immediately after the rounds, the patient navigator and the medical oncologist used the data elements on the tracking sheet to enter orders for medications, chemotherapy education session, labs, MRI, and follow-up appointments. At AZ’s radiation simulation, the administrative assistant used a scheduling checklist created by the patient navigator to schedule weekly labs, the chemotherapy education session, and a transition visit with the medical oncologist. These tools and processes were put in place to ensure that every patient’s care is carefully planned, and no step is overlooked.
Once the treatment start date was set by the radiation oncologist, the patient navigator coordinated with the medical oncologist and the pharmacists to ensure that the specialty medication would be delivered to the patient on time. AZ’s insurance authorized the specialty medication, but because a confirmation on the dose was needed, the medication delivery date was delayed a day. The patient navigator notified the entire team, most importantly the radiation team, who had to adjust AZ’s radiation treatment start date to align with day 1 of the chemotherapy treatment.
The day prior to treatment start, the patient navigator contacted AZ to ensure that he had his medications and that he understood the timing for the antiemetic, the antibiotic, and the oral chemotherapy relative to the radiation treatment schedule. AZ had a question about whether he should take the medication with/without food, so the patient navigator conferred with the primary medical oncology nurse for an answer and got back to AZ.
During the third of the 6 weeks of chemoradiation treatment, the patient navigator met with the patient to administer the questionnaire. During this visit, AZ indicated that he had some questions about the extent of the surgery he had and the implications that this may have for his eligibility for clinical trials in the future. The patient navigator e-mailed the physicians involved in AZ’s care and asked that they address this at the next treatment visit.
Conclusion
Patient navigators are increasingly being used to support the clinical team and have a role in timeliness of care, care coordination, addressing patient barriers, program evaluation, and process improvement. With the recent creation of patient navigation accreditation through AONN+, the required competencies for patient navigation have been more clearly defined and evaluated. In the area of professional development, patient navigators need organizational skills, office skills, interpersonal skills, as well as skills in time management, problem solving, and critical thinking. Various opportunities exist to develop those skills through AONN+, the Cancer Patient Education Network, and the Institute for Patient-Centered Initiatives and Health Equity at the GW Cancer Center. Patient navigators are required to understand their scope of practice and have opportunities to expand their role through professional development, collaborating with clinical team, utilizing critical thinking, participating in online and in-person training, networking with other patient navigators, and maximizing on memberships in AONN+ or other professional organizations.
References
- Young JM, Walsh J, Butow PN, et al. Measuring cancer care coordination: development and validation of a questionnaire for patients. BMC Cancer. 2011;11:298.
- Han SJ, Englot DJ, Birk H, et al. Impact of timing of concurrent chemoradiation for newly diagnosed glioblastoma: a critical review of current evidence. Neurosurgery. 2015;62(suppl 1):160-165.
Resources
- Navigation tracking sheet for patient navigator and for weekly rounds (http://www.jons-online.com/wp-content/uploads/2017/06/JONS-EIP38-39p.pdf)
- Patient flow chart (http://www.jons-online.com/wp-content/uploads/2017/06/JONS_June17aPatFlow.pdf)
- Patient evaluation of care coordination (http://www.jons-online.com/wp-content/uploads/2017/06/JONS_June17-PDF1.pdf)
- Academy of Oncology of Nurse & Patient Navigators: www.aonnonline.org/career-center/aonn-navi gation-certification/
- American Cancer Society. www.cancer.org/latest-news/navigators-help-cancer-patients-manage-their-care.html
- Cancer Patient Education Network. www.cancer patienteducation.org/
- Harold P. Freeman Patient Navigation Institute. www.hpfreemanpni.org
- Institute for Patient-Centered Initiatives and Health Equity at the GW Cancer Center. https://smhs.gwu.edu/gwci
The authors can be contacted as follows:
Eugenia Artice, RN-BC, BSN
WVU Cancer Institute
This email address is being protected from spambots. You need JavaScript enabled to view it.
Pam Goetz, BA, OPN-GC
Sibley Memorial Hospital, Johns Hopkins Medicine
This email address is being protected from spambots. You need JavaScript enabled to view it.
Barbara McHale, RN, BS, ONN-CG, OCN, CBCN
Retired, Hildegard Medicus Cancer Center
This email address is being protected from spambots. You need JavaScript enabled to view it.
Marian E. Gilmore, RN, OCN, ONN-CG
Dana-Farber/Brigham & Women’s Cancer Center
This email address is being protected from spambots. You need JavaScript enabled to view it.