To download this article as a PDF, see the link below.
AONN1546-3
Executive Summary
When a lung cancer diagnosis is made, the first thing that nearly every individual and their loved ones want are answers. What do I do next? How do I tell my children? Will I live? Making sure that newly diagnosed patients get the answers and information they need in a timely and consistent manner is the goal of the new initiative being spearheaded by the Academy of Oncology Nurse & Patient Navigators (AONN+). The diagnosis of cancer evokes a life-threatening reaction that can immediately hinder the quality of life (QOL) of individuals and their families. Anxiety and fear, common in the initial phase of cancer diagnosis and treatment, can be barriers to comprehension, coping, and self-care decisions. Receiving effective information regarding diagnosis and treatment during this stressful time is very beneficial in reducing anxiety, regaining a sense of control, and creating realistic expectations.1 When anxiety is lessened, coping is enhanced, and an individual’s needs are met during education, QOL is improved during the crucial period from diagnosis to treatment.
The objective of the Cancer Advocacy & Patient Education (CAPE) initiative is to create a web-based library of best-practice information that providers in the lung cancer space can give to their patients and caregivers at each point of interaction. The objectives are:
- To make the time between diagnosis and treatment as productive and meaningful as possible through interactivity and education to meet patients’ psychosocial needs
- To improve communication and shared decision-making around diagnosis, testing, and treatment between the patient, caregiver, and the cancer treatment team
- To ensure patient understanding of their diagnostic and treatment journey, individualized to their disease state
To develop this library, AONN+ partnered with Takeda Oncology and a multistakeholder coalition of leading patient advocacy organizations for lung cancer. A predetermined QOL model based on the domains of physical, psychological, social, and spiritual well-being was utilized to determine the needs of patients and their caregivers.2 A comprehensive search of the published literature in the past 10 years was conducted. A total of 1610 articles were screened, 205 full-text publications were reviewed, and 50 relevant articles were identified. Findings from the review and analysis of relevant articles, using the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) model, identified common areas of need/concern for patients with lung cancer and their caregivers.
Based on the identified areas of concern, 7 modules for the integrative education program were outlined, and current best-practice resources and tools were gathered for each module. The 7 modules addressing the physical, psychological, social, and spiritual well-being are: (1) Understanding Your Diagnosis, (2) Treatment & Clinical Trials, (3) Self-Care, (4) Coping, (5) Shared Decision-Making, (6) Financial, and (7) Caregiver & Family Role.
The CAPE program with its web-based platform through Health Unlocked3 will allow navigators and healthcare providers to deliver a personalized digital prescription to lung cancer patients and caregivers of cultivated, evidence-based, best of the best resources based on their physical, psychological, social, and spiritual well-being needs to make the time between diagnosis and treatment as productive and meaningful as possible.
By providing education, improving communication, shared decision-making, and ensuring patient understanding through interactivity and personalized resources of the CAPE program, navigators and healthcare providers can engage, inform, and empower newly diagnosed lung cancer patients, resulting in reduced distress and an improved patient experience. The education platform will assist the identification of interventions or tools to improve QOL throughout the disease process.
Introduction
Newly diagnosed cancer patients undergo numerous visits to doctors, imaging centers for scans, and laboratory testing prior to initiation of treatment. Waiting for test results can be challenging for physicians, patients, and caregivers, because there is a sense of urgency to start treatment. However, ensuring the correct diagnosis, staging, and optimal treatment plan is generally more relevant than initiating a timely but incorrect treatment plan.4 There are instances in which patient outcomes improve if treatment is expedited once all relevant tests are conducted and evaluated. In an era of personalized medicine, however, patients with actionable mutations derive greater survival benefit from targeted therapies as first-line treatment in addition to the advantage of better tolerability over chemotherapy.5,6 Non–small cell lung cancer (NSCLC) is one cancer for which molecular biomarker analysis must be done to determine therapeutic treatment choice. Yet, in one study, almost 20% of NSCLC patients started chemotherapy before biomarker results became available, although studies indicate that delaying treatment for several weeks while additional testing is being performed does not affect outcomes.7-9 As noted by Maigi and colleagues, “efforts to improve timeliness should not sacrifice the other five dimensions of health care quality, namely, safety, effectiveness, efficiency, equity, and patient centeredness.”10 The right treatment for the right patient at the right time is proving more effective for some patients than traditional approaches to medication selection.
With the complexities of cancer, healthcare providers need to ensure that patients and their caregivers are central to all care to be provided, taking into consideration their perceived notion of QOL, acknowledging their goals for receiving care, and confirming that their personal preferences and wishes are at the forefront in the decision-making process. Recently diagnosed cancer patients often look for approaches to become actively engaged in their care journey, evaluating what to expect as their diagnosis and treatment unfolds, its impact on their QOL, and what the future may hold. Recognizing the impetus to making appropriate healthcare decisions, they must have the ability to attain, process, and comprehend information regarding diagnostic testing and treatment options.
There is an opportunity to make the time between diagnosis and first treatment more productive and meaningful for patients and their caregivers by actively engaging them and assigning them tasks.11,12 Instead of passively sitting at home, ruminating over their diagnosis and waiting for treatment, patients and caregivers have the ability to influence the cancer trajectory by receiving individualized educational tools and options. Through such empowerment, the loss of control a newly diagnosed patient faces, compounded by feelings of distress, anxiety, and depression, is abated.
Problem
A significant outcome measure used to evaluate health status as well as treatment efficacy and survival is QOL, which encompasses the physical, psychological, social, and spiritual aspects of a patient.13-15 The diagnosis of cancer evokes a life-threatening reaction that can immediately hinder the QOL of individuals and their families. Anxiety and fear, common in the initial phase of cancer diagnosis and treatment, can be barriers to comprehension, coping, and self-care decisions. Coupled with treatment modality, side effects from disease or therapy, preexisting comorbidities, social support and well-being, and financial toxicity, QOL may be further impaired.16
Patient education, a fundamental part of high-quality care, impacts a patient’s health and QOL.17 Said educational material must span the disease trajectory, encompass the 4 domains of well-being, be accurate, up-to-date, and relevant to both the patient and caregiver while being patient-centric. However, according to their systematic review, Tzelepis and colleagues noted that 10% to 24% of cancer patients perceived a lack of pertinent information received at the time of diagnosis, and 11% to 97% expressed unmet information needs throughout treatment.18 There is currently a need for an integrated educational program for newly diagnosed patients who are between their cancer diagnosis and the start of acute treatment.
High-Level Solution
During a period of heightened distress, newly diagnosed cancer patients are barraged with information that they must try to understand to consent to a therapy plan. Accessing disease-specific information has changed considerably over time. Cancer patients and caregivers are increasingly turning to social media platforms for health-related information and support. Connecting them with appropriate, up-to-date, evidence-based information can help them self-manage more effectively.
The CAPE initiative has been developed to provide a vessel for (1) gathering high-quality, disease-specific, evidence-based educational material together on 1 platform; (2) presenting the healthcare provider with 1 source for all cancer-related information spanning the disease trajectory for patient educational purposes; and (3) providing a mechanism for healthcare providers to identify gaps within patient education, with ongoing feedback from the digital platform.
Coalition Membership Development
The CAPE initiative has been methodically designed. In preparation for building the digital educational platform, AONN+ meticulously assembled disease-specific experts, calling on members from industry, advocacy groups, and clinical experts to discuss, define, and contribute their expertise to the design of the CAPE initiative. Members of the coalition (Figure 1) met via Webex to develop a needs assessment, determine the mission and vision of the initiative, as well as to delineate goals, objectives, and deliverables. The mission and vision statements, as well as the deliverable timeline, were sent electronically to all members for further commentary. Members agreed to participate in regularly scheduled virtual meetings and occasional live meetings.
Mission and Vision Statements Defined
The Lung CAPE steering committee developed both a mission and a vision statement to guide the initiative and clearly communicate the goals and objectives to healthcare providers and cancer programs. The vision is to engage, inform, and empower newly diagnosed cancer patients utilizing a predetermined QOL model to reduce the stress and improve the patient experience between diagnosis and first treatment. The mission is to improve the patient experience from patient diagnosis to treatment with personalized education.
QOL Model Defined
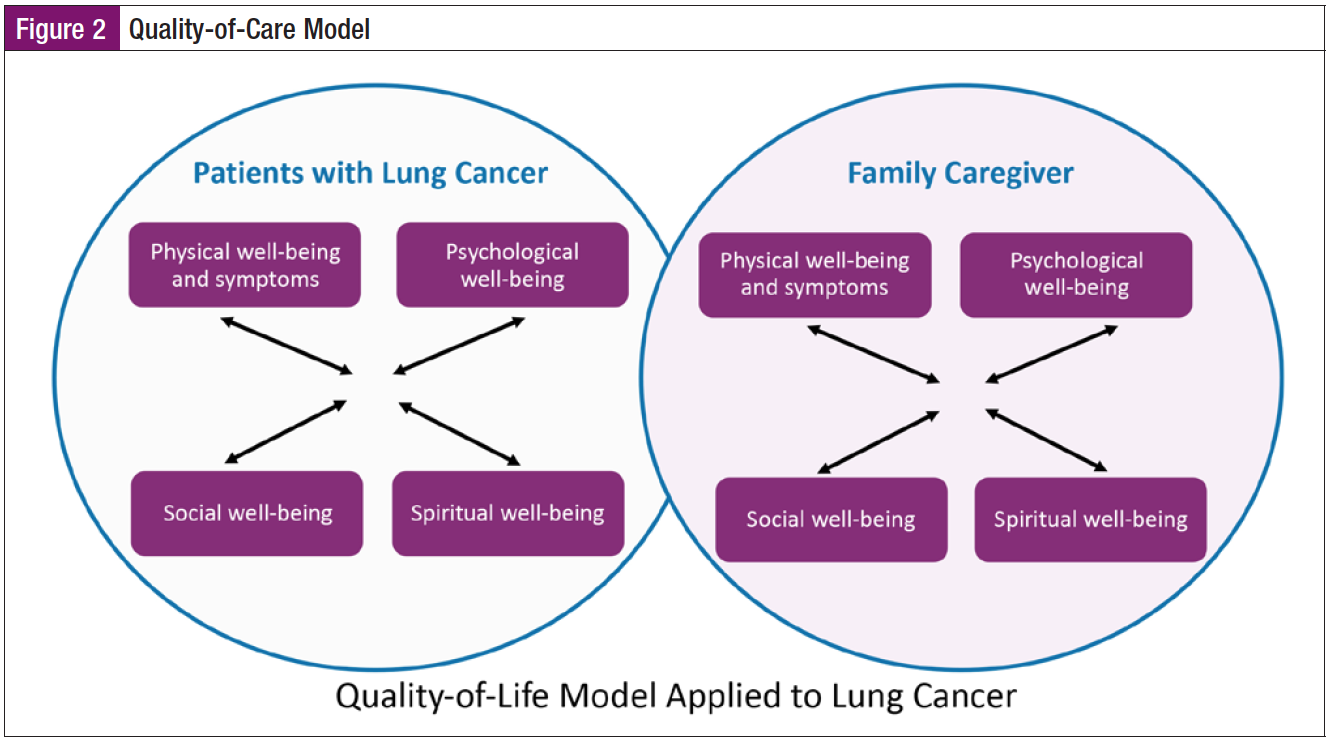
A predetermined QOL model (Figure 2) was used to inform the coalition about the educational needs and necessary evidence-based interventions relevant to each domain across the care continuum for patients and caregivers.13-15 In keeping the cancer patient and caregiver central to the QOL model’s domains of well-being, literature review search terms were identified.
Literature Review
In preparation for the development of an educational platform, members sought to determine the impact lag time between diagnosis and treatment initiation had on QOL for newly diagnosed cancer patients, given the necessary need for delay for biomarker profiling for some cancers. To answer said impact and better understand the needs and concerns of lung cancer patients and their caregivers, a literature review was conducted. Utilizing the identified search terms, and in an effort to fully define current knowledge, the review encompassed an overview of the significant scholarly works published within the past 10 years as they pertained to the domains of physical, psychological, social, and emotional well-being. The summation of the review provided the coalition with a better understanding of educational requirements to meet these needs and identified thematic trends used to describe potential education needs for the patient and caregiver. These themes evolved into specific recommendations for module development.
A comprehensive search of the published literature in the past 10 years was conducted. A total of 1610 articles were screened, 205 full-text publications were reviewed, and 50 relevant articles were identified. Findings from the review and analysis of relevant articles, using the PRISMA model, identified common areas of need/concern for patients with lung cancer and their caregivers.
After the completion of the literature review based on the 4 QOL domains (physical, psychological, social, and spiritual well-being) and the current barriers, challenges, and needs that lung cancer patients and their caregivers face during the time from diagnosis to treatment, it was essential to develop module topics for the organization of materials and resources. Seven modules were determined to address patient and caregiver needs.
Identification of Educational Material
Next, the coalition members identified existing high-quality, evidence-based, validated, and culturally/literacy-appropriate patient materials/resources/tools for each of the modules. The curated materials, in the form of websites, apps, videos, and printed material, were put through a rubric in the form of the Patient Education Materials Assessment Tool (PEMAT) to critique and evaluate the materials. PEMAT is a 7-step systematic method to evaluate and compare the understandability and actionability of patient print and audiovisual education materials. The PEMAT evaluation served as a guide to help determine whether patients would be able to understand and act on the information.19
Following completion of the PEMAT evaluation, permission for use was obtained, and the best of the best curated evidence-based validated materials were organized into the determined modules with the goal to inform, engage, and empower patients and their caregivers. Seven robust education modules have been built to address the varying aspects of the cancer journey, including the barriers and challenges plaguing newly diagnosed lung cancer patients.
Digital Education Platform Identified
Having access to evidence-based, reliable, disease-specific educational resources augments patient-provider conversations, enhances shared decision-making and adherence to treatment plans, and improves patient satisfaction, ultimately improving clinical outcomes and decreasing healthcare expenditure.1,17,20 Technologic advances, social media, and ways of accessing health-related information have encouraged the development of creative educational tool options.21 According to Xu and colleagues, 35% of adults in the United States rely on online platforms for health-related information and seek web-based resources for emotional support and practical day-to-day advice rather than seeking the same advice from their healthcare team.22
A digital education platform provides a multimedia approach to patient education and has the ability to deliver the material in a flexible and user-friendly environment. Designing a robust digital education platform will allow providers to reiterate and build on the teaching with every point of contact. Through design and implementation of an integrated digital education platform, healthcare providers will be able to socially prescribe a personalized educational plan for patients and caregivers as well as build up on the plan across the disease trajectory.23,24
In developing the CAPE initiative library, AONN+ collaborated with Takeda Oncology and a multistakeholder coalition of leading patient advocacy organizations for lung cancer. Based on the identified areas of concern, 7 modules for the integrative education program were outlined, and current best-practice resources and tools were gathered for each of the defined modules (Table). To be able to offer the modules as an integrative web-based library and allow healthcare providers and navigators to deliver a personalized digital prescription to lung cancer patients based on their needs, AONN+ established a partnership with Health Unlocked. Health Unlocked is the world’s largest social network for health with 1 million members and 4 million visitors per month.3 The social prescribing platform has been validated to improve people’s knowledge, skills, and confidence levels with regard to the management of their own health by connecting them to sources of support, community services, and evidenced-based high-quality patient education material.25,26 Social prescribing is essential to the clinical toolkit of healthcare providers and navigators to tackle wider social determinants of ill-health by focusing on what matters to patients as opposed to what’s the matter with the patients.27
Benefits
Research has shown that the most critical time for introducing navigation services is around diagnosis and staging.28,29 The benefits of an integrated educational program for patients during this period is supported by studies that show:
- Improvements in QOL and depression at 3 and 6 months when palliative care is included at the time of diagnosis in advanced lung cancer (all, P <.05)30
- The most critical time for navigation services is around diagnosis and staging28,29
- Obtaining more information during the period from diagnosis to start of treatment increases patient’s decision-making capacity and may improve patient response, thereby enhancing their quality of treatment and care, reducing anxiety and emotional distress, and promoting emotional stability with family members30
The concept of social prescribing in the care of cancer patients is communication, forming relationships, and providing information/resources that support and empower patients through their cancer journey.22,31 Through communication and assessment, healthcare providers and navigators assist patients and caregivers to identify areas of focus or need, such as taking an active role in decision-making, tips for self-care, and dealing with financial concerns. Utilizing the digital platform, relevant modules with corresponding relevant resources selected that relate to their patient or caregiver, are sent electronically to the patient or handed out in print. Using an integrative digital education platform approach, the AONN+ CAPE initiative helps cancer patients and their caregivers manage distress at the time of their diagnosis and supports them through the rigors of treatment by optimizing self-care management, securing community resources, and focusing on the enrichment of their QOL.
Summary
NSCLC, even in an advanced state, has shifted survival outcomes. Cancer patients and their caregivers face a range of emotions at the time of diagnosis. It is imperative that the healthcare team engage with patients and caregivers in a formal way to address their physical, psychological, social, and spiritual well-being throughout the cancer trajectory.30,32 Preemptively knowing patients’ educational needs fosters a positive impact on their ability to cope and improves their decision-making ability. Through robust education, presented at a time convenient for them, in a place that is conducive for learning, and in a method of their choosing, patients and caregivers will experience improved QOL and be better equipped to be active participants in their cancer journey.30 Information related to cancer diagnosis, treatments, and self-management strategies encourages patient engagement and empowers them to employ strategies to optimize physical, psychological, social, and spiritual well-being.17
The Lung CAPE steering committee developed both a mission and a vision statement to guide the initiative and clearly communicate the goals and objectives to healthcare providers and cancer programs. The vision is to engage, inform, and empower newly diagnosed cancer patients utilizing a predetermined QOL model to reduce the stress and improve the patient experience between diagnosis and first treatment. The mission is to improve the patient experience from patient diagnosis to treatment with personalized education.
The CAPE initiative is intended to be a sustainable integrative educational program to cause behavioral change delivered over the waiting period, usually 4 to 6 weeks, from diagnosis until the completion of diagnostic testing, that gives patients and caregivers a focus while waiting for biomarker test results. The parameters, therefore, begin with diagnosis, and the end point is first treatment.
CAPE will include a curriculum, educational materials, and tools for the coordinator/navigator guiding the newly diagnosed lung cancer patient. Learnings and materials will be deployed across a variety of delivery vehicles: online, hard copy, and in person. The CAPE program is ultimately intended to integrate into the existing flow of appointments/clinic days, etc, to limit time burden to patients and families. Additionally, one of the long-term, ultimate goals of CAPE is to shift the perception of the time frame between diagnosis and start of acute treatment from the “waiting period” to an active and engaged education enrichment period in the cancer care paradigm.
Plan of Action
The CAPE lung cancer web-based library will be introduced at the AONN+ 10th Annual Navigation & Survivorship Conference in November 2019 via a series of focus groups. AONN+ is also expecting to conduct a pilot study of the web-based library in 2020 involving a variety of providers and settings. When the web library is finalized, the program, along with a training webinar, will be made available to pulmonology offices, radiation and medical oncology clinics, and navigation programs.
Once the CAPE lung cancer pilot study is complete and the practical aspects of the initiative, including confirmed ease of use and justification for the program, are met, the plan is to expand the initiative to other disease sites. At this time, the initiative has been working closely with lung cancer–specific advocacy groups to ensure educational material is representative of the population needing the information. Moving forward as the initiative is expanded to other disease sites, the plan is to engage other disease-specific advocacy groups to guarantee material is pertinent to the respective population.
Acknowledgments
AONN+ would like to acknowledge the Lung CAPE steering committee members and the advocacy organizations behind the development of the program for their dedication to lung cancer patients and their caregivers. AONN+ expresses a heartfelt thank you to Takeda Oncology for its support and funding of this innovative, leveraged, and evidence-based program.
References
- Mann KS. Education and health promotion for new patients with cancer. Clin J Oncol Nurs. 2011;15:55-61.
- Fujinami R, Otis-Green S, Klein L, et al. Quality of life of family caregivers and challenges faced in caring for patients with lung cancer. Clin J Oncol Nurs. 2012;16:E210-E220.
- Health Unlocked. https://about.healthunlocked.com. 2019.
- Gould MK. Delays in lung cancer care: time to improve. J Thorac Oncol. 2009;4:1303-1304.
- Nadler E, Espirito JL, Pavilack M, et al. Treatment patterns and clinical outcomes among metastatic non-small-cell lung cancer patients treated in the community practice setting. Clin Lung Cancer. 2018;19:360-370.
- Kris MG, Johnson BE, Berry LD, et al. Using multiplexed assays of oncogenic drivers in lung cancers to select targeted drugs. JAMA. 2014;311:1998-2006.
- Lim C, Tsao MS, Le LW, et al. Biomarker testing and time to treatment decision in patients with advanced nonsmall-cell lung cancer. Ann Oncol. 2015;26:1415-1421.
- Bullard JT, Eberth JM, Arrington AK, et al. Timeliness of treatment initiation and associated survival following diagnosis of non-small-cell lung cancer in South Carolina. South Med J. 2017;110:107-113.
- Labbé C, Anderson M, Simard S, et al. Wait times for diagnosis and treatment of lung cancer: a single-centre experience. Curr Oncol. 2017;24:367-373.
- Maiga AW, Deppen SA, Pinkerman R, et al. Timeliness of care and lung cancer tumor-stage progression: how long can we wait? Ann Thorac Surg. 2017;104:1791-1797.
- Johansen C, Dalton SO. Survivorship in new harbors. Acta Oncol. 2017;56:119-122.
- Silver JK, Biama J. Cancer prehabilitation: an opportunity to decrease treatment-related morbidity, increase cancer treatment options, and improve physical and psychological health outcomes. Am J Phys Med Rehabil. 2013;92:715-727.
- Ferrell BR, Hassey Dow K. Quality of life among long-term cancer survivors. Oncology (Williston Park). 1997;11:565-568, 571.
- Ferrell BR, Dow HK, Grant M. Measurement of the quality of life in cancer survivors. Qual Life Res. 1995;4:523-531.
- Grant M, Padilla GV, Ferrell BR, Rhiner M. Assessment of quality of life with a single instrument. Semin Oncol Nurs. 1990;6:260-270.
- Polat U, Arpacı A, Demir S, et al. Evaluation of quality of life and anxiety and depression levels in patients receiving chemotherapy for colorectal cancer: impact of patient education before treatment initiation. J Gastrointest Oncol. 2014;5:270-275.
- Aghakhani N, Nia HS, Ranjbar H, et al. Nurses’ attitude to patient education barriers in educational hospitals of Urmia University of Medical Sciences. Iran J Nurs Midwifery Res. 2012;17:12-15.
- Tzelepis F, Sanson-Fisher RW, Zucca AC, Fradgley EA. Measuring the quality of patient-centered care: why patient-reported measures are critical to reliable assessment. Patient Prefer Adherence. 2015;9:831-835.
- Agency for Healthcare Research and Quality. The Patient Education Materials Assessment Tool (PEMAT) and User’s Guide. www.ahrq.gov/professionals/prevention-chronic-care/improve/self-mgmt/pemat/index.html. April 2017.
- Frentsos JM. Use of videos as supplemental education tools across the cancer trajectory. Clin J Oncol Nurs. 2015;19:E126-E130.
- Koh HK, Berwick DM, Clancy CM, et al. New federal policy initiatives to boost health literacy can help the nation move beyond the cycle of costly ‘crisis care.’ Health Aff (Millwood). 2012;31:434-443.
- Xu R, Zhou J, Zhang Q, Hendler JA. Research on Online Health Communities: A Systematic Review. In: Alhajj R, Rokne J, eds. Encyclopedia of Social Network Analysis and Mining. New York, NY: Springer; 2018.
- Samson K. Web-based guideline tool increases NSCLC patients in decisions. Oncology Times. 2019;41(8):26.
- Common JL, Mariathas HH, Parsons K, et al. Reducing wait time for lung cancer diagnosis and treatment: impact of a multidisciplinary, centralized referral program. Can Assoc Radiol J. 2018;69:322-327.
- Healthy London Partnership. How to introduce a social prescribing champion model and/or a digital platform to support your social prescribing offer. www.healthylondon.org/wp-content/uploads/2018/12/How-to-introduce-a-social-prescribing-champion-model.pdf. 2018.
- Healthy London Partnership. Case study: Primary Care Networks in North Central London – Islington GP Federation – March 2019. www.healthylondon.org/resource/case-study-primary-care-networks-in-north-central-london-islington-gp-federation.
- General Medical Council. Outcomes for Graduates 2018. www.gmc-uk.org/-/media/documents/dc11326-outcomes-for-graduates-2018_pdf-75040796.pdf. Accessed July 7, 2019.
- Allison L. Oncology care coordination in two settings. Journal of Oncology Navigation & Survivorship. 2018;9(4):146-148.
- Thygesen MK, Pedersen BD, Kragstrup J, et al. Benefits and challenges perceived by patients with cancer when offered a nurse navigator. Int J Integr Care. 2011;11:e130.
- Balboni TA, Hui KP, Kamal AH. Supportive care in lung cancer: improving value in the era of modern therapies. Am Soc Clin Oncol Educ Book. 2018;38:716-725.
- Mettler M, Kemper DW. Information therapy: the strategic role of prescribed information in disease self-management. APLAR Journal of Rheumatology. 2005;8(2):69-76.
- Bau I, Logan RA, Dezii C, et al. Patient-centered, integrated health care quality measures could improve health literacy, language access, and cultural competence. NAM Perspectives. Discussion Paper, National Academy of Medicine, Washington, DC. https://nam.edu/patient-centered-integrated-health-care-quality-measures-could-improve-health-literacy- language-access-and-cultural-competence.