Background: Patients newly diagnosed with breast cancer face overwhelming distress and fear, often due to a deficit of knowledge about the disease and expectations regarding a cancer diagnosis. Research shows that in times of other types of illness and exigency, home visits by a nurse have improved health and wellness; expedited progressive patient outcomes; and increased comfort and decreased anxiety, fear, and distress related to the situation, as shown in the literature review. Patients receiving a new diagnosis of breast cancer may also benefit from the support, education, and reassurance provided by a registered nurse navigator during a home visit to the clients.
Purpose: The purpose of this study was to examine and assess the effect of a nurse navigator home visit to reduce distress among women who have been newly diagnosed with breast cancer. It was hypothesized that the amount of distress experienced would be less following the nurse navigator visit providing support and education than the amount experienced at the initiation of the visit.
Methods: A total of 31 patients with newly diagnosed breast cancer from a hospital-based breast health center participated in the study. Participants self-reported ratings of their distress levels before and after a home visit intervention that included education, support, and navigation by a registered nurse navigator.
Results: There was a significant reduction of distress levels as reported by participants (P = .001) from preintervention to postintervention.
Conclusion: The findings suggest significantly decreased levels of distress in newly diagnosed breast cancer patients after receiving a home visit intervention including individualized education, support, and navigation.
Excluding skin cancers, breast cancer is the most common type of cancer diagnosed in women in the United States. According to the American Cancer Society (ACS)1 and the National Cancer Institute (NCI),2 more than 2.8 million women in the United States have a history of breast cancer. These increasing numbers include women who are currently undergoing treatment and those who have completed it. According to the ACS,1 an estimated number of more than 200,000 women were diagnosed with invasive breast cancer in 2015 in the United States, and over 1 million new cases were diagnosed worldwide. For noninvasive ductal carcinoma in situ, 60,290 new cases were projected for 2015.
Affecting 1 in 8 women (12.5%) in the United States,1 a breast cancer diagnosis has the power to reduce strong, confident women to those experiencing physical and psychological effects, including apprehension, panic, distress, and fear. This year, it is expected that 40,290 women will die of breast cancer. The number of deaths is approximately 26.6 per 100,000 women per year.2 It is the third leading cause of death in the United States in women behind lung cancer and heart disease, according to the National Breast Cancer Coalition3 and the ACS.1 NCI figures show the median age at death from breast cancer is 68 years, with the highest percentage of deaths occurring between the ages of 55 and 64 years.2
Problem Statement
A gap exists between the time a patient receives a new breast cancer diagnosis and the time and ability it takes to assimilate the diagnosis. Within this gap is typically fear, anxiety, and distress related to the new cancer diagnosis. As part of a randomized controlled trial, researchers sent a survey to breast cancer survivors 7 years after the research trial was completed to examine recollections of the breast cancer experience. The most prominent experience, more even than chemotherapy treatment, was psychological distress.4 Fear, distress, and anxiety may negatively affect breast cancer patient outcomes. Yeh et al5 found in several studies that patients with breast cancer were affected by severe anxiety (38.4%) and depression (22%) manifested by fatigue, sleep disturbance, and lowered quality of life, affecting recovery and long-term survival. Newly diagnosed patients experience many fears. These include fear of recurrence; death; loss of hair; telling their families, work colleagues, and managers; and financial fears related to the inability to work. Some experience language and cultural barriers, and others experience household disruptions. Ullman et al6 found that patients and their family members may experience both physical and psychological disorders that impair recovery for the patient.
Fear of recurrence in patients diagnosed with either invasive or noninvasive forms of breast cancer has been found to lead to decreased quality of life. In a study conducted by Sanders et al,7 anxiety levels were shown to vary only slightly between these 2 groups; however, the margin of mortality varies between these 2 types of diagnoses. The risk of dying of invasive breast cancer in 10 years is 11.5% compared with 2% found with noninvasive breast cancer. According to the ACS,1 in women with early breast cancer (classified as either noninvasive or invasive identified as <2 cm), recurrence risk is higher within 5 years of the first diagnosis. Seven percent to 11% of women with early breast cancer may have a local recurrence; however, that risk varies individually. The perception of recurrence is often overestimated, resulting in higher levels of anxiety and decreased quality-of-life outcomes. Other responses affecting quality of life from fear and anxiety include maladaptive coping, such as frequent body checking or worrying.8 Other women, due to possible distress, knowledge deficit, or distrust of the medical system, refuse traditional standard treatment regimens and look for alternative therapies or quick fixes that have not been shown to be effective.9
Purpose of the Project
The purpose of this study was to examine the effect of a nurse navigator home visit to reduce distress in newly diagnosed breast cancer patients, incorporating support and education that included resources and gift items. The hypothesis was that the nurse navigator home visit would result in decreased distress levels from initiation to end of the visit. The clinical question addressed by the study was: In newly diagnosed breast cancer patients, does a home visit intervention by a nurse navigator help to decrease distress and fear related to the breast cancer diagnosis within the first week following diagnosis?
Background/Rationale
Utilization of a nurse navigator home visit shortly after receiving a breast cancer diagnosis may make a difference in how diligently the patient progresses on the breast cancer treatment continuum, by decreasing levels of fear and distress. Findings from a year-long study show the feasibility of providing home visits in rural communities to patients with life-limiting disease.10 These visits have improved quality of life, smoothed transitions during disease processes, and fostered the patient/family-centered approach. One purpose for a nurse navigator home visit is to assess for barriers to care, such as those that might hamper a safe home environment in which to recover, “facilitating healthy behaviors,” and providing “innovative care for its home-based intervention venue” for the nurse navigator to assist with positive outcomes.11 Another study, looking at the effects of an advanced practice nurse in-home visit for elderly adults, concluded that principles of empowerment, partnership, family, and health promotion were effective in reducing adverse health outcomes such as anxiety, depression, and falls.12 The Agency for Healthcare Research and Quality estimates that the direct costs for cancer in the United States in 2014 were over $87.8 billion.13 Other sources state that each breast cancer patient’s treatment will be $20,000 to $100,000, depending on need. Most breast cancers cost patients or other financial sources $2100 to $5000 per month during the months of treatment.14 Much of the education and support found in the facility setting could be provided in the comfort and familiarity of the home and may lead to cost savings through improved outcomes. Home visits may be included in nurse navigation services within facility billing; some coding is available. Nurse navigation and coordination of care were part of the Patient Protection and Affordable Care Act that was signed into law in 2012.
Literature Review
A literature review of full-text, peer-reviewed articles on patient perspectives of nurse navigation intervention was conducted. Three key findings were discovered that helped delineate this project and support the need for early intervention after a diagnosis of breast cancer to reduce distress, fear, and anxiety: (1) the need for early intervention to help decrease distress, (2) include nurse navigation as part of standard care for cancer, and (3) a potential for home visits by the nurse navigator to bring comfort and decrease distress or fear. A small sample of the literature reviewed follows.
Early intervention appears to help reduce fear and anxiety, as well as assist patients to better adjust to life-altering illness. A study completed by Lee et al15 measured distress in patients with newly diagnosed breast cancer and found that 30% to 75% have distress particularly at the onset, and that around 33% of those have poor psychosocial responses and associated quality-of-life outcomes. Chirico et al16 performed a cross-sectional study of distress indicators in 130 newly diagnosed breast cancer patients over 4 months and found that most patients receiving early interventions did have slightly decreased levels of anxiety and adjusted to illness more effectively.
Results from a 2014 study exploring the patient navigator role and perspectives of young women diagnosed with breast cancer showed that there continue to be gaps in transitions of care. The patients continue to need increasing emotional support, education, and navigation early in diagnosis, with tailored interventions leading to favorable outcomes.17 Face-to-face nurse navigation as part of standard early care appears to be beneficial to patients with a new breast cancer diagnosis. In one longitudinal, phenomenological-hermeneutical study, patients were offered the use of a nurse navigator throughout the entire cancer trajectory. Five were followed over 2 years. All reported feelings of self-actualization and decreased anxiety.18
A randomized controlled trial tested the effectiveness of nurse navigators to enhance the usual cancer care of 251 patients over 16 weeks. Patients reported satisfaction and feeling supported psychologically and clinically.19 Another randomized controlled trial was performed to examine the impact of patient nurse navigation in Northwest tribal communities on cancer diagnostic resolution with 1236 participants over 4 years. Patients receiving the intervention of a navigator received faster diagnostic resolution, with the outcome that the navigator could have significant impact on patient outcomes after barriers to care are removed.20 In a systematic review examining the effect of nurse navigators on patient outcomes,21 studies looked mostly at the needs of populations and measured issues such as timeliness of care, screening levels, and levels of distress. Generally, those who used a navigator experienced positive outcomes, particularly in the identification of barriers to care.
The use of home visits for newly diagnosed patients with breast cancer is not well documented; however, the benefit of using home visits by nurses for other disease processes and conditions, including reduction of anxiety, fear, and distress, has been documented for years. A multiperspective qualitative study looked at the effectiveness of visiting nurses with patients receiving palliative care.22 Trust relationships were built in the home, and patients appreciated the informal style as very complex care events took place. The study showed that for clinical practice implications, home visits were a welcome provision of care and helped the patient to communicate more openly in a familiar environment.22 Sahlen et al23 found tremendous cost-effectiveness, care improvements, and improved distress outcomes with home visits. Patients have verbalized feeling so supported when a nurse navigator came to the home and provided human contact, thus one of the reasons to visit the home and not just have a telephone conversation. A nurse navigator home visit may help to reduce fear and distress in a comfortable and empowered environment for a newly diagnosed patient with breast cancer.
Project Objectives
The specific objectives were: (1) to implement a nurse navigator home visit to provide support and education to newly diagnosed breast cancer patients; (2) to examine the impact of this visit on self-reported distress due to fear and anxiety surrounding a new breast cancer diagnosis following support and education provided with a nurse navigator visit; and (3) to increase patient satisfaction as evidenced by responses on a patient satisfaction survey. This project seeks to provide meaningful data to contribute to the body of knowledge that supports the utilization of nurse navigator home visits for patients newly diagnosed with breast cancer, and how this nursing intervention can decrease distress in newly diagnosed patients. Note that the visit was made for support shortly after diagnosis (3-4 days) and is made before the patient sees the breast surgeon or oncologist, which typically happens approximately 1 week after diagnosis.
Theoretical Framework
The framework for this project is based on Jean Watson’s Caring Theory,24 in which the following concepts, describing navigator purposes, were used to facilitate the nurse navigator home visit to decrease distress:
- A relational caring for self and others
- Transpersonal caring relationships: heart-centered, authentic presence
- Caring occasion/caring moment: appropriate for home visit
- Multiple ways of knowing (includes cultural competence, also appropriate with visit)
- Reflective, meditative approach
- Caring changes self, others, and culture (decreasing distress in the new normal)
Jean Watson developed her science and theory with an eye to the community and holistic health practices while at the same time recognizing the needs of the individual and his/her need to give and experience caring for oneself and others. The use of this theory for new breast cancer patients is helpful and applicable to the situation as they transition into a new normal and feel cared for at each step of the process from diagnosis through treatment and survivorship. The navigator visit to the home encompasses all the concepts of this theory and helps ease the patient into what will become the new way of life.
Project Design
This study is a descriptive-exploratory study to assess the effect of the nurse navigator home visit intervention on reduction of distress among patients with a new breast cancer diagnosis following a breast biopsy. A paired t test was conducted to compare pretest and posttest levels of self-reported distress using the National Comprehensive Cancer Network (NCCN) Distress Thermometer and Questionnaire. Patient satisfaction surveys were also captured to evaluate patient satisfaction with the nurse navigator home visit.
Human Subjects Protection
The study was approved by both the medical center and university Human Subjects Protection committees. No personally identifiable data were captured for the study. The nurse navigator home visit intervention was a voluntary program in which individuals could decline at any time to participate, with no questions asked. The study was self-funded with no cost to the participant. Patients who declined to participate in the study still received nurse navigation services, including a home visit if it was desired, to ensure the care continuum met their needs.
Instruments
The NCCN Distress Thermometer and Questionnaire is frequently used in oncology to assess levels of distress, fear, and anxiety.25 The tool does not require permission to use in patient care; however, permission was obtained to use the tool for this project. To complete the tool, the participant circles the number corresponding to the level of distress perceived. Responses on the Distress Thermometer range from 0 (no distress) to 10 (extreme distress). The other boxes on the form indicate categories in which the patient may feel distress; this part of the tool is for possible referrals for additional assistance but was not measured for this project. Those categories include practical problems, family problems, emotional problems, spiritual/religious concerns, and physical problems. This valid instrument has been used in numerous studies, with a Cronbach alpha of 0.88. Research has supported its internal consistency and reliability.
The participant/patient satisfaction survey was a simple survey designed by the nurse navigator. It asked participants to rate their satisfaction with the home visit. There were 5 questions on the survey: (1) How helpful was the nurse visit? (2) How helpful were the materials? (3) Why or why not did you feel the visit to be helpful to you? (4) What can we do to improve the nurse navigator home visit? (5) What might we do to improve the resource materials? The first 2 questions provided a number to circle from 1 to 4, from not helpful at all to extremely helpful. There was room for comments. Participants were provided an addressed, stamped envelope at the time of the home visit and requested to mail the satisfaction survey back within 2 days.
Recruitment Methods
A convenience sample of patients with newly diagnosed breast cancer was recruited from the breast health center of a regional medical center in North Carolina. Participants were chosen from a population of patients undergoing breast biopsy following an abnormal mammogram. Inclusion criteria were met by patients undergoing stereotactic or ultrasound-guided core biopsies that resulted in a breast cancer diagnosis. The number of participants was determined based on the number of biopsies performed each week, the average number of cancer diagnoses per week, and time constraints of the researcher. A priori power analysis was not conducted.
Participants were invited to be part of the study while still in the preparatory stages for the biopsy and signed a written informed consent form provided by the hospital cancer center. Participants chose a method to receive their biopsy results—phone call or meeting. Each chose a telephone call from the nurse navigator to discuss biopsy results 2 or 3 days after the biopsy. Following the call, arrangements were made to provide a home visit intervention on the participant’s choice of day and time, and within 3 to 4 days of receiving biopsy results unless specified otherwise by the patient.
Home Visit Intervention
The home visit intervention was conducted by the nurse navigator in the homes of the newly diagnosed patients. Mostly, visits took place in living rooms, sitting side by side where hands could be held and hugs exchanged when needed. Some were at kitchen tables. Some visits included the participant’s family sitting with her or gathered around the room. The goal was to create an atmosphere of calm, comfort, and familiarity to empower the patient while having informative and supportive conversations related to her new cancer diagnosis and process of care.
The home visit intervention did not have a predetermined length of time. Time spent with the patient and/or family was based on the needs, questions, and expressions of the participant. Most were approximately 1 hour; times ranged from 45 minutes to 2 hours. Prior to the intervention of support and education provided by the nurse navigator during the home visit, the participant completed the NCCN Distress Thermometer and Questionnaire.25 The tool was explained to the participant by the nurse navigator during the home visit. The intervention began with time for the participant to express thoughts, feelings, and questions. A cancer care package was then presented with accompanying education, including a breast cancer handbook, complete with pictures to help educate, and other pertinent information. Discussion time was provided about the process of care, package contents, pathology of the disease, and for the nurse navigator to respond to any other concerns expressed by the patient. A packet of resources was provided along with a pillow made by the Girl Scouts and other volunteers, and a piano CD made by the researchers. These resources and gifts are provided to all patients diagnosed at the breast health center. Following the intervention, the participant completed the distress screening tool again. If needed, time was again provided for the participant to express feelings, thoughts, and questions regarding the new breast cancer diagnosis and related issues. All package materials, previously approved by the hospital system and cancer center, were free of cost to participants. The visit for this study was made only once; however, the participant was informed that she could have other visits if needed or desired for support and education.
Results
Sample
The sample (N = 31) consisted of all female patients, ranging in age from 32 to 71 years. They were from a diverse cultural population: 19 were Caucasian; 6, African American; 2, Hispanic; 1, Asian; and 3 who declined to designate ethnic origin; 7 different religious preferences were listed. The power analysis indicated a sufficient sample size for this analysis and resulted in a calculated power of .77, with a moderate effect size (.5).26 The visits ranged in time from 45 minutes to 2 hours, depending on patient need. Travel time, for estimate of nurse cost, varied from 10 minutes to 1.1 hours one way.
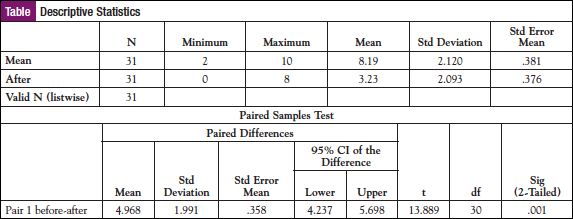
The mean pretest score on the NCCN Distress Thermometer and Questionnaire was 8.19 (SD = 2.120), indicating high levels of distress. The mean score on the posttest was 3.23 (SD = 2.093). The differences between pretest and posttest scores were found to be significant (t = 13.889, P = .001) (Table).
Eleven participant satisfaction surveys were returned, resulting in a 35% response rate, which is an acceptable response rate for a mail-back survey.
Discussion
The nurse navigator home visit intervention had a significant positive effect on reducing the levels of distress in this sample of patients with newly diagnosed breast cancer. The hypothesis that newly diagnosed breast cancer patients would benefit by having a nurse navigator home visit to decrease levels of distress was supported by the findings in this study. The home visit intervention helped these patients to lower their distress levels and feel comfortable in their homes asking questions and learning about their disease process.
The nurse navigator home visit intervention also resulted in high patient satisfaction. All surveys returned included patient comments, in a space at the bottom in which to write comments, such as “I still cannot believe you were willing to come out to my home and sit with me and talk to me.” Others were “It meant so much to me that you came to the house and met my family and taught us about breast cancer,” and “You made this whole thing so personal and so much better when you visited. I felt prepared to meet the doctor and go on.” In one visit, the patient’s physician was very interested in the visit and accompanied the navigator to the home. The patient stated feeling so supported and loved when she saw both standing on her porch. Comments made by participants in their homes and on returned surveys indicate satisfaction and intent to return to the breast health center, thereby indicating salience and business stability.
The findings from this study indicate that the use of a nurse navigator home visit can successfully decrease distress levels of patients with a new cancer diagnosis. This study has a number of limitations, including use of a convenience sample. Future studies with a larger sample size and a higher diversity of the patient population accounting for various social determinants are needed. Other factors to be explored in future studies include presence or absence of family/social support on distress levels, use of telephonic or home visit interventions, and cost-benefit analysis of nurse home visit interventions. Longitudinal cohort studies to examine the nurse navigator home visit on long-term patient outcomes are also needed.
Summary
The results from this pilot study provide support that nurse navigation home visit interventions are effective for reducing distress in patients with newly diagnosed breast cancer. As the literature suggested, distress is associated with negative patient outcomes, so it is vital for nurse navigators to be encouraged to talk with their patients and explore possibilities for incorporating home visits in their practice to promote positive patient outcomes.
References
- American Cancer Society. Breast Cancer. www.cancer.org/cancer/breast-cancer.html. 2015.
- National Cancer Institute. Surveillance, Epidemiology, and End Results program. http://seer.cancer.gov/statfacts/html/breast.html. 2015.
- National Breast Cancer Coalition. The Breast Cancer Deadline. http://breastcancerdeadline2020.org/breast-cancer-information/31-truths/truth-8.html. 2015.
- Lindberg P, Koller M, Steinger B, et al. Breast cancer survivors’ recollection of their illness and therapy seven years after enrollment into a randomized controlled clinical trial. BMC Cancer. 2015;15:554.
- Yeh M, Chung Y, Hsu MY, et al. Quantifying psychological distress among cancer patients in interventions and scales: a systematic review. Curr Pain Headache Rep. 2014;18:399.
- Ullman AJ, Aitken LM, Rattray J, et al. Intensive care diaries to promote recovery for patients and families after critical illness: a Cochrane Systematic Review. Int J Nurs Stud. 2015;52:1243-1253.
- Sanders JB, Loftin A, Seda J, et al. Psychosocial distress affecting patients with ductal carcinoma in situ compared to patients with early invasive breast cancer. Clin J Oncol Nurs. 2014;18:684-688.
- Lebel S, Maheu C, Lefebvre M, et al. Addressing fear of cancer recurrence among women with cancer: a feasibility and preliminary outcome study. J Cancer Surviv. 2014;8:485-496.
- Citrin DL, Bloom DL, Grutsch JF, et al. Beliefs and perceptions of women with newly diagnosed breast cancer who refused conventional treatment in favor of alternative therapies. Oncologist. 2012;17:607-612.
- Pesut B, Hooper BP, Robinson CA, et al. Feasibility of a rural palliative support service. Rural Remote Health. 2015;15:3116.
- Yun L, Boles RE, Haemer MA, et al. A randomized, home-based, childhood obesity intervention delivered by patient navigators. BMC Public Health. 2015;15:506.
- Imhof L, Naef R, Wallhagen MI, et al. Effects of an advanced practice nurse in-home health consultation program for community-dwelling persons aged 80 and older. J Am Geriatr Soc. 2012;60:2223-2231.
- American Cancer Society. Economic Impact of Cancer. www.cancer.org/cancer/cancer-basics/economic-impact-of-cancer.html. 2015.
- Jerusalem G, Neven P, Marinsek N, et al. Patterns of resource utilization and cost for postmenopausal women with hormone-receptor-positive, human epidermal growth factor receptor-2-negative advanced breast cancer in Europe. BMC Cancer. 2015;15:787.
- Lee TY, Chen HH, Yeh ML, et al. Measuring reliability and validity of a newly developed stress instrument: Newly Diagnosed Breast Cancer Stress Scale. J Clin Nurs. 2013;22:2417-2425.
- Chirico A, Lucidi F, Mallia L, et al. Indicators of distress in newly diagnosed breast cancer patients. PeerJ. 2015;3:e1107.
- Pedersen AE, Hack TF, McClement SE, et al. An exploration of the patient navigator role: perspectives of younger women with breast cancer. Oncol Nurs Forum. 2014;41:77-88.
- Thygesen MK, Pederson BD, Kragstrup J, et al. Benefits and challenges perceived by patients with cancer when offered a nurse navigator. Int J Integr Care. 2011;11:1-12.
- Horner K, Ludman EJ, McCorkle R, et al. An oncology nurse navigator program designed to eliminate gaps in early cancer care. Clin J Oncol Nurs. 2013;17:43-48.
- Warren-Mears V, Dankovchik J, Patil M, et al. Impact of patient navigation on cancer diagnostic resolution among northwest tribal communities. J Cancer Educ. 2012;28:109-118.
- McVay S. The effect of different types of navigators on patient outcomes. Journal of Oncology Navigation & Survivorship. 2014;5(2):17-24.
- Griffiths J, Ewing G, Rogers M. Early support visits by district nurses to cancer patients at home: a multi-perspective qualitative study. Palliat Med. 2012;27:349-357.
- Sahlen KG, Boman K, Brannström M. A cost-effectiveness study of person-centered integrated heart failure and palliative home care: based on a randomized controlled trial. Palliat Med. 2016;30:296-302.
- Watson J. Core concepts of Jean Watson’s theory of human caring/caring science. Watson Caring Science Institute. 2010;1-7.
- National Comprehensive Cancer Network. NCCN Distress Thermometer and Problem List for Patients. www.nccn.org/patients/resources/life_with_cancer/pdf/nccn_distress_thermometer.pdf. 2016.
- Biderman MD. Power tables. www.utc.edu/faculty/michael-biderman/pdfs/powertables.pdf. 2014.




