The diagnosis of cancer can be overwhelming for patients and their families, and the process of cancer treatment is often complex and fragmented. Many patients have limited knowledge on how to adapt or navigate through different aspects of their cancer journey. As an integral part of oncology treatment and patient care, patient navigation has emerged as a nationally recognized healthcare service delivery model that is designed to eliminate barriers to timely care and coordinating treatment across all segments of the cancer care continuum. Through close and continued involvement with patients after a cancer diagnosis is made, oncology nurse navigators (ONNs) empower patients to take charge of their health by providing education to patients and their families so they can make informed decisions, offering resources, facilitating communication, and healthcare planning. In this article, the role of ONNs in providing support to patients with hematologic malignancies to empower them to participate in decisions regarding their care will be discussed.
Oncology Nurse Navigation Explained
The discipline of nurse navigation program has evolved substantially since its introduction in 1990 due to its positive contribution to quality patient-centered care.1,2 The Academy of Oncology Nurse & Patient Navigators (AONN+) defines a nurse navigator as “a clinically trained individual responsible to identify and address barriers to timely and appropriate cancer treatment.”3
The AONN+ has identified that ONNs must demonstrate knowledge in the several overarching domains of care to provide quality patient-centered care (Figure).3,4
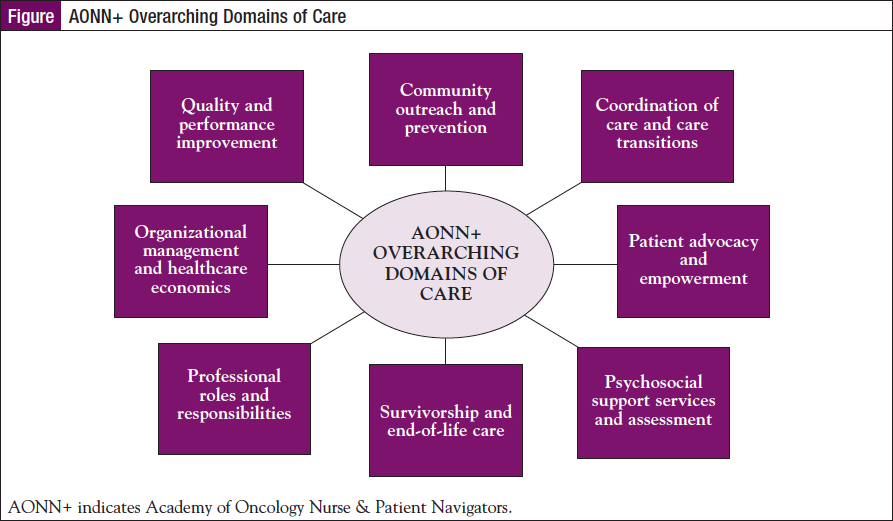
Within each domain, there are a number of national evidence-based metrics, allowing all navigation programs to utilize the same metrics to measure success and sustainability.
The Oncology Nursing Society has also established a list of core competencies to describe ONN roles and responsibilities.5 Broadly, these competencies are described under 4 functional categories: coordination of care, overcoming healthcare system barriers, education, and professional role. An important responsibility of ONNs is to educate and provide resources to patients and their caregivers to facilitate informed decision-making and timely access to quality health and psychosocial care throughout all phases of the cancer care continuum.5
Although the core concepts of navigation remain the same, different cancer centers may have adopted different navigation models to achieve these goals. As a result, the specific scope and responsibilities of ONNs may differ across institutions. Regardless, an ONN has the clinical background necessary to help patients and is a critical member of the multidisciplinary cancer team.3 Nurse navigators guide patients through the cancer care continuum and serve as a central point of contact for patients through each stage of treatment. Nurse navigators serve on the multidisciplinary team that may consist of multiple physicians, including surgeons, radiologists, and medical oncologists and other providers such as physician assistants or nurse practitioners, financial navigators, pharmacists, and social workers. However, a patient’s contact with multiple healthcare team members can complicate a patient’s ability to confidently approach their care. An integral part of the nurse navigator’s unique role is to serve as a clinically informed liaison between the patients and their healthcare team.
A fundamental role of the ONN is to educate the patient, their family, and caregivers to ultimately empower them to make informed decisions about their care.6 Oftentimes, health literacy is an important hurdle for the patient, and understanding the medical jargon may be very daunting.7,8 To address this barrier, ONNs are extensively involved in explaining medical terminology and educate on various aspects of care to patients extending from treatment plans to psychosocial health. Toward that end, ONNs must be knowledgeable about the ever- changing landscape for general protocol, management, and treatment options for a given diagnosis. Generally, a nurse navigator builds a rapport with the patient and gains an in-depth understanding of each patient’s unique situation that allows them to identify barriers to care and mitigate them as needed. As such, they are readily able to communicate with a patient and their healthcare team regarding the patient’s changing needs. Ultimately, ONNs facilitate a patient’s timely access to quality healthcare and are available to explain or assist a patient throughout the complex cancer trajectory.
Hematologic Malignancies
Hematologic malignancies are a broad group of heterogeneous cancers that affect blood, bone marrow, and lymph nodes. Main subcategories of hematologic malignancies include leukemias, lymphomas, multiple myeloma (MM), and myeloproliferative disorders.9 Lymphomas originate in lymphatic tissue of the body (eg, lymph nodes, spleen, thymus) and result from overproduction of lymphocytes; the 2 major subtypes are non-Hodgkin lymphoma and Hodgkin lymphoma. Leukemia occurs due to abnormal production of white blood-cells; 4 main types of leukemia are recognized: acute myeloid leukemia (AML), chronic myeloid leukemia (CML), acute lymphocytic leukemia, and chronic lymphocytic leukemia (CLL). MM is a cancer that originates from plasma cells, with excess production of plasma cells crowding bone marrow and limiting growth of other blood cell types. Additionally, myelodysplasia is considered a precancerous disease of bone marrow that can progress to an acute leukemia.10
Hematologic malignancies account for approximately 10% of all newly diagnosed cancer cases in the United States.11 Altogether, hematologic malignancies account for around 9% of annual cancer-related deaths. With recent treatment advances, the 5-year survival rate for leukemia, lymphoma, and MM exceeds 50%.11
The treatment landscape for hematologic malignancies is complex and continuously evolving, with treatment strategies dependent on the stage and aggressiveness of the disease, the patient’s health status, and the goals of treatment. Based on the treatment goals, phases of treatment in some subtypes may include an induction phase (the primary and initial treatment), a consolidation phase (enhancing or adding to the initial treatment, also known as intensification therapy and postremission therapy), and a maintenance phase (to maintain the remission achieved in previous phases). Broadly, treatment strategies include active surveillance, surgery, chemotherapy, biologic and targeted therapy, immunotherapy, radiation therapy, and stem-cell transplantation (SCT). Whereas chemotherapy kills all rapidly proliferating cells, targeted therapies are designed to target specific molecular entities in a cancer cell to produce antitumor effects. Immunotherapies such as checkpoint inhibitors harness the body’s immune system to launch an antitumor response. SCT is a major treatment modality that holds curative potential for hematologic disorders by facilitating restoration of the patient’s immune system by replacing the bone marrow cell repertoire. SCT may be autologous (using patient’s own stem-cells) or allogeneic (using stem-cells collected from a matched donor), each with associated risks and benefits. Several biologic and targeted agents have been introduced for hematologic malignancies and have revolutionized the management of many of these cancers; newer agents continue to be developed to improve patient outcomes.12 Multiple treatment modalities may be recommended, either sequentially or concomitantly, over the course of treatment. Choice of treatment at a given point in time depends on many patient- and disease-specific factors.
Role of ONNs: Unique Challenges of Hematologic Malignancies
While the core competencies required remain the same, ONNs involved in the care of patients with hematologic malignancies face unique challenges that are multifold. Inherently, hematologic malignancies are a diverse group of cancers that are associated with distinct pathobiologies, etiologies, incidence, and disease courses and thereby are associated with different prognoses and survival.13 These differences have warranted distinct treatment strategies, which are documented in clinical treatment guidelines developed for each subtype.13 Therefore, ONNs must be well-informed about the different cancer subtypes and the evolving treatment landscape. A particular challenge is to keep abreast of the large number of new therapies in hematologic malignancies, including combination therapies. They must understand and be able to address important clinical nuances specific to different types and subtypes. ONNs must then educate the patients about their cancer subtype so they may be empowered to make informed decisions regarding their care.
Hematologic malignancies exhibit a diverse clinical course, with some fast-growing and aggressive (eg, diffuse large B-cell lymphoma [DLBCL]), others showing an indolent disease course (eg, follicular cell lymphoma), and a few showing an indolent phenotype for extended periods and then transforming to an aggressive cancer (eg, CLL undergoing Richter’s transformation into aggressive DLBCL). Similarly, the natural courses of AML and CML are different, with CML showing a relatively slow disease progression; smoldering myeloma can also show a fulminating course and progress rapidly to MM. Because most hematologic malignancies are not curable and are characterized by recurring periods of remission followed by eventual relapse, ONNs must be prepared for extensive follow-up, relapses, complications of disease, side effects of ongoing treatment, or potential outcomes after perceived success of treatment.14 A nurse navigator’s knowledge of hematologic malignancies and the variable outcomes associated with them is thus paramount to be competent as a navigator in educating patients.
Diagnosis
Following the diagnosis of a hematologic malignancy, regardless of the subtype, the ONN helps the patients cope with the diagnosis itself and empowers them by providing education on their cancer subtype and prepares them for their cancer journey in terms of further testing they may have to undergo, treatment, and overall prognosis. Many diagnostic tests are performed if a physician suspects a hematologic malignancy, and all tests that ensue are uniquely tailored to the suspected diagnosis. The definitive diagnosis of these malignancies often requires performing several tests, including laboratory tests, imaging assessments, bone marrow aspiration, and biopsy. In this setting, the ONN plays an important role in explaining the results of these tests, the necessity of each diagnostic test, and what information it adds to the diagnosis and subsequent treatment. This education can also facilitate more informed participation by the patient in the shared decision-making process. Further, ONNs can also assist a patient’s comprehension of the planned schedule for future testing.
Treatment and Side Effect Management
As evidenced in the NCCN guidelines, treatment strategies are diverse and complex for patients diagnosed with hematologic malignancies.13 Cancer therapy prescribed for a patient may be challenging to understand and adhere to; the ONN educates the patient on rationale for treatment, importance of treatment adherence, treatment outcomes, and side effect management. Based on the treatment plan developed for the cancer subtype, some patients may require years of therapy and follow-up care. For some patients on an active surveillance strategy, depending on a patient’s symptoms, risk factors, health status, or any number of factors, a physician may choose to begin or hold off on initiating therapy. The ONNs must educate patients on the importance of routine surveillance and address the emotional health component associated with this strategy.
For patients prescribed active treatment, several treatment options are available either as a single modality or combination strategies (ie, surgery, chemotherapy, biologic and targeted therapy, immunotherapy, radiation therapy, and SCT). Each treatment modality has different short-term and long-term implications for patients, and the ONN must educate them about each of these implications. Some patients may receive multiple treatment modalities, highlighting the complexity of treatment regimens for many hematologic malignancies. Chemotherapy may be administered orally or intravenously, as a single agent or as a multiagent therapy, as a primary treatment modality, or after surgery (adjuvant chemotherapy) prior to SCT to decrease disease burden. The patient must be educated on the rationale for chemotherapy in each of these scenarios, and potential side effects explained.
SCT remains an important treatment modality that provides a potential for cure for many lymphomas and MM; however, given that it is a complex procedure that may be associated with significant morbidity and mortality, careful patient selection is key.15,16 The procedure involves stem-cell mobilization, administration of high-dose chemotherapy and myeloablative doses of radiation followed by reinfusion of stem-cells (either autologous or allogeneic). Allogeneic SCT is associated with risk of graft-versus-host disease that requires the use of immunosuppressive agents, such as anti–T-cell globulin, tacrolimus, cyclosporine, and methotrexate.15,17 Together, patients undergoing SCT, particularly allogeneic SCT, require intensive monitoring and follow-up and need significant education on the procedure and risks involved, need for compliance of immunosuppressive agents, and toxicity management.
Several classes of biologic and targeted agents are recognized, including tyrosine kinase inhibitors (eg, imatinib, bosutinib, dasatinib, nilotinib), Bruton’s tyrosine kinase inhibitors (eg, ibrutinib and acalabrutinib), monoclonal antibodies directed toward key molecules such as CD20 (eg, rituximab), CD38 (eg, daratumumab), proteasome inhibitors (eg, bortezomib, ixazomib), and immunotherapy (eg, pembrolizumab, nivolumab) that are approved for different hematologic malignancies; each is associated with distinct side effects and risks. For example, peripheral neuropathy is a notable side effect of bortezomib and ixazomib that are used for the treatment of MM, whereas infusion reactions are typically associated with monoclonal antibodies.18 A key role of ONNs is to encourage patients to identify and report any unusual treatment-related side effects. Supportive care for management of treatment-emergent adverse effects may include addressing bone disease, hypercalcemia, hyperviscosity of the blood, anemia, infection, renal dysfunction, coagulation/thrombosis, fatigue, nausea, vomiting, diarrhea, loss of appetite, increased susceptibility to infection, or pain. ONNs can further empower patients by educating them on strategies that will help them take an active role in their self-care, such as exercise and maintaining a healthy diet.
The newer class of checkpoint inhibitors is associated with a unique set of adverse events known as immune-related adverse events (irAEs) that are commonly dermatologic, endocrine, hepatic, and gastrointestinal events.19 Although these are typically grade 1 or 2, early recognition and timely intervention are critical for their management.20-22 ONNs must use individualized patient education on symptom recognition, screening, and assessment for the early identification of irAEs.19
Enrollment in clinical trials is also an integral treatment option for many hematologic subtypes. Importantly, patients might have many misconceptions about clinical trial participation, including that clinical trials are appropriate only for patients who have exhausted all standard therapies; experimental treatment might potentially be unsafe, ineffective, and costly; and only placebos are used.23 Therefore, ONNs must possess a functional understanding of the clinical trial process and be well-informed about the potential benefits and risks of clinical trial participation. Because of their rapport with the patient, ONNs can evaluate patient receptivity to participation and share their insights with appropriate members of the multidisciplinary care team with clinical trial responsibilities.
Survivorship
Life expectancy has improved for many hematologic cancers due to treatment breakthroughs, with many patients now achieving deep and durable remissions. Survivorship is associated with its own share of severe medical, economic, and healthcare consequences.24 The overall burden of illness among survivors is significantly worse than that of their age-matched noncancer survivor control counterparts.25 In 2006, an Institute of Medicine report showed that cancer survivors were not receiving the comprehensive and coordinated follow-up care they require, and that many get lost in transition after completion of treatment.26 For this reason, the role of the ONN in the survivorship phase of a patient’s cancer journey is critical. Despite achieving clinical remission following successful treatment completion, patients are still at risk for cancer recurrence or late effects of treatment. ONNs must educate patients about these consequences and empower them to manage their expectations and disease.
Psychosocial Health
The nurse navigator has an important role in educating and empowering patients in terms of their psychosocial well-being. An estimated 50% to 90% of patients with cancer experience psychosocial distress to some degree due to fear of recurrence, inability to make plans, uncertainty, heightened sense of vulnerability, consequences of disease on employment, health insurance, social functioning, and parenting.27 Such elevated levels of emotional distress are also associated with decreased adherence to treatment, poor health-related quality of life, poor satisfaction with medical care, decreased employment functioning, increased health risk behaviors, worse survival, higher medical costs, and overall greater burden on the medical system.13 Thus, the role of the ONN in this regard is crucial. Given the rapport that an ONN seeks to maintain with the patient, they are well suited to monitor the patient’s psychosocial needs. When appropriate, the nurse navigator can validate a patient’s experience and educate them on available resources. Resources could include, for example, access to psychiatrists or counselors, access to support groups, or access to more educational information on the subject.13,27
Conclusion
ONNs play a pivotal role on the multidisciplinary teams that serve cancer patients. These specialists work hand in hand with patients throughout their cancer trajectory by educating and connecting them to resources, information, and support, and thereby empowering them to adequately manage their cancer. The heterogeneity of hematologic malignancies poses exceptional challenges to ONNs, requiring a broad knowledge base to provide optimal patient care. Although the role, duties, and training of ONNs will continue to evolve as standards and competencies are further defined, their contribution to patient care fundamentally helps to alleviate some of the burden patients would otherwise have to face navigating their cancer journey.
CLL Case Study
The following case study illustrates the role of an ONN throughout the course of a patient’s care with a diagnosis of CLL.
Jill is a 49-year-old female who initially presented with new axillary adenopathy. Follow-up testing included blood labs, CT imaging of her chest and abdomen, and a lymph node biopsy. Biopsy results confirmed a diagnosis of chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL), Rai stage I, and imaging showed multiple enlarged bilateral axillary nodes. Jill was deemed to have a favorable prognosis due to being CD38 negative. The decision was made to enter a “watchful waiting” period.
Upon receiving her diagnosis, Jill was introduced to her nurse navigator, Suzy, who explained her role on the healthcare team and how she would be involved in Jill’s care. Jill shared that she did not fully understand what CLL/SLL was, so Suzy explained the complicated medical jargon used by the provider in layman’s terms, making sure to fill in any remaining gaps of comprehension or confusion. Once all of Jill’s questions were answered, Suzy gave Jill her number and explained the care plan once again, discussed follow-up appointments, and planned lab testing. Suzy instructed Jill on what to do should she begin to experience new or unsettling symptoms like night sweats, fevers, unintentional weight loss, worsening fatigue, or changes in her lymph node size. Suzy also gave Jill informational pamphlets with information about her disease and resources for social support. While Jill felt uneasy about her diagnosis and slightly overwhelmed, she found Suzy’s discussion helpful and felt reassured by knowing that she could contact Suzy at any point if she needed further help.
For 5 years following this appointment, Jill returned to the clinic every 3 months for lab tests and every 6 months to see her provider. In 2015, Jill reached out to Suzy with worsening symptoms. Suzy promptly set Jill up for a same-day appointment. Repeat labs were significant for worsening cell counts, and a CT scan confirmed worsening adenopathy. Jill was started on a treatment regimen of chlorambucil and prednisone as a bridge to ibrutinib. Suzy explained the treatment plan, possible treatment-emergent adverse effects to expect, as well as the plan to follow up in the clinic every 3 months. Suzy explained Jill’s risk of tumor lysis, and how taking allopurinol and increasing her fluid intake will help combat it. She answered Jill’s concerns and questions and reminded her to call if she needed any further help. After 4 years, Jill continues to receive ibrutinib, has not progressed, and has periodic contact with Suzy. When they speak, Suzy reinforces the possibility of recurrence, risk of developing long-term adverse effects, and the importance of ongoing surveillance. Suzy continues to remain in touch with Jill during her ongoing treatment.
References
- American College of Surgeons. Commission on Cancer. Cancer Program Standards 2012: Ensuring Patient-Centered Care. www.facs.org/cancer/coc/programstandards2012.pdf. 2012. Accessed October 7, 2019.
- Freeman HP. The origin, evolution, and principles of patient navigation. Cancer Epidemiol Biomarkers Prev. 2012;21:1614-1617.
- Academy of Oncology Nurse & Patient Navigators. https://aonnonline.org. 2019. Accessed October 9, 2019.
- Strusowski T, Sein E, Johnston D, et al. Standardized evidence-based oncology navigation metrics for all models: a powerful tool in assessing the value and impact of navigation programs. Journal of Oncology Navigation & Survivorship. 2017;8:220-243.
- Baileys K, McMullen L, Lubejko B, et al. Nurse navigator core competencies: an update to reflect the evolution of the role. Clin J Oncol Nurs. 2018;22:272-281.
- Oncology Nursing Society. Oncology Nurse Navigator Core Competencies. www.ons.org/sites/default/files/ONNCompetencies_rev.pdf. Accessed October 9, 2019.
- American Medical Association. Health literacy and patient safety: Help patients understand. www.pogoe.org/sites/default/files/Health%20Literacy%20-%20Reducing%20the%20Risk%20by%20Designing%20a%20Safe,%20Shame-Free%20Health%20Care%20Environment.pdf. 2007. Accessed October 9, 2019.
- Kutner M, Greenberg E, Jin Y, Paulsen C. The Health Literacy of America’s Adults: Results from the 2003 National Assessment of Adult Literacy. US Department of Education. Washington, DC: National Center for Education Statistics (NCES 2006-483). http://nces.ed.gov/pubsearch/pubsinfo.asp?pubid=2006483. 2006.
- National Cancer Institute. Dictionary of Cancer Terms. Bethesda, MD: National Cancer Institute. www.cancer.gov/publications/dictionaries/cancer-terms. 2019. Accessed October 9, 2019.
- MDS Foundation. What is MDS? www.mds-foundation.org/what-is-mds. Accessed October 9, 2019.
- Surveillance, Epidemiology, and End Results Program. Cancer Stat Facts. www.seer.cancer.gov. 2019. Accessed October 9, 2019.
- US Food & Drug Administration. Hematology/Oncology (Cancer) Approvals and Safety Notifications. www.fda.gov/drugs/resources-informa tion-approved-drugs/hematologyoncology-cancer-approvals-safety-notifications. 2019. Accessed October 9, 2019.
- National Comprehensive Cancer Network. Guidelines for treatment of cancer by site. www.nccn.org/professionals/physician_gls/default.aspx#site. 2019. Accessed October 9, 2019.
- American Cancer Society. Key Statistics for Non-Hodgkin Lymphoma. www.cancer.org/cancer/non-hodgkin-lymphoma/about/key-statistics.html. 2019. Accessed October 9, 2019.
- Barton-Burke M, Dwinell DM, Kafkas L, et al. Graft-versus-host disease: a complex long-term side effect of hematopoietic stem cell transplant. Oncology (Williston Park). 2008;22:31-45.
- Singh N, Loren AW. Overview of hematopoietic cell transplantation for the treatment of hematologic malignancies. Clin Chest Med. 2017;38:575-593.
- Singh AK, McGuirk JP. Allogeneic stem cell transplantation: a historical and scientific overview. Cancer Res. 2016;76:6445-6451.
- American Cancer Society. Drug Therapy for Multiple Myeloma. www.cancer.org/cancer/multiple-myeloma/treating/chemotherapy.html. 2019. Accessed October 9, 2019.
- Myers G. Immune-related adverse events of immune checkpoint inhibitors: a brief review. Curr Oncol. 2018;25:342-347.
- Bajwa R, Cheema A, Khan T, et al. Adverse effects of immune checkpoint inhibitors (programmed death-1 inhibitors and cytotoxic T-lymphocyte-associated protein-4 inhibitors): results of a retrospective study. J Clin Med Res. 2019;11:225-236.
- Brahmer JR, Lacchetti C, Schneider BJ, et al. Management of immune-related adverse events in patients treated with immune checkpoint inhibitor therapy: American Society of Clinical Oncology clinical practice guideline. J Clin Oncol. 2018;36:1714-1768.
- Postow MA, Sidlow R, Hellmann MD. Immune-related adverse events associated with immune checkpoint blockade. N Engl J Med. 2018;378:158-168.
- Napolitano E. Clearing Up Myths and Misconceptions about Clinical Trials. Memorial Sloan Kettering Cancer Center. www.mskcc.org/blog/clearing-clinical-trials-myths-and-misconceptions. 2014.
- American Cancer Society. Managing Cancer as a Chronic Illness. www.cancer.org/treatment/survivorship-during-and-after-treatment/when-cancer-doesnt-go-away.html. 2019. Accessed October 9, 2019.
- Yabroff KR, Lawrence WF, Clauser S, et al. Burden of illness in cancer survivors: findings from a population-based national sample. J Natl Cancer Inst. 2004;96:1322-1330.
- Institute of Medicine and National Research Council. From Cancer Patient to Cancer Survivor: Lost in Transition. Washington, DC: National Academies Press; 2006.
- Institute of Medicine. Cancer Care for the Whole Patient: Meeting Psychosocial Health Needs. Washington, DC: National Academies Press; 2008.



