Medical buzzwords such as immunotherapy, precision medicine, targeted therapies, and personalized medicine have flooded headlines over the years and are the center of many clinical discussions. These treatment modalities target a tumor’s specific genetic composition after various biospecimens (eg, tumor, blood, or saliva) are collected and next-generation panel testing is performed. Today, genetics and genomics are fully integrated in oncology standard-of-care pathways in professional guidelines such as those from the National Comprehensive Cancer Network (NCCN).
Genetic counselors are board-certified healthcare professionals with uniquely specialized graduate degrees in clinical genetics and counseling. A growing number of states require that genetic counselors are both licensed and board-certified practitioners. Genetic counselors work as members of a multidisciplinary healthcare team, providing genetic testing, test interpretation, risk assessment, education, and support to individuals and families at risk for, or diagnosed with, inherited conditions.1 Genetic counselors inform and advise individuals and families of their risks for passing down or inheriting disease, genetic and familial risk estimates, individualized risk management, preventive measures, and treatment options. They are also responsible for interpreting and relaying genetic test results to patients, families, and physicians. In addition, they work with individuals who are at risk of passing down or developing inherited disorders or disease risks to compose a personalized risk reduction or risk response plan that may, in part, include reproductive support, specialty clinic referral, enhanced screening, or risk reduction surgery. Many genetic counselors specialize in specific areas, such as prenatal genetics, assisted reproductive technology, pediatric disorders, cardiovascular genetics, cancer genetics, and other specialty sites. Physicians or other healthcare providers often refer patients who have a family history of a specific disease to genetic counselors for their expertise.
The scope of practice for nursing started to include genetics in the 1970s.2 More recently, nurses are specializing in genetics. The term “genetic counselor extenders” has also emerged in the nursing domain.3 Oncology nurses require relevant and continuing education to be effective in their evolving roles.4 It is vital that oncology nurses and patient navigators are equipped to address the role of personalized medicine with their patients across the continuum of care from prevention, screening, diagnosis, treatment, surveillance, and into survivorship. Evolving nursing competencies require our expanded knowledge of genetics and genomics.
Integrating Genetics and Genomics in Oncology Nursing Practice
Incorporating genetics and genomics in oncology nursing care ensures we are contributing to advancing treatment modalities and care for our current and future patients.5 This same principle applies to navigators who are the frontline communicators between patients and the oncology care team.
In previous decades, oncology nurses had limited discussions with patients about genetics. The responsibilities of the oncology nurse with involvement in genetics have evolved significantly in recent years. Oncology nurses now help to collect and assess medical history and family history information to help identify patients for whom genetic counseling and testing may be appropriate. They also play a role in educating patients about the risk assessment and genetic testing process, referring patients to a certified genetic counselor for risk management, reviewing the essential elements for informed consent, ensuring patients that genetic information is confidential, and facilitating management based on genetic test results.4 Oncology nurses are also vital facilitators of cascade testing, which involves getting at-risk family members informed about their risk and tested when a known genetic variant is present in the family.
The Oncology Nursing Practice core competencies from the Oncology Nursing Society do not specifically list genetics as a scope. Instead, genetics/genomics can be included in the daily practice through coordination of patient care, assistance to patients and their families with healthcare system barriers, and provision of education and resources about genetic screening and diagnosis, and how they determine treatment planning.6
Similarly, the Academy of Oncology Nurse & Patient Navigators (AONN+) Oncology Navigation competencies do not list genetics as a core competency, yet it is relevant in our patient care as we educate patients and caregivers on the multidisciplinary nature of cancer. We must expand our knowledge and practice regarding genetic/genomic screening as it relates to cancer screening, diagnosis, and treatment options, including clinical trials and surveillance into survivorship.7
In 2016, the American Nurses Association and the International Society of Nurses in Genetics (ISONG) released Genetics/Genomics Nursing: Scope and Standards of Practice. This collaborative publication includes 16 standards with illustrative case examples. It provides information oncology nurses need to be comfortable addressing with their patients who have genetic-related needs.4 AONN+ Oncology Nurse Navigator–Certified Generalist includes genetics in the domain of Community Outreach/Prevention.8
This article serves to increase our knowledge about genetics so that we are better equipped to collaborate with care teams and meet the genetics/genomics needs of our patients and their at-risk family members. In the next sections, we review some basic genetic concepts.
Basic Genetic Concepts Overview9
Genes, DNA, Chromosomes
Genes, DNA, and chromosomes collectively make up the blueprint of all living things. In humans, these are the blueprints that tell the body what type of proteins to make for each human tissue and organ to function.
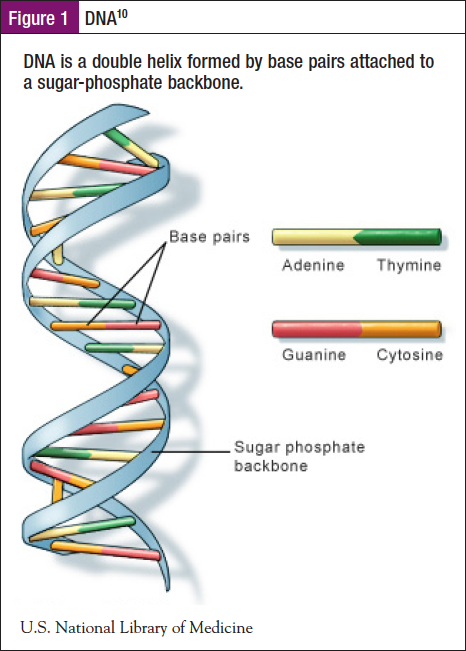
The basic unit of all life is our DNA (Figure 1). DNA is a double-stranded molecule made up of 4 chemical bases: adenine (A), guanine (G), cytosine (C), and thymine (T). Think of it as 2 rungs of a ladder that have been turned to form a helix, much like a spiral staircase. Each strand of the DNA is the side of the ladder held together by each step. Step A pairs with step T, and step G pairs with step C. Each pairing is called a base pair. The human genome contains approximately 3 billion of these base pairs, which reside in the 23 pairs of chromosomes within the nucleus of all our cells. Each chromosome contains hundreds to thousands of genes, which carry the instructions for making proteins. More than 99% of those bases are the same in all people, regardless of ancestry. The order, or sequence, of these bases determines the information available for building and maintaining an organism, similar to the way in which letters of the alphabet appear in a certain order to form words (DNA), which shape into sentences (genes) that are part of a story (protein). Our DNA is our unique story.
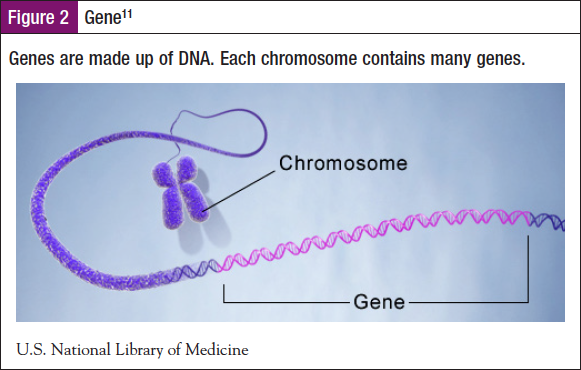
A gene is a basic unit of DNA that is located on a chromosome (Figure 2) and controls the development of 1 or more traits. It is the means by which genetic information is passed from parent to offspring. Some genes act as the instruction manual (coding genes) for making proteins. However, not all genes have this function and serve other important roles in the body. Only about 1% of DNA is made up of protein-coding genes. Astonishingly, the other 99% is noncoding. This noncoding DNA used to be considered “junk DNA,” with no function or purpose. However, we now know that at least some of it is critical for cell regulation. There is a tremendous amount of variability in the size of genes, ranging from a few hundred to well over 2 million bases. While it was once believed that humans had 50,000 genes, the current estimate is roughly 25,000.
Basically, everyone has 2 copies of most genes, 1 inherited from their mother and 1 inherited from their father. There are exceptions to this. Because females have 2 X chromosomes and males have an X and a Y chromosome, males may have only 1 copy of the genes on the X chromosome and therefore be more at risk of X-linked conditions. Most genes are functionally the same across all people, but a small number of base pairs are slightly different. Alleles are forms of the same gene with subtle differences in their DNA sequence. These differences are what makes us all unique, but they do not cause disease.
Two terms are used to describe the genetic makeup of an individual and the outward appearance of that genetic makeup—genotype and phenotype. The genotype is a person’s unique combination of genes. Thus, the genotype is a complete set of instructions on how that person’s body manufactures proteins and how that body is supposed to function. The phenotype is the actual structure and function of a person’s body. The phenotype typically differs somewhat from the genotype because not all the instructions in the genotype may be expressed. Simply put, the genotype is the internal genetics that are unique to that individual, whereas the phenotype is the outward appearance or expression of that genetic message. Whether and how a gene is expressed is determined not only by the genotype but also by the environment, which could include illnesses, diet, exposures, and other factors, some of which are unknown.
Chromosomes are structures within cells that contain a person’s genes (Figure 3). Chromosomes are long orderly strings of DNA located in the nucleus of most cells. Each chromosome is made up of DNA tightly coiled around protein structures known as histones. Humans have 23 pairs of chromosomes, for a total of 46. Twenty-two of these pairs (autosomes) are the same in both males and females. The 23rd pair (sex chromosomes) determines our sex, with males having an XY pair and females an XX pair.
Each chromosome has a structure known as a centromere that divides the chromosome into 2 arms. The short arm of the chromosome is called the “p arm” (for petite). The long arm of the chromosome is referred to as the “q arm,” because it was the next letter in the alphabet. Not very clever, but it makes it easy to remember. The location of the centromere on each chromosome can vary and is not always in the middle of the chromosome. It serves as a marker for geneticists to use in describing the location of specific genes along the chromosome arm (eg, 17q21.31 is where the BRCA1 gene is located).
Gene Structure
Much of the gene structure is broadly similar between eukaryotes and prokaryotes. The gene structure of living things such as humans (eukaryotes) is arranged individually, and for simpler prokaryotic cells, such as those in bacteria, arranged in classes. A key feature of the structure of eukaryotic genes is that their transcripts are typically subdivided into exon and intron regions. We will only discuss eukaryotes in this section.
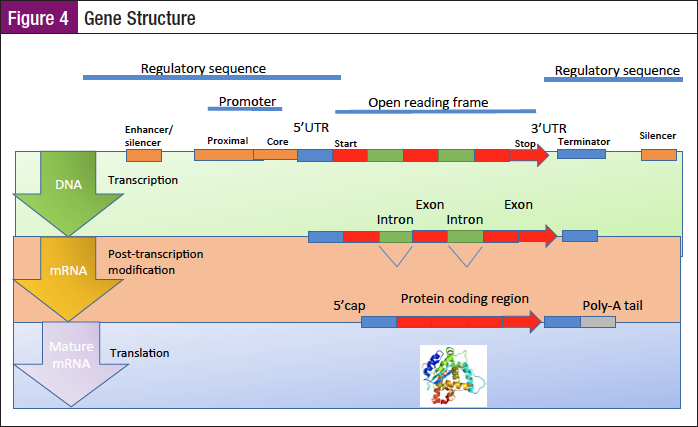
In most organisms, genes are made of DNA, where the DNA sequence determines the function of the gene. Figure 4 demonstrates each step leading to the production of a protein. A gene is transcribed or copied from DNA into RNA. Each step of the process is controlled by specific sequence elements within the gene. Every gene requires multiple sequence elements to be functional. There is a whole host of control measures in place for this process to work properly. These are known as regulatory sequences. They control when and where expression occurs for the protein coding region (red). The promoter marks the start site for transcription by binding RNA polymerase and other proteins necessary for copying DNA to RNA. Gene function uses the exons to make mature mRNA, while the introns are regions of the gene that are removed during posttranscription processing. Promoter and enhancer regions (purple) regulate the transcription of the gene into a pre-mRNA, which is modified to remove introns (green) and add a 5′ cap and poly-A tail (light grey). These additions stabilize the mRNA and direct it from the cell nucleus to the cytoplasm. The intron regions of a gene can be considerably longer than the exon regions. Once spliced together, the exons form a single continuous protein-coding region, and the splice boundaries are not detectable. The mRNA 5′ and 3′ untranslated regions (blue) regulate translation into the final protein product. These regions may be as short as a few base pairs or up to many thousands of base pairs long.13,14
Genetic Variants
A genetic condition or the susceptibility to a genetic disease is caused by a change in the DNA sequence. Specifically, this means that the letters of our genetic alphabet—A, G, C, and T—are altered or mutated from the way they should be to work properly. Some variants are inherited from the parents and are present in every cell in an individual at birth. Other diseases are caused by acquired variants in a gene or group of genes that accumulate during a person’s life.
Changes in the DNA sequence are called genetic variants. Most genetic variants do not have any effect on an individual. However, sometimes, the effect is harmful: just 1 letter missing or changed may result in the production of too little protein, extra protein, or no protein at all, which could have serious health consequences. An example of this may be the misspelling of a word and the impact it may have on cancer risk: Gray = expected; Grey = benign change (not pathogenic) but not harmful; Griy = pathogenic and potentially harmful. These genetic variants can be passed from one generation to the next, which explains why many conditions run in families, such as hereditary breast and ovarian cancer, Lynch syndrome, and Cowden syndrome. Knowing your patient’s family health history is of increasing importance since we are learning that the underlying basis for most conditions has a genetic basis. In addition, many treatments are tailored toward an individual’s specific genetic makeup (precision medicine).
Inheritance Patterns
Inheritance patterns describe how a disease is transmitted in families. These patterns help to predict the recurrence risk for relatives so they can take steps to reduce their risk or be followed by their healthcare provider differently than someone who does not have this risk. In general, inheritance patterns for single-gene disorders are classified based on whether they are autosomal or X-linked, and whether they have a dominant or recessive pattern of inheritance. These disorders are called Mendelian disorders, after the geneticist Gregor Mendel.
The most common inheritance pattern in cancer is autosomal dominant inheritance, in which only 1 copy of a disease allele is necessary for an individual to be susceptible to expressing the phenotype. For example, if a father has a genetic variant in his BRCA2 gene, he has a 50:50, or 1 in 2, chance of passing that on to each of his children, who may express it by having cancer (cancer is the phenotype, while the genetic variant is the genotype). Autosomal dominant inheritance is often called vertical inheritance because of the transmission from parent to offspring.
We see autosomal recessive inheritance more commonly in metabolic conditions or conditions like sickle cell anemia or cystic fibrosis, but very infrequently in cancer. In autosomal recessive inheritance, 2 copies of a disease allele are required for an individual to be susceptible to expressing the phenotype. Typically, the parents of an affected individual do not have the condition but are each carriers of the genetic variant. Each time a couple who are carriers of an autosomal genetic variant has a pregnancy, their chance of having children with the condition is 1 in 4 (25%) that the child will inherit 2 copies of the disease allele and will therefore have the condition; a 1 in 2 chance (50%) the child will inherit 1 copy of the disease allele and will be a carrier like the parents; or a 1 in 4 chance (25%) the child will inherit no copies of the disease allele and will not express the phenotype or be a carrier. Obviously, this individual would not be at risk for passing the disorder on to their offspring.
Identifying patterns of inheritance is the cornerstone of risk assessment. These concepts are evidenced in patient care through genetic risk assessment and genetic testing. Oncology navigators are key to facilitating and ensuring ongoing education to patients about the need to understand their family history, their risks, and the option for genetic/genomic testing.
Genetic Risk Assessment and Genetic Testing
Risk assessment and testing for hereditary predisposition has evolved considerably over the past few years due to many factors, including identification of additional genes, enhanced testing platforms, treatment implications, and greater awareness and demand by patients. It is important to understand how this process started to fully appreciate how it has rapidly evolved to allow greater numbers of at-risk patients access to risk assessment and testing. In the 1990s, testing primarily began in the academic research setting, in which individuals with cancer and their family members were part of longitudinal studies to identify genes, genetic variants, and outcomes for hereditary cancer syndromes and familial risk. In this setting, those who participated in research were typically given informed consent by genetic counselors, study coordinators, or the study’s principal investigators. Blood was drawn and samples analyzed, and depending on the protocol, results may have been given back to patients, but in some protocols they were not. This model followed the early testing model set up by the groups that investigated Huntington disease. That model included a pretest in-person visit, a second visit for a blood draw, and an in-person visit for result discussion.15 In 1995, the availability of clinical testing for BRCA1, BRCA2, and other genes led to the development of clinical risk assessment, risk prediction modeling tools, and counseling and testing services, primarily in academic medical centers. Gradually, community hospitals and other oncology services added clinically based testing to their practices utilizing a variety of delivery models given the broader indications for testing, improvements to technology making testing more accessible, and the limited number of trained genetic counselors.
Several genetic testing models exist, and new models of genetic service delivery are currently under development worldwide to address the increasing demand for accessible and efficient services. These models require the integration of genetics into all medical specialties, collaboration among different healthcare professionals, and the redistribution of professional roles. Table 1 outlines the spectrum of a few models. In the direct-to-consumer (DTC) model the healthcare provider has very little involvement, whereas the traditional model is guided and directed by the provider. Healthcare professionals are usually not involved in the process, and medical referrals are not required for genetic testing through DTC companies; thus, patients are self-referred. Furthermore, the companies usually do not offer risk assessment and genetic counseling. A middle-of-the-road option between traditional DTC is the hybrid model that allows the patient to initiate the testing process with a provider involved at some point. Genetic services led by the healthcare provider is the traditional model of genetic services (eg, for rare diseases) and remains the most common model of delivery.16,17 However, genetic applications are increasingly utilized by a wide range of healthcare professionals who are involved to various degrees in patient management (eg, surgeons, gynecologists, gastroenterologists, nurses, and many others) (Table 2). Increased demand and existing variability in the availability of trained cancer genetics experts make evaluating alternate service delivery models of high importance given the impact to patient access and care.
The delivery of genetic counseling has also evolved from the early 3-visit model for hereditary predisposition testing into a 2-visit model: a pretest, face-to-face counseling and sample collection, with a return visit (or call) several weeks later for a face-to-face or telephone result disclosure and discussion about medical management. The National Society of Genetic Counselors (NSGC), as well as other professional organizations, endorse this model for risk assessment and counseling.18-22
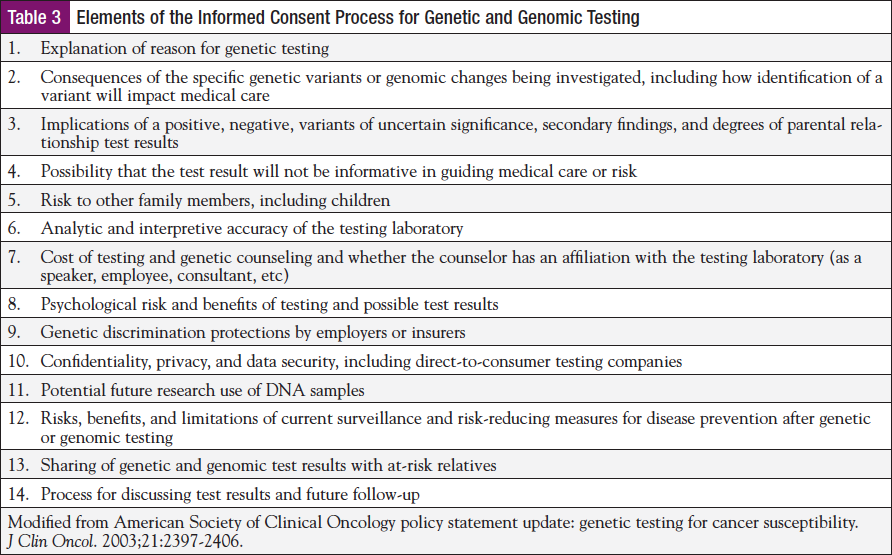
This 2-visit model is designed to provide the patient with the essential elements of the informed consent process (Table 3) and review all the possible results and their associated potential impact on medical management before testing.23,24 In addition, the pretest visit typically includes the collection of at least a 3-generation pedigree that includes cancer types and age at diagnosis. Also included in the pretest visit is the specific types of cancer and age at onset, risk assessment (sometimes aided by modeling), a discussion about the differences between sporadic and hereditary cancers, and the underlying causes of cancer (both inherited and sporadic) in the family. A plan for genetic testing is devised if appropriate, including the most informative approach; benefits and limitations of testing technology; who should be tested; accuracy of testing; and ethical, legal, and social issues associated with testing. These sessions can typically last 45 to 75 minutes.17 The face-to-face result disclosure visit typically recaps many elements of what was discussed at the pretest visit, primarily because it has been several weeks since that initial discussion, and secondarily because now that a result is in hand, a more concrete discussion of its meaning and medical management options can take place. This session typically lasts 30 to 60 minutes and allows for a discussion on the significance of the results to that patient, risk to other family members, and medical management options.17
The limited number of patients served and the time- intensiveness to support this high-touch level of genetic counseling has led to newer models that are targeted to treatment decision-making. Currently, there is an array of pretest and posttest delivery models with a variety of outcomes for patients.25,26 A few examples include a pretest upfront video followed by a face-to-face meeting, genetic counseling over the phone either for pretest, posttest, or both; or tele-education for pretest with posttest in person or over the phone.27 Some centers do all the pretests in person and all posttest discussions over the phone, with the option of coming in for a face-to-face discussion. Multiple variations exist based on staffing, resources, institutional policy, standards and guidelines followed, and provider and patient preference.
In the oncology setting, the power of genetic testing is in the treatment and management of an individual with cancer. In the noncancer setting, it can be a powerful tool to aid in the identification of an individual at risk before they get cancer so risk reduction measures can be implemented. When an individual is identified with a hereditary cancer syndrome, providers should strongly encourage the patient to share this information with their family members. Conversely, when a hereditary predisposition is not identified, it is best to encourage the patient to periodically contact their provider to share any family history updates and inquire about new information related to cancer syndromes and expanded testing opportunities. The risk for subsequent primary cancer diagnoses is significantly elevated when there is a hereditary predisposition. A new diagnosis in a family or in a patient who has had a previous diagnosis can be a sign that a hereditary predisposition is present.
The utilization of broader testing criteria and the advent of panel testing, where we can simultaneously test for multiple cancer-related genes at substantially reduced costs, forced the counseling models to evolve and focus more on the back end of testing, when a result is available. Multigene panel testing makes it impossible to provide the same type of gene-specific pretest counseling as when it was being done for 1 or 2 genes within the traditional 60-minute paradigm. The growing demand for genetics and genomics testing for cancer risk and shared treatment decision-making will continue to shift how we educate patients and still be efficient in the busy clinic setting. With the increasing number of individuals who qualify for clinical genetic testing comes added responsibility for the provision of genetics education and evaluation by various types of professionals. The expansion of genetic and genomic testing across medical specialties, and the changing workforce demographics of certified genetic counselors, have led to concerns of a workforce shortage.28,29 The traditional clinical genetics model of only a certified genetic counselor providing complete pretest and posttest evaluation and counseling cannot meet the growing volume and need for cancer genetic testing. A broad array of educational tools or programs for allied healthcare professionals and other nongenetic experts may assist in meeting the triage needs for genetic testing, as these tests become more commonplace and demand continues to grow.
Informed consent is a key component in risk assessment and genetic testing. There are several components to include in the informed consent process, as outlined in Table 3. One key worry from patients is that they will be treated unfairly because of genetic differences, which may increase their chance of developing a genetic condition.30-32 Could genetic information affect their health insurance and employment? Both state and federal governments recognize the value of genetic information for patients and healthcare providers and have established specific legal protections. In May 2008, the Genetic Information Nondiscrimination Act (GINA) was signed into law and added to the legal protections that are in place on both state and federal levels.33 GINA sets minimum protection against genetic discrimination and does not preempt state laws with stricter protections. GINA is a federal law that protects Americans from being treated unfairly because of differences in their DNA that may affect their health. This law also prevents discrimination from health insurers and employers but does not cover disability, life, or long-term care insurance. For more information on the details of GINA, please go to www.genome.gov/about-genomics/policy-issues/Genetic-Discrimination.
In 2010, the Patient Protection and Affordable Care Act (ACA)34 added additional protections by prohibiting health issuers from discriminating against patients with genetic diseases by refusing coverage because of preexisting conditions. The full ACA document can be found at www.hhs.gov/sites/default/files/patient-protection.pdf.
Genetics and Genomics in Survivorship
There has been a steady progression in patient survivorship in the arena of genetics and genomics. In 2013, the US Preventive Services Task Force provided recommendations on the use of genetic testing. In 2015, the American College of Surgeons included genetics education in their Commission on Cancer (CoC) Guidelines followed by practitioners in the United States. The NCCN continues to enhance its guidelines highlighting evidence-based and consensus recommendations for individuals who qualify for genetic counseling and testing.4,35
The National Accreditation Program for Breast Centers (NAPBC) 2018 standards require multidisciplinary breast care conferences to include discussions about genetic risk.36 Specifically, Standard 2.16: Genetic Evaluation and Management requires genetic counseling and testing services. Qualified medical professionals who can conduct these services include certified genetic counselors, genetics clinical nurses, advanced practice nurses in genetics, and nurses who are Advanced Genetics Nursing-Board Certified–credentialed through the American Nurses Credentialing Center. A credentialed clinical navigator or a trained lay navigator can assist to educate patients about genetics, provide information about genetic testing, cancer screening and cancer prevention into survivorship.36
The American Society of Clinical Oncology survivorship care plans require a familial cancer risk assessment with genetic counseling and testing.37 The Advisory Board Company has numerous discussions on survivorship care plans and meeting CoC requirements.
Professional Nursing Practice Considerations and Resources
Oncology nurses have expanded roles that include the use of genetics and genomics compared with nurses in other specialties; however, the overall role is growing across disciplines. There are many more nurses practicing in the United States than there are genetic counselors. With adequate training and access to genetic experts (eg, certified genetic counselors, medical geneticists), oncology nurses have the skill set to increase access to genetics/genomics information within their scope of nursing practice.2 Many healthcare organizations have successfully trained nurses and other qualified healthcare professionals to serve as genetic counselor extenders to meet the growing need for genetic testing.2,3,38,39 At a minimum, oncology navigators must possess sufficient knowledge to be comfortable discussing the role of genetics/genomics with their healthcare team and the patients and their families.
Updated tools, counseling models, and resources are improving how we screen, diagnose, treat, and conduct surveillance for cancer care. Genetics is at the center of it all. Genetic information may determine current and future medical management recommendations and treatments. Therefore, the best way to educate, advocate, and support our patients in real time is to empower oncology navigators on who, how, and when to refer a patient for cancer genetic risk assessment and have reliable resources for patients to ensure they receive the highest quality of care.
ISONG resources can be found at www.isong.org, and NSGC resources at www.nsgc.org/page/about-nsgc.
AONN+ genetics/genomics resources are available at www.aonnonline.org. The AONN+ Midyear and Annual Navigation & Survivorship Conferences both incorporate genetics/genomics. At this year’s Annual Conference in Nashville, TN, November 6-10, 2019, there will be a general session titled Precision Medicine for Navigators: Tissue Is the Issue.
An AONN+ national project, an initiative called BRIDGE: Building Relationships in Delivering Genetic/Genomic Education, is underway. The mission of the AONN+ BRIDGE program is to empower and engage oncology nurses and patient navigators to play a role in linking patients and personalized medicine with the ultimate goal of increasing access to genetic information for the purpose of shared decision-making. AONN+ and the BRIDGE Committee would like to thank NSGC for their support and collaboration as we embark on this educational journey.
References
- National Society of Genetic Counselors. www.nsgc.org.
- Barr JA, Tsai LP, Welch A, et al. Current practice for genetic counseling by nurses: an integrative review. Int J Nurs Pract. 2018;24:e12629.
- Cohen SA, Nixon DM. A collaborative approach to cancer risk assessment services using genetic counselor extenders in a multi-system community hospital. Breast Cancer Res Treat. 2016;159:527-534.
- Kerber AS, Ledbetter NJ. Standards of practice: applying genetics and genomics resources to oncology. Clin J Oncol Nurs. 2017;21:169-173.
- Jenkins J. Essential genetic and genomic nursing competencies for the oncology nurse. Semin Oncol Nurs. 2011;27:64-71.
- Oncology Nursing Society. 2017 Oncology Nurse Navigator Core Competencies. www.ons.org/sites/default/files/2017-05/2017_Oncology_Nurse_Navigator_Competencies.pdf.
- Academy of Oncology Nurse & Patient Navigators. Academy of Oncology Nurse & Patient Navigators Announces Standardized Navigation Metrics. https://aonnonline.org/education/articles/10-aonn-announces-standardized-navigation-metrics.
- Academy of Oncology Nurse & Patient Navigators. Oncology Nurse Navigator–Certified Generalist. www.aonnonline.org/certification/oncology-nurse-navigator-certified-generalist-onn-cg-certification. 2015.
- Cummings MR. Human Heredity: Principles and Issues. 11th ed. Cengage Learning: Boston, MA; 2016.
- National Institutes of Health. Genetics Home Reference. What is DNA? https://ghr.nlm.nih.gov/primer/basics/dna.
- National Institutes of Health. Genetics Home Reference. What is a gene? https://ghr.nlm.nih.gov/primer/basics/gene.
- National Institutes of Health. Genetics Home Reference. What is a chromosome? https://ghr.nlm.nih.gov/primer/basics/chromosome.
- Alberts B, Johnson A, Lewis J, et al. Molecular Biology of the Cell. 4th ed. New York: Garland Science; 2002.
- National Institutes of Health. Genetics Home. Reference. What is noncoding DNA? https://ghr.nlm.nih.gov/primer/basics/noncodingdna.
- International Huntington Association and the World Federation of Neurology Research Group on Huntington’s Chorea. Guidelines for the molecular genetics predictive test in Huntington’s disease. J Med Genet. 1994;31:555-559.
- Buchanan AH, Rahm AK, Williams JL. Alternate service delivery models in cancer genetic counseling: a mini-review. Front Oncol. 2016;6:120.
- Trepanier AM, Allain DC. Models of service delivery for cancer genetic risk assessment and counseling. J Genet Couns. 2014;23:239-253.
- American College of Medical Genetics. Genetic Susceptibility to Breast and Ovarian Cancer: Assessment, Counseling and Testing Guidelines. www.ncbi.nlm.nih.gov/books/NBK56955. 1999.
- Berliner JL, Fay AM. Risk assessment and genetic counseling for hereditary breast and ovarian cancer: recommendations of the National Society of Genetic Counselors. J Genet Couns. 2007;16:241-260.
- Statement of the American Society of Clinical Oncology: genetic testing for cancer susceptibility, adopted on February 20, 1996. J Clin Oncol. 1996;14:1730-1736.
- American Society of Clinical Oncology policy statement update: genetic testing for cancer susceptibility. J Clin Oncol. 2003;21:2397-2406.
- Robson ME, Storm CD, Weitzel J, et al. American Society of Clinical Oncology policy statement update: genetic and genomic testing for cancer susceptibility. J Clin Oncol. 2010;28:893-901.
- Allain D, Baker M, Blazer K, et al. Evolving models of cancer risk genetic counseling. Perspectives in Genetic Counseling. 2010;32:14-17.
- Cohen SA, Marvin ML, Riley BD, et al. Identification of genetic counseling service delivery models in practice: a report from the NSGC Service Delivery Model Task Force. J Genet Couns. 2013;22:411-421.
- Fournier DM, Bazzell AF, Dains JE. Comparing outcomes of genetic counseling options in breast and ovarian cancer: an integrative review. Oncol Nurs Forum. 2018;45:96-105.
- Cohen SA, Huziak RC, Gustafson S, Grubs RE. Analysis of advantages, limitations, and barriers of genetic counseling service delivery models. J Genet Couns. 2016;25:1010-1018.
- Rayes N, Bowen DJ, Coffin T, et al. MAGENTA (Making Genetic Testing Accessible): a prospective randomized controlled trial comparing online genetic education and telephone genetic counseling for hereditary cancer genetic testing. BMC Cancer. 2019;19:648.
- Villegas C, Haga SB. Access to genetic counselors in the southern United States. J Pers Med. 2019;9(3):33.
- Berg J, Hoskovec J, Hashmi SS, et al. Relieving the bottleneck: an investigation of barriers to expansion of supervision networks at genetic counseling training programs. J Genet Couns. 2018;27:241-251.
- Armstrong K, Calzone K, Stopfer J, et al. Factors associated with decisions about clinical BRCA1/2 testing. Cancer Epidemiol Biomarkers Prev. 2000;9:1251-1254.
- Haga SB, Barry WT, Mills R, et al. Public knowledge of and attitudes toward genetics and genetic testing. Genet Test Mol Biomarkers. 2013;17:327-335.
- Clayton EW, Halverson CM, Sathe NA, Malin BA. A systematic literature review of individuals’ perspectives on privacy and genetic information in the United States. PLoS One. 2018;13:e0204417.
- National Institutes of Health. Genetic Discrimination. www.genome.gov/about-genomics/policy-issues/Genetic-Discrimination.
- Patient Protection and Affordable Care Act. www.hhs.gov/sites/default/files/patient-protection.pdf. 2009.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines). Survivorship. Version 2.2019. www.nccn.org/professionals/physician_gls/pdf/survivorship.pdf.
- American College of Surgeons. National Accreditation Program for Breast Centers. Standards Manual 2018 Edition. https://accreditation.facs.org/accreditationdocuments/NAPBC/Portal%20Resources/2018NAPBCStandardsManual.pdf.
- American Society of Clinical Oncology. ASCO Answers: Cancer Survivorship. www.cancer.net/sites/cancer.net/files/cancer_survivorship.pdf. 2017.
- Nixon DM, Harwood CE, Kreyling G, Cohen SA. Genetic counselor extenders help meet growing demand for services. Oncology Issues. 2019;34(4):36-45.
- Blazer KR, Christie C, Uman G, Weitzel JN. Impact of web-based case conferencing on cancer genetics training outcomes for community-based clinicians. J Cancer Educ. 2012;27:217-225.